Proteus Syndrome
Radiology Cases in Pediatric Emergency Medicine
Volume 7, Case 4
Craig T. Nakamura, MD
Kapiolani Medical Center For Women And Children
University of Hawaii John A. Burns School of Medicine
This is a 16 year old female who presents to the
emergency department with a two day history of
coughing, productive for small amounts of thin, yellow
mucous. She also has two episodes of mild
hemoptysis each day (5 milliliters per episode). She
had a low grade fever and clear rhinorrhea 5 days ago,
which has resolved. She denies shortness of breath,
wheezing, chest pain, headaches, malaise, chills,
symptoms of reflux, weight loss, rashes, and joint
pains. However, she does become dyspneic with
prolonged activity. There are several family members
with rhinorrhea and low grade fevers. There is no
history of recent travel.
The patient has a history remarkable for lung cysts
of unknown etiology. At the age of 10, she developed
similar symptoms. A chest radiograph revealed
bilateral cystic changes thought to be secondary to
bronchiectasis. A follow-up film several months later
reportedly showed a progression of the right middle
lobe cyst. Bronchoscopy was normal and a TB skin
test was negative. The cyst was surgically excised.
Pathology revealed atrophic lung parenchyma lining the
cyst and chronic nonspecific inflammation. No atypical
cells were present.
Her birth history is unremarkable. A chest
radiograph from infancy was normal. Her past medical
history is significant for left hand hemihypertrophy
which was noted shortly after birth. At 5 years of age,
metal plates were placed in her left hand to retard the
hemihypertrophy. As mentioned, a chest radiograph at
10 years of age revealed cystic lung disease and she
underwent a resection of a right middle lobe cyst. Her
family history is unremarkable for pulmonary,
connective tissue, or genetic disorders.
Exam: T36.3, P 96, RR 24, BP 110/72, oxygen
saturation 91%-95% in room air. Weight 39.7 kg (<5th
percentile). Height 164 cm (70%ile).
She is a thin, well developed alert female in no
distress. Skin: No rashes, lesions, thickened skin, or
varicosities. Head: Normocephalic. EENT: Normal.
Neck: No elongation or adenopathy. Chest:
Symmetrical with normal anteroposterior diameter. No
retractions. No scoliosis or kyphosis noted. Mild
pectus excavatum is present. No tympany to
percussion. A surgical scar is noted. Lungs: Mildly
decreased breath sounds. No rhonchi, rales, or
wheeze. No prolongation of the expiratory phase.
Heart: Regular rate and rhythm. No murmur. Normal
S2. No gallop. Abdomen: Benign. No organomegaly.
Extremities: Enlarged left hand with long fingers.
There is also joint enlargement involving her left hand.
No other hemihypertrophy noted.
Arterial blood gas: pH 7.39, pCO2 40, pO2 55,
bicarbonate 24.
Review her radiographs:
Review her CXR at an early age.
 Review a later CXR.
Review a later CXR.
 Review her current CXR.
Review her current CXR.

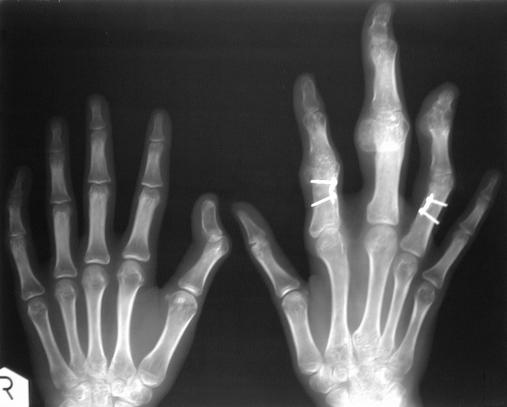
 Review her hand radiographs.
Review her hand radiographs.
 The patient was hospitalized for further evaluation of
her cystic lung disease as well as treatment of her
hypoxemia. A genetics evaluation was obtained upon
admission.
Discussion
The name, Proteus syndrome, was coined by
Wiedemann in 1983 after the Greek sea God, Proteus
(1). As the son of Poseidon, Proteus possessed the
ability to transform himself into any shape to avoid
prophesying the futures of the mortals who hounded
him. Like the Greek God, this syndrome manifests
itself in many ways. The most famous patient afflicted
with Proteus syndrome was Joseph Merrick, better
known as the "Elephant Man" (2).
Proteus syndrome is an uncommon clinical entity
characterized by abnormalities in growth (asymmetric
overgrowth, increased stature, macrodactyly, soft
tissue hypertrophy, elongated neck, macrocephaly),
skin (plantar and palmar skin thickening, epidermal
nevi, lipomas, lymphangiomas, hemangiomas, cafe au
lait spots, varicosities, dermal hypoplasia),
musculoskeletal (hemihypertrophy, bony prominences,
ankle ankylosis, craniosynostosis, mandibular
prognathia, scoliosis, pectus excavatum, thinning of the
cortical layer of long bones), eye (ptosis, strabismus,
nystagmus, myopia, colobomas, cataracts, epibulbar
dermoids, blue sclera), central nervous system
(seizures, mental retardation), venous (varicosities,
hemorrhoids, dilated superior mesenteric and
pulmonary veins) and as in this patient, cystic lung
disease (3-7).
Patients afflicted with Proteus syndrome frequently
appear normal at birth. Features begin to appear
during the first year of life with subsequent progression.
The etiology of Proteus syndrome remains unknown.
The majority of patients have a normal chromosomal
complement. However, it has been suggested that
there may be a mosaic somatic mutation affecting the
regulation of tissue growth factors, leading to the
associated polymorphic characteristics of this disease
(8-12). We will focus on the pulmonary disease and
chest radiographic findings associated with Proteus
syndrome.
The most striking radiographic finding are cystic
lung lesions (1,2,5,13). These cysts can be quite large
and may be distributed unilaterally or bilaterally. There
is no preference for any particular lobe to be involved.
Another reported finding is the prominence of
pulmonary markings with obstructive lung parenchymal
changes (4). The chest radiograph may also reveal
dilated pulmonary veins, scoliosis (2), kyphosis (4),
dysplastic or enlarged thoracic vertebrae (14), rib
hypertrophy (12,15), and soft tissue masses (16).
The differential of cystic lung disease includes
bronchopulmonary dysplasia (17), bronchogenic cysts
(18), Marfan syndrome (19,20), neurofibromatosis (21),
tuberous sclerosis (22), bronchiectasis,
pneumatoceles, pneumoconiosis, alpha-1-antitrypsin
deficiency (23), cystic adenomatoid malformation (24),
histiocytosis X (25), and sarcoidosis (26).
The morbidity and mortality risk of pulmonary cysts
in Proteus syndrome is unknown. Treatment generally
focuses on minimizing further lung damage and
avoiding infection of the cysts to prevent respiratory
compromise. If these attempts prove to be
unsuccessful, lung transplantation may be an option
(5,27). In the future, further efforts may be made to
further delineate the exact etiology of this syndrome,
which may suggest alternate forms of therapy.
References.
1. Wiedemann HR, Burgio GR, Aldenhoff P, Kunze
J, Kaufmann HG, Schirg E. The proteus syndrome.
European Journal of Pediatrics 1983;140:5-12.
2. Tibbles JAR, Cohen MM Jr. The proteus
syndrome: The elephant man diagnosed. British
Medical Journal 1986;293:683-685.
3. Proteus Syndrome. In: Jones KL. Smith's
Recognizable Patterns of Human Malformation. 4th
edition. Philadelphia, PA, W.B. Saunders, 1988,
pp. 458-459.
4. Barona-Mazuera M, Hidalgo-Galvan LR,
Orozco-Covarrubias M, Duran-McKinster C,
Tamayo-Sanchez L, Ruiz-Maldonado R. Proteus
syndrome: New findings in seven patients. Pediatric
Dermatology 1997;14(1):1-5.
5. Fay JT, Schow SR. A possible cause of
Maffucci's syndrome: Report of a case. J Oral Surg
1968;26:739-744.
6. Newman B, Urbach AH, Orenstein D, Dickman
PS. Proteus syndrome: Emphasis on the pulmonary
manifestations. Pediatric Radiology 1994;24:189-193.
7. Happle R, Steijlen PM, Theile U, Karitzky D,
Tinschert S, Albrecht-Nebe H, Kuster W. Patchy
dermal hypoplasia as a characteristic feature of
Proteus syndrome. Arch Dermatol 1997;133:77-80.
8. Lezama DB, Buyse ML. The proteus syndrome:
The emergence of an entity. J Clin Dysmorphol
1984;2:10-13.
9. Samlaska CP, Levin SW, James WD, Benson
PM, Walker JC, Perlik PC. Proteus syndrome. Arch
Dermatol 1989;125:1109.
10. Say B, Carpenter NJ. Report of a case
resembling the Proteus syndrome with a chromosome
abnormality. Am J Med Genet 1988;31:987-989.
11. Happle R. Lethal genes surviving by
mosaicism: A possible explanation for sporadic birth
defects involving the skin. Am Acad Dermatol
1987;16:899-906.
12. Clark RD, Donnai D, Rogers J, Cooper J,
Baraitser M. Proteus syndrome: An expanded
phenotype. Am J Med Genet 1987; 27:99-117.
13. Bender BL, Unis E. Fibrocartilaginous lesions
of bone and hemangiomas and lipomas of soft tissue
resembling Maffucci's syndrome. J Bone Joint Surg
1979;61:1104-1108.
14. Azouz EM, Costa T, Fitch N. Radiologic
findings in the Proteus syndrome. Pediatric Radiology
1987;17:481-485.
15. Cremin BJ, Viljoen DL, Wynchank S, Beighton
P. The Proteus syndrome: The magnetic resonance
and radiological features. Pediatric Radiology
1987;17:486-488.
16. Bialer MG, Riedy MJ, Wilson WG. Proteus
syndrome versus Bannayan-Zonana syndrome: A
problem in differential diagnosis. Eur J Pediatr
1988;148:122-125.
17. Karmazin N, Panitch HB, Balsara RK, Faerber
EN, de Chadarevian JP. De novo circumscribed
pulmonary lobar cystic anomaly in a young boy. A
possible sequela of bronchopulmonary dysplasia.
Chest 1989;95(5):1162-1163.
18. Raymond GS, Logan PM. Congenital thoracic
masses: Imaging features in the adult. Crit Rev Diagn
Imaging 1997;38(2):115-205.
19. Wood JR, Bellamy D, Child AH, Citron KM.
Pulmonary disease in patients with Marfan syndrome.
Thorax 1984;39:780-784.
20. Day DL, Burke BA. Pulmonary emphysema in
a neonate with Marfan syndrome. Pediatric Radiology
1986;16:518-521.
21. Webb WR, Goodman PC. Fibrosing alveolitis
in patients with neurofibromatosis. Radiology
1977;122:289-293.
22. Dwyer JM, Hickie JB, Garvan J. Pulmonary
tuberous sclerosis. Report of three patients and a
review of the literature. Quart J Med 1971;40:115-125.
23. Eriksson S. Studies in alpha-1-antitrypsin
deficiency. Acta Med Scand 1965;432(suppl):1-85.
24. Nokes SR, Pierce WB. Radiological case of
the month. Cystic adenomatoid malformation. J Ark
Med Soc 1996;92(9):469-470.
25. Smith M, McCormack LJ, Van Ordstrand HS,
Effler DB, Groves LK. "Primary" pulmonary
histiocytosis X. Chest 1974;65:176-180.
26. Ellis K, Renthal G. Pulmonary sarcoidosis:
Roentgenographic observations on course of disease.
Am J Roentgenol 1962;88:11070-1083.
27. Armitage JM, Kurland G, Michaels M, Cipriani
LA, Griffith BP, Fricker F. Critical issues in pediatric
lung transplantation. Journal of Thoracic and
Cardiovascular Surgery 1995;109(1): 60-65.
The patient was hospitalized for further evaluation of
her cystic lung disease as well as treatment of her
hypoxemia. A genetics evaluation was obtained upon
admission.
Discussion
The name, Proteus syndrome, was coined by
Wiedemann in 1983 after the Greek sea God, Proteus
(1). As the son of Poseidon, Proteus possessed the
ability to transform himself into any shape to avoid
prophesying the futures of the mortals who hounded
him. Like the Greek God, this syndrome manifests
itself in many ways. The most famous patient afflicted
with Proteus syndrome was Joseph Merrick, better
known as the "Elephant Man" (2).
Proteus syndrome is an uncommon clinical entity
characterized by abnormalities in growth (asymmetric
overgrowth, increased stature, macrodactyly, soft
tissue hypertrophy, elongated neck, macrocephaly),
skin (plantar and palmar skin thickening, epidermal
nevi, lipomas, lymphangiomas, hemangiomas, cafe au
lait spots, varicosities, dermal hypoplasia),
musculoskeletal (hemihypertrophy, bony prominences,
ankle ankylosis, craniosynostosis, mandibular
prognathia, scoliosis, pectus excavatum, thinning of the
cortical layer of long bones), eye (ptosis, strabismus,
nystagmus, myopia, colobomas, cataracts, epibulbar
dermoids, blue sclera), central nervous system
(seizures, mental retardation), venous (varicosities,
hemorrhoids, dilated superior mesenteric and
pulmonary veins) and as in this patient, cystic lung
disease (3-7).
Patients afflicted with Proteus syndrome frequently
appear normal at birth. Features begin to appear
during the first year of life with subsequent progression.
The etiology of Proteus syndrome remains unknown.
The majority of patients have a normal chromosomal
complement. However, it has been suggested that
there may be a mosaic somatic mutation affecting the
regulation of tissue growth factors, leading to the
associated polymorphic characteristics of this disease
(8-12). We will focus on the pulmonary disease and
chest radiographic findings associated with Proteus
syndrome.
The most striking radiographic finding are cystic
lung lesions (1,2,5,13). These cysts can be quite large
and may be distributed unilaterally or bilaterally. There
is no preference for any particular lobe to be involved.
Another reported finding is the prominence of
pulmonary markings with obstructive lung parenchymal
changes (4). The chest radiograph may also reveal
dilated pulmonary veins, scoliosis (2), kyphosis (4),
dysplastic or enlarged thoracic vertebrae (14), rib
hypertrophy (12,15), and soft tissue masses (16).
The differential of cystic lung disease includes
bronchopulmonary dysplasia (17), bronchogenic cysts
(18), Marfan syndrome (19,20), neurofibromatosis (21),
tuberous sclerosis (22), bronchiectasis,
pneumatoceles, pneumoconiosis, alpha-1-antitrypsin
deficiency (23), cystic adenomatoid malformation (24),
histiocytosis X (25), and sarcoidosis (26).
The morbidity and mortality risk of pulmonary cysts
in Proteus syndrome is unknown. Treatment generally
focuses on minimizing further lung damage and
avoiding infection of the cysts to prevent respiratory
compromise. If these attempts prove to be
unsuccessful, lung transplantation may be an option
(5,27). In the future, further efforts may be made to
further delineate the exact etiology of this syndrome,
which may suggest alternate forms of therapy.
References.
1. Wiedemann HR, Burgio GR, Aldenhoff P, Kunze
J, Kaufmann HG, Schirg E. The proteus syndrome.
European Journal of Pediatrics 1983;140:5-12.
2. Tibbles JAR, Cohen MM Jr. The proteus
syndrome: The elephant man diagnosed. British
Medical Journal 1986;293:683-685.
3. Proteus Syndrome. In: Jones KL. Smith's
Recognizable Patterns of Human Malformation. 4th
edition. Philadelphia, PA, W.B. Saunders, 1988,
pp. 458-459.
4. Barona-Mazuera M, Hidalgo-Galvan LR,
Orozco-Covarrubias M, Duran-McKinster C,
Tamayo-Sanchez L, Ruiz-Maldonado R. Proteus
syndrome: New findings in seven patients. Pediatric
Dermatology 1997;14(1):1-5.
5. Fay JT, Schow SR. A possible cause of
Maffucci's syndrome: Report of a case. J Oral Surg
1968;26:739-744.
6. Newman B, Urbach AH, Orenstein D, Dickman
PS. Proteus syndrome: Emphasis on the pulmonary
manifestations. Pediatric Radiology 1994;24:189-193.
7. Happle R, Steijlen PM, Theile U, Karitzky D,
Tinschert S, Albrecht-Nebe H, Kuster W. Patchy
dermal hypoplasia as a characteristic feature of
Proteus syndrome. Arch Dermatol 1997;133:77-80.
8. Lezama DB, Buyse ML. The proteus syndrome:
The emergence of an entity. J Clin Dysmorphol
1984;2:10-13.
9. Samlaska CP, Levin SW, James WD, Benson
PM, Walker JC, Perlik PC. Proteus syndrome. Arch
Dermatol 1989;125:1109.
10. Say B, Carpenter NJ. Report of a case
resembling the Proteus syndrome with a chromosome
abnormality. Am J Med Genet 1988;31:987-989.
11. Happle R. Lethal genes surviving by
mosaicism: A possible explanation for sporadic birth
defects involving the skin. Am Acad Dermatol
1987;16:899-906.
12. Clark RD, Donnai D, Rogers J, Cooper J,
Baraitser M. Proteus syndrome: An expanded
phenotype. Am J Med Genet 1987; 27:99-117.
13. Bender BL, Unis E. Fibrocartilaginous lesions
of bone and hemangiomas and lipomas of soft tissue
resembling Maffucci's syndrome. J Bone Joint Surg
1979;61:1104-1108.
14. Azouz EM, Costa T, Fitch N. Radiologic
findings in the Proteus syndrome. Pediatric Radiology
1987;17:481-485.
15. Cremin BJ, Viljoen DL, Wynchank S, Beighton
P. The Proteus syndrome: The magnetic resonance
and radiological features. Pediatric Radiology
1987;17:486-488.
16. Bialer MG, Riedy MJ, Wilson WG. Proteus
syndrome versus Bannayan-Zonana syndrome: A
problem in differential diagnosis. Eur J Pediatr
1988;148:122-125.
17. Karmazin N, Panitch HB, Balsara RK, Faerber
EN, de Chadarevian JP. De novo circumscribed
pulmonary lobar cystic anomaly in a young boy. A
possible sequela of bronchopulmonary dysplasia.
Chest 1989;95(5):1162-1163.
18. Raymond GS, Logan PM. Congenital thoracic
masses: Imaging features in the adult. Crit Rev Diagn
Imaging 1997;38(2):115-205.
19. Wood JR, Bellamy D, Child AH, Citron KM.
Pulmonary disease in patients with Marfan syndrome.
Thorax 1984;39:780-784.
20. Day DL, Burke BA. Pulmonary emphysema in
a neonate with Marfan syndrome. Pediatric Radiology
1986;16:518-521.
21. Webb WR, Goodman PC. Fibrosing alveolitis
in patients with neurofibromatosis. Radiology
1977;122:289-293.
22. Dwyer JM, Hickie JB, Garvan J. Pulmonary
tuberous sclerosis. Report of three patients and a
review of the literature. Quart J Med 1971;40:115-125.
23. Eriksson S. Studies in alpha-1-antitrypsin
deficiency. Acta Med Scand 1965;432(suppl):1-85.
24. Nokes SR, Pierce WB. Radiological case of
the month. Cystic adenomatoid malformation. J Ark
Med Soc 1996;92(9):469-470.
25. Smith M, McCormack LJ, Van Ordstrand HS,
Effler DB, Groves LK. "Primary" pulmonary
histiocytosis X. Chest 1974;65:176-180.
26. Ellis K, Renthal G. Pulmonary sarcoidosis:
Roentgenographic observations on course of disease.
Am J Roentgenol 1962;88:11070-1083.
27. Armitage JM, Kurland G, Michaels M, Cipriani
LA, Griffith BP, Fricker F. Critical issues in pediatric
lung transplantation. Journal of Thoracic and
Cardiovascular Surgery 1995;109(1): 60-65.
Return to Radiology Cases In Ped Emerg Med Case Selection Page
Return to Univ. Hawaii Dept. Pediatrics Home Page
 Review a later CXR.
Review a later CXR.
 Review her current CXR.
Review her current CXR.

 Review her hand radiographs.
Review her hand radiographs.
 The patient was hospitalized for further evaluation of
her cystic lung disease as well as treatment of her
hypoxemia. A genetics evaluation was obtained upon
admission.
Discussion
The name, Proteus syndrome, was coined by
Wiedemann in 1983 after the Greek sea God, Proteus
(1). As the son of Poseidon, Proteus possessed the
ability to transform himself into any shape to avoid
prophesying the futures of the mortals who hounded
him. Like the Greek God, this syndrome manifests
itself in many ways. The most famous patient afflicted
with Proteus syndrome was Joseph Merrick, better
known as the "Elephant Man" (2).
Proteus syndrome is an uncommon clinical entity
characterized by abnormalities in growth (asymmetric
overgrowth, increased stature, macrodactyly, soft
tissue hypertrophy, elongated neck, macrocephaly),
skin (plantar and palmar skin thickening, epidermal
nevi, lipomas, lymphangiomas, hemangiomas, cafe au
lait spots, varicosities, dermal hypoplasia),
musculoskeletal (hemihypertrophy, bony prominences,
ankle ankylosis, craniosynostosis, mandibular
prognathia, scoliosis, pectus excavatum, thinning of the
cortical layer of long bones), eye (ptosis, strabismus,
nystagmus, myopia, colobomas, cataracts, epibulbar
dermoids, blue sclera), central nervous system
(seizures, mental retardation), venous (varicosities,
hemorrhoids, dilated superior mesenteric and
pulmonary veins) and as in this patient, cystic lung
disease (3-7).
Patients afflicted with Proteus syndrome frequently
appear normal at birth. Features begin to appear
during the first year of life with subsequent progression.
The etiology of Proteus syndrome remains unknown.
The majority of patients have a normal chromosomal
complement. However, it has been suggested that
there may be a mosaic somatic mutation affecting the
regulation of tissue growth factors, leading to the
associated polymorphic characteristics of this disease
(8-12). We will focus on the pulmonary disease and
chest radiographic findings associated with Proteus
syndrome.
The most striking radiographic finding are cystic
lung lesions (1,2,5,13). These cysts can be quite large
and may be distributed unilaterally or bilaterally. There
is no preference for any particular lobe to be involved.
Another reported finding is the prominence of
pulmonary markings with obstructive lung parenchymal
changes (4). The chest radiograph may also reveal
dilated pulmonary veins, scoliosis (2), kyphosis (4),
dysplastic or enlarged thoracic vertebrae (14), rib
hypertrophy (12,15), and soft tissue masses (16).
The differential of cystic lung disease includes
bronchopulmonary dysplasia (17), bronchogenic cysts
(18), Marfan syndrome (19,20), neurofibromatosis (21),
tuberous sclerosis (22), bronchiectasis,
pneumatoceles, pneumoconiosis, alpha-1-antitrypsin
deficiency (23), cystic adenomatoid malformation (24),
histiocytosis X (25), and sarcoidosis (26).
The morbidity and mortality risk of pulmonary cysts
in Proteus syndrome is unknown. Treatment generally
focuses on minimizing further lung damage and
avoiding infection of the cysts to prevent respiratory
compromise. If these attempts prove to be
unsuccessful, lung transplantation may be an option
(5,27). In the future, further efforts may be made to
further delineate the exact etiology of this syndrome,
which may suggest alternate forms of therapy.
References.
1. Wiedemann HR, Burgio GR, Aldenhoff P, Kunze
J, Kaufmann HG, Schirg E. The proteus syndrome.
European Journal of Pediatrics 1983;140:5-12.
2. Tibbles JAR, Cohen MM Jr. The proteus
syndrome: The elephant man diagnosed. British
Medical Journal 1986;293:683-685.
3. Proteus Syndrome. In: Jones KL. Smith's
Recognizable Patterns of Human Malformation. 4th
edition. Philadelphia, PA, W.B. Saunders, 1988,
pp. 458-459.
4. Barona-Mazuera M, Hidalgo-Galvan LR,
Orozco-Covarrubias M, Duran-McKinster C,
Tamayo-Sanchez L, Ruiz-Maldonado R. Proteus
syndrome: New findings in seven patients. Pediatric
Dermatology 1997;14(1):1-5.
5. Fay JT, Schow SR. A possible cause of
Maffucci's syndrome: Report of a case. J Oral Surg
1968;26:739-744.
6. Newman B, Urbach AH, Orenstein D, Dickman
PS. Proteus syndrome: Emphasis on the pulmonary
manifestations. Pediatric Radiology 1994;24:189-193.
7. Happle R, Steijlen PM, Theile U, Karitzky D,
Tinschert S, Albrecht-Nebe H, Kuster W. Patchy
dermal hypoplasia as a characteristic feature of
Proteus syndrome. Arch Dermatol 1997;133:77-80.
8. Lezama DB, Buyse ML. The proteus syndrome:
The emergence of an entity. J Clin Dysmorphol
1984;2:10-13.
9. Samlaska CP, Levin SW, James WD, Benson
PM, Walker JC, Perlik PC. Proteus syndrome. Arch
Dermatol 1989;125:1109.
10. Say B, Carpenter NJ. Report of a case
resembling the Proteus syndrome with a chromosome
abnormality. Am J Med Genet 1988;31:987-989.
11. Happle R. Lethal genes surviving by
mosaicism: A possible explanation for sporadic birth
defects involving the skin. Am Acad Dermatol
1987;16:899-906.
12. Clark RD, Donnai D, Rogers J, Cooper J,
Baraitser M. Proteus syndrome: An expanded
phenotype. Am J Med Genet 1987; 27:99-117.
13. Bender BL, Unis E. Fibrocartilaginous lesions
of bone and hemangiomas and lipomas of soft tissue
resembling Maffucci's syndrome. J Bone Joint Surg
1979;61:1104-1108.
14. Azouz EM, Costa T, Fitch N. Radiologic
findings in the Proteus syndrome. Pediatric Radiology
1987;17:481-485.
15. Cremin BJ, Viljoen DL, Wynchank S, Beighton
P. The Proteus syndrome: The magnetic resonance
and radiological features. Pediatric Radiology
1987;17:486-488.
16. Bialer MG, Riedy MJ, Wilson WG. Proteus
syndrome versus Bannayan-Zonana syndrome: A
problem in differential diagnosis. Eur J Pediatr
1988;148:122-125.
17. Karmazin N, Panitch HB, Balsara RK, Faerber
EN, de Chadarevian JP. De novo circumscribed
pulmonary lobar cystic anomaly in a young boy. A
possible sequela of bronchopulmonary dysplasia.
Chest 1989;95(5):1162-1163.
18. Raymond GS, Logan PM. Congenital thoracic
masses: Imaging features in the adult. Crit Rev Diagn
Imaging 1997;38(2):115-205.
19. Wood JR, Bellamy D, Child AH, Citron KM.
Pulmonary disease in patients with Marfan syndrome.
Thorax 1984;39:780-784.
20. Day DL, Burke BA. Pulmonary emphysema in
a neonate with Marfan syndrome. Pediatric Radiology
1986;16:518-521.
21. Webb WR, Goodman PC. Fibrosing alveolitis
in patients with neurofibromatosis. Radiology
1977;122:289-293.
22. Dwyer JM, Hickie JB, Garvan J. Pulmonary
tuberous sclerosis. Report of three patients and a
review of the literature. Quart J Med 1971;40:115-125.
23. Eriksson S. Studies in alpha-1-antitrypsin
deficiency. Acta Med Scand 1965;432(suppl):1-85.
24. Nokes SR, Pierce WB. Radiological case of
the month. Cystic adenomatoid malformation. J Ark
Med Soc 1996;92(9):469-470.
25. Smith M, McCormack LJ, Van Ordstrand HS,
Effler DB, Groves LK. "Primary" pulmonary
histiocytosis X. Chest 1974;65:176-180.
26. Ellis K, Renthal G. Pulmonary sarcoidosis:
Roentgenographic observations on course of disease.
Am J Roentgenol 1962;88:11070-1083.
27. Armitage JM, Kurland G, Michaels M, Cipriani
LA, Griffith BP, Fricker F. Critical issues in pediatric
lung transplantation. Journal of Thoracic and
Cardiovascular Surgery 1995;109(1): 60-65.
The patient was hospitalized for further evaluation of
her cystic lung disease as well as treatment of her
hypoxemia. A genetics evaluation was obtained upon
admission.
Discussion
The name, Proteus syndrome, was coined by
Wiedemann in 1983 after the Greek sea God, Proteus
(1). As the son of Poseidon, Proteus possessed the
ability to transform himself into any shape to avoid
prophesying the futures of the mortals who hounded
him. Like the Greek God, this syndrome manifests
itself in many ways. The most famous patient afflicted
with Proteus syndrome was Joseph Merrick, better
known as the "Elephant Man" (2).
Proteus syndrome is an uncommon clinical entity
characterized by abnormalities in growth (asymmetric
overgrowth, increased stature, macrodactyly, soft
tissue hypertrophy, elongated neck, macrocephaly),
skin (plantar and palmar skin thickening, epidermal
nevi, lipomas, lymphangiomas, hemangiomas, cafe au
lait spots, varicosities, dermal hypoplasia),
musculoskeletal (hemihypertrophy, bony prominences,
ankle ankylosis, craniosynostosis, mandibular
prognathia, scoliosis, pectus excavatum, thinning of the
cortical layer of long bones), eye (ptosis, strabismus,
nystagmus, myopia, colobomas, cataracts, epibulbar
dermoids, blue sclera), central nervous system
(seizures, mental retardation), venous (varicosities,
hemorrhoids, dilated superior mesenteric and
pulmonary veins) and as in this patient, cystic lung
disease (3-7).
Patients afflicted with Proteus syndrome frequently
appear normal at birth. Features begin to appear
during the first year of life with subsequent progression.
The etiology of Proteus syndrome remains unknown.
The majority of patients have a normal chromosomal
complement. However, it has been suggested that
there may be a mosaic somatic mutation affecting the
regulation of tissue growth factors, leading to the
associated polymorphic characteristics of this disease
(8-12). We will focus on the pulmonary disease and
chest radiographic findings associated with Proteus
syndrome.
The most striking radiographic finding are cystic
lung lesions (1,2,5,13). These cysts can be quite large
and may be distributed unilaterally or bilaterally. There
is no preference for any particular lobe to be involved.
Another reported finding is the prominence of
pulmonary markings with obstructive lung parenchymal
changes (4). The chest radiograph may also reveal
dilated pulmonary veins, scoliosis (2), kyphosis (4),
dysplastic or enlarged thoracic vertebrae (14), rib
hypertrophy (12,15), and soft tissue masses (16).
The differential of cystic lung disease includes
bronchopulmonary dysplasia (17), bronchogenic cysts
(18), Marfan syndrome (19,20), neurofibromatosis (21),
tuberous sclerosis (22), bronchiectasis,
pneumatoceles, pneumoconiosis, alpha-1-antitrypsin
deficiency (23), cystic adenomatoid malformation (24),
histiocytosis X (25), and sarcoidosis (26).
The morbidity and mortality risk of pulmonary cysts
in Proteus syndrome is unknown. Treatment generally
focuses on minimizing further lung damage and
avoiding infection of the cysts to prevent respiratory
compromise. If these attempts prove to be
unsuccessful, lung transplantation may be an option
(5,27). In the future, further efforts may be made to
further delineate the exact etiology of this syndrome,
which may suggest alternate forms of therapy.
References.
1. Wiedemann HR, Burgio GR, Aldenhoff P, Kunze
J, Kaufmann HG, Schirg E. The proteus syndrome.
European Journal of Pediatrics 1983;140:5-12.
2. Tibbles JAR, Cohen MM Jr. The proteus
syndrome: The elephant man diagnosed. British
Medical Journal 1986;293:683-685.
3. Proteus Syndrome. In: Jones KL. Smith's
Recognizable Patterns of Human Malformation. 4th
edition. Philadelphia, PA, W.B. Saunders, 1988,
pp. 458-459.
4. Barona-Mazuera M, Hidalgo-Galvan LR,
Orozco-Covarrubias M, Duran-McKinster C,
Tamayo-Sanchez L, Ruiz-Maldonado R. Proteus
syndrome: New findings in seven patients. Pediatric
Dermatology 1997;14(1):1-5.
5. Fay JT, Schow SR. A possible cause of
Maffucci's syndrome: Report of a case. J Oral Surg
1968;26:739-744.
6. Newman B, Urbach AH, Orenstein D, Dickman
PS. Proteus syndrome: Emphasis on the pulmonary
manifestations. Pediatric Radiology 1994;24:189-193.
7. Happle R, Steijlen PM, Theile U, Karitzky D,
Tinschert S, Albrecht-Nebe H, Kuster W. Patchy
dermal hypoplasia as a characteristic feature of
Proteus syndrome. Arch Dermatol 1997;133:77-80.
8. Lezama DB, Buyse ML. The proteus syndrome:
The emergence of an entity. J Clin Dysmorphol
1984;2:10-13.
9. Samlaska CP, Levin SW, James WD, Benson
PM, Walker JC, Perlik PC. Proteus syndrome. Arch
Dermatol 1989;125:1109.
10. Say B, Carpenter NJ. Report of a case
resembling the Proteus syndrome with a chromosome
abnormality. Am J Med Genet 1988;31:987-989.
11. Happle R. Lethal genes surviving by
mosaicism: A possible explanation for sporadic birth
defects involving the skin. Am Acad Dermatol
1987;16:899-906.
12. Clark RD, Donnai D, Rogers J, Cooper J,
Baraitser M. Proteus syndrome: An expanded
phenotype. Am J Med Genet 1987; 27:99-117.
13. Bender BL, Unis E. Fibrocartilaginous lesions
of bone and hemangiomas and lipomas of soft tissue
resembling Maffucci's syndrome. J Bone Joint Surg
1979;61:1104-1108.
14. Azouz EM, Costa T, Fitch N. Radiologic
findings in the Proteus syndrome. Pediatric Radiology
1987;17:481-485.
15. Cremin BJ, Viljoen DL, Wynchank S, Beighton
P. The Proteus syndrome: The magnetic resonance
and radiological features. Pediatric Radiology
1987;17:486-488.
16. Bialer MG, Riedy MJ, Wilson WG. Proteus
syndrome versus Bannayan-Zonana syndrome: A
problem in differential diagnosis. Eur J Pediatr
1988;148:122-125.
17. Karmazin N, Panitch HB, Balsara RK, Faerber
EN, de Chadarevian JP. De novo circumscribed
pulmonary lobar cystic anomaly in a young boy. A
possible sequela of bronchopulmonary dysplasia.
Chest 1989;95(5):1162-1163.
18. Raymond GS, Logan PM. Congenital thoracic
masses: Imaging features in the adult. Crit Rev Diagn
Imaging 1997;38(2):115-205.
19. Wood JR, Bellamy D, Child AH, Citron KM.
Pulmonary disease in patients with Marfan syndrome.
Thorax 1984;39:780-784.
20. Day DL, Burke BA. Pulmonary emphysema in
a neonate with Marfan syndrome. Pediatric Radiology
1986;16:518-521.
21. Webb WR, Goodman PC. Fibrosing alveolitis
in patients with neurofibromatosis. Radiology
1977;122:289-293.
22. Dwyer JM, Hickie JB, Garvan J. Pulmonary
tuberous sclerosis. Report of three patients and a
review of the literature. Quart J Med 1971;40:115-125.
23. Eriksson S. Studies in alpha-1-antitrypsin
deficiency. Acta Med Scand 1965;432(suppl):1-85.
24. Nokes SR, Pierce WB. Radiological case of
the month. Cystic adenomatoid malformation. J Ark
Med Soc 1996;92(9):469-470.
25. Smith M, McCormack LJ, Van Ordstrand HS,
Effler DB, Groves LK. "Primary" pulmonary
histiocytosis X. Chest 1974;65:176-180.
26. Ellis K, Renthal G. Pulmonary sarcoidosis:
Roentgenographic observations on course of disease.
Am J Roentgenol 1962;88:11070-1083.
27. Armitage JM, Kurland G, Michaels M, Cipriani
LA, Griffith BP, Fricker F. Critical issues in pediatric
lung transplantation. Journal of Thoracic and
Cardiovascular Surgery 1995;109(1): 60-65.