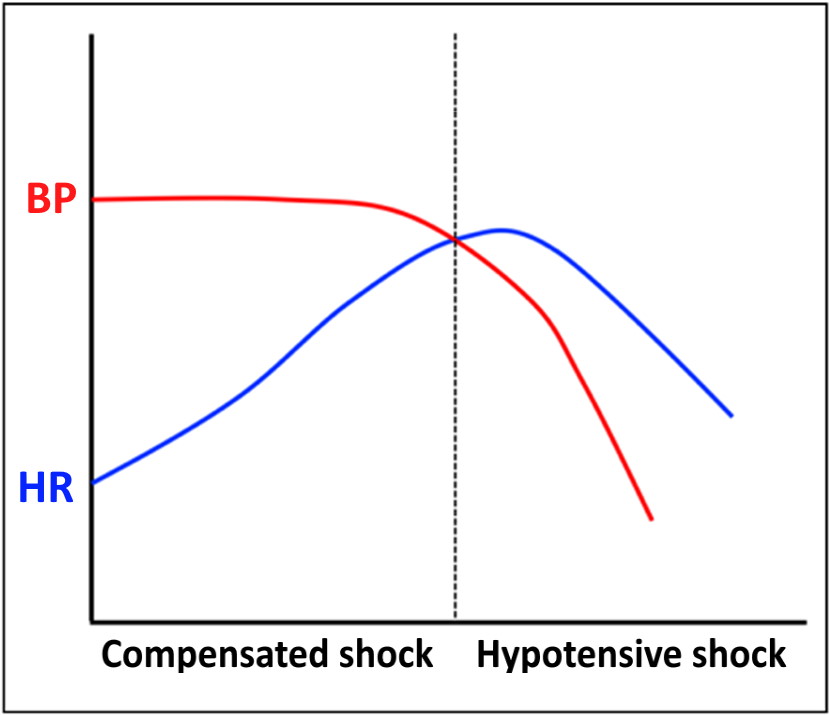
Figure 1. Compensated versus hypotensive shock. HR can compensate to maintain BP to a point at which it can no longer sufficiently compensate to maintain BP, resulting in hypotension.

The editors and current author would like to thank and acknowledge the significant contribution of the previous author of this chapter from the 2004 first edition Dr. Rodney B. Boychuk. This current third edition chapter is a revision and update of the original author’s work.
Case 1:
This is a 12-month-old male infant with a 4-day history of vomiting and diarrhea who was brought to the emergency department by his mother. On the initial exam, the patient’s airway is patent and breath sounds are heard with a respiratory rate of 70 breaths per minute with mild subcostal retractions. Oxygen saturation (SpO2) is 99% on room air.
The infant is lethargic, does not respond well to his parents, and responds to pain only with a minimal grimace. Central pulses are poor, peripheral pulses are diminished, and extremities are cool. Feeling from the 5th toe upwards, the legs are cool to the touch up to the knee. Capillary refill time (CRT) is 8 seconds. Heart rate is 209 beats per minute, and blood pressure is 60 mmHg systolic.
On ECG there are narrow QRS complexes with sinus tachycardia on the monitor.
You are unable to start an IV line. 100% oxygen via a nonrebreather mask is started. The mucous membranes of the mouth are pink. An intraosseous (IO) is placed in the left tibia and 20cc/kg of normal saline is infused as rapidly as possible. The infant is reassessed. Airway remains patent, and the work of breathing appears more relaxed. The heart rate is now 195. A repeat bolus of 20cc/kg is given, and the patient is reassessed. After the 3rd fluid bolus is given, distal pulses become more palpable, his heart rate comes down to 160, and the patient becomes more alert. However, a rapid bedside glucose analysis reveals a blood sugar of only 50, which is quickly treated with an IV dextrose bolus.
This case represents a patient in hypotensive, hypovolemic shock (and hypoglycemia) secondary to vomiting and diarrhea.
Case 2:
A 12-year-old girl presents with the chief complaint of respiratory distress and lethargy over the past 18 hours. Parents state that this morning she didn’t feel well. Initial respiratory rate is 40 breaths per minute. Lung exam is notable for tachypnea, slight subcostal retractions and nasal flaring. Aeration is good bilaterally and with faint, fine crackles over the lung bases. No wheezing is appreciated. She is arousable but difficult to maintain attention, poorly following commands, and not particularly bothered by peripheral IV insertion. Cardiac exam is notable for significant tachycardia with a HR of 150, BP 75/35, mean arterial pressure (MAP) 48. Radial pulses are weak, femoral pulses palpable, fair. Hands and feet feel cool to touch. CRT is 5 seconds in the fingers and toes, 4 seconds over the sternum. Abdominal exam is without tenderness or distention. A liver edge is noted to be 5 cm below the right costal margin. Neurologically, she appears to be moving all of her extremities with mild grimacing, weak speech, and localized flexion withdrawal to pinching. Pupils are 4 mm in diameter and are briskly reactive to light. Skin exam unremarkable for any rash.
This case represents a patient in hypotensive, cardiogenic shock.
Shock is a clinical syndrome of circulatory dysfunction resulting in inadequate oxygen delivery with the inability to meet the metabolic demands of the tissues (cells). This results in a cascade of events resulting in altered cellular metabolism and function; and ultimately death. Hypotension is a late finding in pediatric patients. Within the pediatric population, the definition of hypotension varies by age:
| Infants 0 to 1 month of age | systolic pressure <60 mmHg |
| For infants 1 to 12 months of age | systolic pressure <70 mmHg |
| In children 1 to 10 years of age | systolic pressure < (70 mmHg + [child's age in years x 2]) |
| Children >10 years of age | systolic pressure <90 mmHg |
Hypotensive shock is when the body is no longer able to compensate for the losses in perfusion, resulting in hypotension and poor perfusion.
The most common cause of shock among pediatric patients is hypovolemic shock. When compared to adults, pediatric patients have a much lower intravascular volume reserve secondary to smaller hepatic and skeletal stores. Shock can be grouped into four major types: hypovolemic, distributive, obstructive, and cardiogenic. Before discussing the differences between the types of shock, we will review the common pathophysiology.
To understand shock, we must briefly review how oxygen is delivered throughout the body as inadequate oxygen delivery defines shock (see Diagnostics and Interpretation below for evaluation of oxygen delivery). Oxygen delivery is a function of the product between oxygen carrying capacity and cardiac output. Assuming that oxygen carrying capacity is adequate, oxygen delivery then becomes a function of cardiac output, which in turn is a function of stroke volume and heart rate.
Upon assessing a patient with concerns for shock, one starting point may be to consider the relationship between cardiac output (CO) with heart rate (HR) and stroke volume (SV): CO = HR x SV
Heart rate plays a dominant role in compensation for decreased SV. Adults can readily double CO as their baseline heart rate is more typically 50 to 70. Children are therefore at a significant disadvantage especially younger children and infants with a baseline heart rate typically greater than 100. Because autoregulation of SV is limited, the change in HR then becomes a critical vital sign when assessing for shock.
The heart rate itself is regulated by two factors: 1) vagal tone and 2) catecholamines. Catecholamines are released in response to stress and have two major circulatory effects: 1) increase in heart rate (i.e., tachycardia), and 2) increase in peripheral vascular tone (resistance) (i.e., vasoconstriction) resulting in cool, pale extremities.
When a disease process causes a component of SV to decline, HR must increase in order to maintain normal CO. Therefore, a resting tachycardia (i.e., tachycardia while the patient does not appear to be stimulated or agitated) would be an initial warning sign when suspecting or at risk for shock. Shock can then be divided into compensated versus hypotensive shock (Figure 1).

Figure 1. Compensated versus hypotensive shock. HR can compensate to maintain BP to a point at which it can no longer sufficiently compensate to maintain BP, resulting in hypotension.
The goal is to prevent the progression from compensated shock to hypotensive shock with timely recognition and intervention. In addition to timely recognition of a shock-like state, the components of SV need to be understood. SV is comprised of three main components: preload, contractility, and afterload. The following diagram identifies where each component lies (Figure 2). Upon identification of the specific component of SV that is compromised, intervention(s) can then be initiated.

Figure 2. Cardiovascular circulation diagram
In more simplified terms, circulatory function depends on 3 components: 1) blood volume (the fluid in the system), 2) cardiac function (the pump), and 3) vascular tone (the pipes).
Tracing blood flow through this cardiovascular diagram, preload refers to the area where deoxygenated blood returns to the right side of the heart. This deoxygenated blood is then pumped from the right heart into the pulmonary circulation where it picks up oxygen and returns to the left heart. Oxygenated blood is then pumped from the left heart into the systemic circulation against the systemic circulation resistance, or afterload, as determined by the arterial vascular tone. Preload and afterload also apply to the pulmonary circulation but will not be discussed here.
Four major types of shock will be discussed in this chapter (hypovolemic, distributive, obstructive, cardiogenic). In hypovolemic shock, preload is decreased due to decreased fluid in the system (such as in dehydration or blood loss), thereby decreasing stroke volume. Distributive shock is often the result of changes in systemic vascular resistance, secondary to leaky pipes or inappropriately large pipes (vasodilation), which can be compounded by decreased preload. Contractility may be hyperactive as a compensatory measure, or it may be decreased due to endotoxins and cytokines produced from septic shock, which is a variation of distributive shock. In obstructive shock, the myocardium is restricted from filling or ejecting due to external forces (such as in cardiac tamponade). Finally, in cardiogenic shock there is a significant decrease in myocardial contractility or pump function. Table 1 outlines changes in vascular pressures according to the different types of shock. All of these ultimately lead to a decrease in cardiac output which leads to a decrease in tissue perfusion.
Table 1: Types of shock and the effect on hemodynamics.
Assessing Stroke Volume Components
Each SV component has its own unique method to assess its status. Preload traditionally can be assessed by measuring a central venous pressure (CVP) through a central venous catheter (CVC) inserted either percutaneously through a large central vein, e.g., internal jugular vein, subclavian vein, or femoral vein, or through a peripherally inserted central catheter (PICC). These catheters can measure CVP when the tip is located ideally at or near the junction between the superior vena cava (SVC) and right atrium (RA). However, it has been repeatedly demonstrated that a CVP may not accurately reflect preload without proper context. For larger patients, preload assessment can be better achieved by utilizing the venous capacitance of the lower extremities and lifting both legs upward while observing changes in arterial BP and HR. Ideally, an arterial catheter is present to monitor changes in BP in real time. As the legs are raised, CVP and preload are increased. Likewise, in infants, toddlers who have relatively less abdominal fascia and muscle, applying gentle pressure over the right upper abdominal quadrant over the liver will augment preload. If the consequence of increased preload were to increase CO, then for hypotensive shock a significant improvement in BP should be observed with the potential concomitant decrease in tachycardia. This would then suggest that an intervention targeting preload (e.g., fluid resuscitation) as seen in Figure 2 would be beneficial in treating the patient with shock.
Contractility is a visual assessment done by echocardiography. In addition to the gross motion of the ventricular walls, the calculated shortening fraction of the myocardium and ejection fraction of the left ventricle can reflect the heart’s contractility status. In some forms of shock, contractility is hyperdynamic, whereas in others it may be markedly poor and would benefit from targeted inotropic intervention.
The concept of afterload is simplistically the downstream systemic blood pressure. Pulse pressure (PP) is the difference between the systolic BP (SBP) and diastolic BP (DBP). A wide PP may suggest decreased SVR or poor vascular tone. Since palpation of pulses is a function of the differential between SBP and DBP, a widened PP may give the impression of bounding pulses even when the patient is hypotensive. Vasoconstriction and elevated SVR typically result in a narrow PP and can result in cooler distal extremities, thready pulses, and pallor. Severe vasodilation due to loss of vascular tone may result in warm extremities and erythema. CRT is the time it takes to recover from blanching of the skin after applying firm pressure. The time is typically prolonged (greater than 2 to 3 seconds) in shock. However, just like with CVP, CRT is a poor independent indicator of shock. With inappropriately low SVR, CRT occasionally is observed to be paradoxically very short and is referred to as flash capillary refill, which again is inconsistent. Table 2 summarizes the various parameters for afterload.
Table 2: Afterload Assessment
Ultimately, shock is a dynamic process that if left untreated, progresses through two phases: 1) compensated and 2) uncompensated. Compensated shock, by definition, occurs when the body can successfully compensate for a circulatory disruption and maintains adequate vital organ perfusion and oxygenation.
As shock progresses, the compensatory mechanisms (e.g., increasing heart rate and vasoconstriction) reach their maximum ability and cannot increase further, resulting in decompensation. Metabolic demands are not met, and cellular ischemia results in the release of vasoactive mediators which affect the microcirculation resulting in end-organ perfusion compromise and lactic acidosis. At this point, damage to key organs (heart, brain, kidneys) may occur.
Ideally, the goal is to correct shock while the body is still compensating appropriately. Although there are four main types of shock, any given patient may progress through multiple types. Understanding these types can help with treatment and prevent further decompensation.
Physical exam findings do not necessarily have high positive or negative predictive value, but they can be used to target interventions when taken in context. A generalized toxic or very weak appearance of the patient may prompt more immediate intervention, whereas a somewhat playful and interactive child may provide some reassurance. Vital sign values are basic yet integral for clinically assessing the status of shock. Heart rate is one such invaluable parameter for the ongoing assessment and intervention cycle. Tachycardia at rest in a patient at risk for shock can serve as a warning. Other abnormal vital signs in shock can include varying pulse pressure (elevated diastolic BP due to increased SVR), hypotension (uncompensated shock and a late finding), and hypotension with bradycardia (uncompensated shock and impending cardiac arrest). It is worth noting that hypotension and bradycardia can also be secondary to a medication overdose (e.g., beta-blocker overdose). Physical exam findings that reflect afterload include temperature and color of the extremities. When noting delayed CRT peripherally, it may be helpful to assess CRT centrally, (e.g., on the chest) to see if central perfusion is better or just as poor. There can be pitfalls, however, when interpreting CRT. If the body is developing a fever or is in a cold environment, vasoconstriction results and capillary refill is not as reliable. Like any other single sign, this must be interpreted in aggregate with all other findings. Regardless of the etiology, inadequate cardiac output may result in compromise of certain target organs that may be more readily measurable. Hypoperfusion to the brain may result in changes in mental status, and the patient may become hyper somnolent or poorly responsive especially to noxious stimulation. Lab values are discussed below with regards to renal and hepatic perfusion. While not an exam finding per se, compromised renal perfusion may also result in decreased or no urine output in shock-like states.
Other physical findings may be more specific for certain types of shock. Exam changes for hypovolemic shock may include the presence of sunken eyes and lack of tears especially while crying, sunken anterior fontanelle in younger infants, sticky oral mucous membranes, and chapped lips. In distributive shock there are two main etiologies: anaphylaxis and sepsis. These etiologies both have unique clinical presentations which are covered in more detail in their respective chapters. Briefly, in all patients with distributive shock you may find extremities or whole body warm to touch and flushed or more deeply erythematous. CRT may be prolonged. In anaphylaxis, additional physical exam findings may include angioedema, stridor, wheezing, or skin changes such as urticaria. In sepsis, additional physical exam findings may include fever and other stereotypical rashes, or generalized erythroderma seen in toxin-mediated diseases. While rare in the pediatric population, obstructive shock may produce more unique physical findings such as jugular venous distention (JVD) in cardiac tamponade or absent breath sounds with tracheal deviation and unilateral chest wall movement with respirations in tension pneumothorax. Cardiogenic shock may also share some physical findings with obstructive shock such as JVD and hepatomegaly in addition to tachycardia. Heart sounds such as murmurs or a gallop rhythm may offer a clue if suspecting cardiogenic shock secondary to valvular disease or congestive heart failure.
Initial laboratory tests should include glucose and ionized calcium measurements, as hypoglycemia and hypocalcemia should both be corrected immediately. With severe capillary leak, total calcium will be falsely low secondary to acute hypoalbuminemia. Therefore, ionized calcium is more ideal to assess for hypocalcemia and to titrate treatment.
As mentioned above, renal function may be impaired by shock and can be assessed by blood urea nitrogen and creatinine levels. Hypoperfusion of the liver may result in release of hepatic enzymes such as AST and ALT, but hepatic function should be assessed by prothrombin time including INR, direct bilirubin, and ammonia.
CO should be assessed on a global or systemic level. Inadequate delivery of oxygen is often associated with poor vital sign parameters such as HR and BP, but they do not assess whether oxygen is being delivered adequately. The two main parameters for global oxygen delivery are serum lactate and mixed venous oxygen saturation (SvO2). Oxidative phosphorylation takes place in the mitochondria producing the normally desired product adenosine triphosphate. However, when faced with inadequate oxygen delivery (when demand exceeds supply) or inability to extract oxygen (mitochondrial failure), mitochondrial respiration switches to an anaerobic pathway and produces lactate as the by-product. This parameter is included in the Surviving Sepsis Campaign in Children (1) and is typically obtained upon initial presentation in the Emergency Department. Of note, serum lactate ideally should be obtained from a free blood flowing sample, e.g., from a central venous catheter or an arterial catheter/puncture. When obtaining a serum lactate sample from a venipuncture or at the same time upon insertion of a peripheral intravenous catheter, a tourniquet is routinely placed to facilitate the needle or catheter insertion. This may result in local tissue destruction and release of lactic acid into the bloodstream, thereby causing a potentially falsely elevated lactate. Conversely, if such a sample is obtained, and the serum lactate is within normal limits, confidence is higher that a low lactate level is true.
SvO2 requires adequate mixing of venous blood return from the entire body. Ideally, the sample is obtained from the pulmonary artery, but a sample from the right atrium is generally sufficient. This is obtained via a central venous catheter or long line PICC in which the tip of the catheter is placed where the SVC connects into the RA, commonly referred to as the SVC-RA junction. A normal range for SvO2 is between 65% to 75%. Low SvO2 suggests a low CO because a low SvO2 indicates high oxygen extraction from the blood due from low CO and tissue perfusion, in which one or more of the three main components of SV should be addressed further. High SvO2, however, suggests mitochondrial failure in which oxygen molecules are prevented from being extracted from red blood cells despite seemingly adequate CO and arterial blood oxygen content such as during some sepsis conditions.
Lab tests to consider include blood gas analysis, serum lactate, comprehensive metabolic panel, complete blood count, coagulation studies , type & crossmatch (for trauma patients with significant blood loss).
Initial imaging can include a chest x-ray to evaluate for cardiomegaly, pulmonary edema, pneumonia, or pneumothorax. Point of care ultrasound can be used to evaluate for pericardial effusion, pleural effusion, or pneumothorax. Echocardiography can be used to evaluate for obstructive lesions, cardiac function with measurements of ejection fraction and shortening fraction, intraventricular septal flattening and tricuspid regurgitation, and a gross visual estimate of circulatory volume status. A 12-lead ECG can be helpful to look for arrhythmias, ST changes, and low voltages.
Types of Shock
Hypovolemic shock is the abnormally low level of fluid in the circulatory system, such as in dehydration or acute blood loss. Fluid loss that drains the system is the most common cause of shock in pediatric patients. In this population, a loss of fluid can be detrimental and quickly progress to shock as they do not have much reserve. Not only is it the leading cause of shock among pediatric patients, it is also the most common cause of death in children worldwide (secondary to diarrheal illness). When hypovolemia is secondary to hemorrhage, this can further exacerbate shock due to the loss of oxygen carrying capacity in blood.
Possible etiologies for hypovolemic shock can be further broken down into fluid loss, blood loss, capillary leak, and renal losses. Acute gastroenteritis is the most common etiology causing diarrhea, vomiting, or both. Dehydration can be exacerbated or caused by poor intake of fluid. Fever and excessive diaphoresis can also exacerbate dehydration from increased insensible fluid losses. Even respiratory infections can lead to severe hypovolemia particularly in infants who often develop poor oral intake and quickly become dehydrated. Blood loss is broad and can be caused by trauma, surgery, GI hemorrhage, pulmonary hemorrhage, and menorrhagia. Capillary leak can result from burn injuries, nephrotic syndrome, and sepsis. Renal losses include both diabetes mellitus and diabetes insipidus. Another vulnerable patient population is the medically fragile children who depend on intake from caregivers using surgical feeding tubes, e.g., gastrostomy tube, to maintain adequate hydration and nutrition, or short gut syndrome patients who are dependent on total parenteral nutrition.
Distributive shock is due to poor vascular tone and often complicated by capillary leak. Three main etiologies largely represent this type of shock: sepsis, anaphylaxis (including drug reactions), and spinal cord injury. These etiologies result in peripheral vasodilation and decreased systemic vascular resistance which leads to redistribution of blood volume and subsequent decreased SV. Of these three, anaphylaxis and spinal cord injury rely primarily on vasopressor medications to reverse poor vascular tone. Septic shock may require vasopressor medications for poor vascular tone, vasoactive medications for impaired myocardial contractility, and/or fluid resuscitation for capillary leak. These may occur from the primary infection or be dramatically exacerbated after the initial antibiotic administration that lyse the bacteria and cause the release of toxins or surge of cytokines or both.
Pathogens with a higher risk for inducing septic shock: Bacterial etiologies include Escherichia coli, Neisseria meningitidis, Haemophilus influenzae type B, Pseudomonas aeruginosa, Staphylococcus aureus, Group A Streptococcus (Streptococcus pyogenes), Streptococcus pneumoniae, Group B Streptococcus (Streptococcus agalactiae). Viral etiologies include influenza, Dengue, Ebola. Other etiologies include candida species and Rickettsial species.
Obstructive shock is rarer in the pediatric population. The three main etiologies include pericardial tamponade, tension pneumothorax, and pulmonary embolism. Pericardial tamponade and tension pneumothorax are more common than pulmonary embolism and results in the restriction of the myocardium. Typically, this is related to trauma or surgical scenarios resulting in bleeding in the pericardial sac or mediastinum as well as air leak resulting in pneumothorax, pneumomediastinum, or pneumopericardium. Pulmonary embolism may result from hypercoagulable states such as in oral contraceptive use, protein C deficiency, protein S deficiency, or anti-phospholipid syndromes.
Regardless of the etiology, forward blood flow is impeded by the inadequacy of ventricular filling or inhibited ejection of blood or both. Clinically this can be confusing due to the similar vital sign changes for other types of responses for shock such as tachycardia and hypotension. Adding inotropic or vasoactive agents such as dopamine or epinephrine may paradoxically be detrimental for tamponade physiology as they would force the myocardium to contract more vigorously in an inadequately filled ventricle and may result in a worse cardiac output state or even cardiac arrest. JVD may be visible in some patients and may offer an important clue. If CVP is being measured, an elevated CVP may also offer a clue. For tamponade and tension pneumothorax, fluid boluses may provide extra stabilizing time before definitive surgical intervention can be performed.
In cardiogenic shock (pump failure) decreased myocardial contractility leads to decreased SV. Etiologies include: 1) Myocarditis or pericarditis (e.g., Coxsackie post-infection, Kawasaki Disease). 2) Congestive heart failure (e.g., congenital heart defects, rheumatic heart disease). 3) Arrhythmia (e.g., supraventricular tachycardia). 4) Myocardial infarction (e.g., anomalous origin of coronary arteries). 5) Cardiac trauma. 6) Drugs (e.g., anthracyclines).
A more typical etiology in the pediatric population is viral myocarditis, which often is a post-infectious phenomenon with a history of a prodromal viral illness. The stereotypical virus causing myocarditis is Coxsackie virus, but others can certainly have a similar effect. Streptococcus pyogenes tonsillopharyngitis (not impetigo) left untreated is the most common bacterial etiology for acute rheumatic carditis and heart failure resulting in extensive valvular disease. Impaired contractility requires inotropic medications. Inotropy typically involves targeting specific adrenergic receptors. Table 3 outlines the various adrenergic receptors and their effects upon activation.
Table 3: Adrenergic receptor effects
| D1 | smooth muscle relaxation: vasodilation (renal, mesenteric, coronary) |
| D2 | smooth muscle relaxation, inhibition of NE release: vasodilatation (renal, mesenteric) |
| beta-1 | myocardium: chronotropy, inotropy |
| beta-2 | smooth muscle and other sites: vasodilation |
| alpha-1 | Vasoconstriction |
| alpha-2 | vasoconstriction (CNS alpha-2A: vasodilation via inhibition of NE release) |
In the treatment of hypovolemic shock, the objective is relatively straightforward: restore volume (add fluid to the system) and prevent further losses. To maintain normal serum tonicity, fluids must also be volume expanders such as normal saline (NS) or lactated Ringers (LR) when repleting a patient’s volume. This is regardless of the patient’s current serum sodium level. Dehydration with hyponatremia or hypernatremia is treated with NS or LR during fluid resuscitation.
Current guidelines and best practice is to begin with an initial bolus of 10 to 20 mL/kg and reassess perfusion. Multiple studies have found decreased survival when pediatric patients were over fluid resuscitated with crystalloid fluids (1,3). Care should be taken to watch for signs of fluid overload and only give as much fluid as needed to improve perfusion. However, many circumstances require larger volumes of fluid during resuscitation. A general guideline recommendation would be to repeat fluid boluses as needed up to 60 mL/kg, at which point a reassessment of the patient’s status including other potential areas of SV compromise should be considered, especially if the patient remains in a refractory shock-like state.
Infusion rates should be fast. Rates can be increased by manually pushing the infusion with a syringe or squeezing the bag of fluid if deemed necessary. In adult patients, fluid resuscitation can be as fast as 60 mL/kg over 10 minutes, which is facilitated by a large bore, short IV catheter. In smaller children, very small caliber IV catheters may be the greatest limiting factor for infusing at faster rates. Smaller children and infants also have a higher incidence of losing a viable vein due to extravasation and ruptured vessels when exposed to higher infusion pressures. If vascular access is difficult to obtain, providers should not hesitate to insert an intraosseous (IO) needle. The most common insertion site is the proximal tibia distal to the growth plate due to the proximity to the skin and larger, flat bone surface, especially if insertion is occurring during resuscitation. It is worth noting that while sometimes necessary and lifesaving, intraosseous needle insertion is very painful as you are essentially performing a bone marrow biopsy. Therefore, the use of subcutaneous lidocaine prior to IO insertion would likely be greatly appreciated by conscious or semiconscious patients.
Albumin is also isotonic and has some colloid properties that is sometimes favored with the hope that fluids will be retained in the intravascular compartment longer than for NS or LR. However, several studies have demonstrated no outcomes benefit with albumin solutions compared with NS or LR. Some studies have also demonstrated an association with higher morbidity and mortality with albumin solutions used for fluid resuscitation. This may be due to its oncotic properties and the risk of leaking through capillary walls during systemic inflammatory response syndrome (SIRS) (3). Despite the acute increase in serum oncotic pressure with albumin infusion, albumin leaks into the extravascular compartment through the now permeable capillary walls. The result is an increase in extravascular oncotic pressure and the movement of water from the intravascular compartment to the extravascular compartment, thereby exacerbating anasarca. Albumin solutions, therefore, are sometimes delayed in use until capillary leak is sufficiently resolved. Albumin solutions are also expensive, raising the cost-benefit issue. However, when a patient is already grossly total body water overloaded and yet intravascularly depleted while having a low serum oncotic pressure (as reflected by a low serum albumin), the volume of fluid resuscitation can be optimized by using 25% albumin. By infusing 1 g/kg (maximum dose of 25 g) intravenously over a relatively shorter period of time (30 to 60 minutes), an oncotic gradient can be induced to shift water from the extravascular compartment to the intravascular compartment, thereby augmenting preload and CO while using less volume than with other crystalloid solutions.
For hemorrhagic shock, guidelines have changed for adults in recent years with the American College of Surgeons Advanced Trauma Life Support guidelines for adults suggesting a one-to-one-to-one ratio of packed red blood cells, fresh frozen plasma, and platelets. Data on its use in the pediatric population is limited but is currently thought to be a safe option, and blood products are being used earlier when treating hemorrhagic shock in children. However, more research is needed on this topic.
While technically challenging, the treatment for obstructive shock is conceptually simple: remove the obstruction. Therefore, the emphasis is placed on early recognition and diagnosis of the underlying etiology. An initial intervention of fluid resuscitation is indicated to offset the external restrictive forces on the myocardium. In tension pneumothorax, the myocardial contraction becomes inhibited by external forces, and emergent needle thoracentesis decompression is then indicated. Patient deterioration is often rapid, thus obtaining a chest radiograph is often not possible since the needle thoracentesis must be done immediately. The other not uncommon complication of certain autoimmune and cardiac diseases is pericardial tamponade, which may require pericardiocentesis and/or pericardial drain placement. If cardiac tamponade is suspected, pericardial effusion can be demonstrated by echocardiography and can also be used as guidance for pericardiocentesis to relieve the tamponade.
In cardiogenic shock, the problem lies within the heart. Therefore, treatment is focused on supporting the remaining cardiac function. This is done through inotropes, judicious use of fluids, and cardiopulmonary resuscitation with cardioversion/defibrillation if needed. Table 4 lists the various adrenergic medications utilized in a continuous intravenous infusion (4,5). The most recent Surviving Sepsis Campaign Guidelines in Children recommended the use of epinephrine or norepinephrine over dopamine as the first vasoactive drug of choice.
Table 4: Adrenergic medications and Clinical Effects
| Lower doses: -renal and mesenteric vasodilation -inotropy Higher doses: -vasoconstriction | |||||||||
| (-) isomer: ++ (+) isomer: - - - | -Inotropy -Net vasodilation | ||||||||
| Lower doses: -inotropy -chronotropy -vasodilation Higher doses: -inotropy -chronotropy -vasoconstriction | |||||||||
Isoproterenol is a non-selective beta-receptor agonist, while dobutamine (DB) is a somewhat selective beta-1-receptor agonist. They theoretically achieve the two desired effects of inotropy and afterload reduction for cardiogenic shock. Isoproterenol and DB have significant inotropic effects; however, they may induce significant chronotropy resulting in inadequate filling time for ventricles and leading to worsening CO. Their beta-2 agonist effect on vasodilation and afterload reduction also may be excessive and result in worsening hypotension. These two undesired effects may limit isoproterenol and DB’s use. On the other hand, DB’s half-life is extremely short, and its adverse effects may be temporarily offset with other medications if a trial on DB is desired.
Epinephrine (EPI) and norepinephrine (NE) target the same broad adrenergic receptors but are viewed differently in practice. Despite activating all receptors, EPI has a predominant inotropic and chronotropic effect through beta-receptor activation particularly at lower doses of less than 0.1 mcg/kg/min. NE, on the other hand, has a predominant alpha-receptor effect and is considered primarily a vasopressor agent rather than an inotropic agent. Therefore, considering the goal of reducing afterload in cardiogenic shock, EPI is much more favored, and NE is not normally used. However, for patients in other types of shock, NE may be preferred over EPI.
Milrinone is a phosphodiesterase (PDE) III inhibitor agent and serves as an inodilator (i.e., induces inotropy and afterload reduction), which are the two desired effects for treating cardiogenic shock. As a PDE III enzyme reaction blocker, milrinone’s effects are not receptor activation dependent, which can become more significant in circumstances when adrenergic receptor activation is blunted (e.g., due to cardiopulmonary bypass or upon adrenergic medication tachyphylaxis). Blocking PDE III inhibits the breakdown of cAMP leading to enhanced calcium transport into the myocardial cells and enhance contractility. Unlike DB, milrinone does not cause chronotropy, and its afterload reduction effects may be less severe. This makes milrinone one of the leading drugs of choice for cardiogenic shock. Because it has a long half-life, though, it does not have an immediate impact on cardiogenic shock. The exception may be when a loading dose of milrinone is given, but the result may be more profound afterload reduction and subsequent hypotension. Therefore, loading doses are not typically given. Instead, EPI or DA are often started in conjunction with milrinone. Milrinone also works synergistically with beta-agonists.
It is important to consider calcium as a potential and potent inotropic agent. Calcium is the substrate required for muscle contractility, and in many situations, calcium depletion can lead to a refractory shock-like state. One situation not uncommonly encountered is acute hypotension following PRBC transfusion. PRBCs are maintained in soluble form (anticoagulated) by citrate, which chelates ionized calcium low enough to prevent clotting. If enough PRBCs are transfused, a patient’s ionized calcium level (iCa) may become low enough to affect myocardial contractility. Very young and newborn infants are also more vulnerable to symptomatic hypocalcemia due to poor calcium body reserves. Some infants are born with severe congenital heart defects. A subset of these defects may be caused by 22q11.2 deletion syndrome or DiGeorge Syndrome, which includes severe hypocalcemia (due to parathyroid aplasia and parathyroid hormone deficiency). These infants often develop refractory shock due to severe hypocalcemia especially post-operatively from surgical repair of the associated congenital heart defects. Calcium treatment in this context is given intravenously in the form of calcium chloride or calcium gluconate. Calcium chloride is immediately bioactive upon infusion, whereas calcium gluconate requires hepatic metabolism to become bioactive. Therefore, in circumstances when liver function is compromised, calcium chloride is the drug of choice. Calcium should be infused slower than the maximum rate of 50 mg per minute or maximum duration of 5 minutes to avoid the adverse cardiac side effects. Conservatively, calcium is often infused over 20 minutes. Because of the requirement for hepatic metabolism and delayed onset of action, calcium gluconate is sometimes considered safer to administer when liver function is not a factor. However, the potential adverse cardiac effects are the same for both parenteral forms.
In addition to inotropic support for cardiogenic shock, patients may also benefit from judicious fluid resuscitation. However, their capacity to tolerate larger boluses as given for hypovolemic shock is likely poor and may exacerbate shock as well as cardiogenic pulmonary edema. It is reasonable to administer a 5 ml/kg infusion over a longer period (e.g., 30 to 60 minutes) and then reassess.
Special notice should be given to infants presenting with cardiogenic shock within the first few weeks of life as this may indicate a ductal dependent lesion. Ductal dependent lesions refer to congenital heart diseases that require a patent ductus arteriosus for arteriovenous mixing to be survivable such as in transposition of the great vessels. When the ductus arteriosus begins to close, silent congenital heart diseases can present as cardiogenic shock with mottling of skin, lethargy, and lactic acidosis. If this is suspected, a prostaglandin E1 infusion should be initiated immediately to maintain patency of the ductus arteriosus.
Antiarrhythmics may also be used when specific arrhythmias are identified. Either IV amiodarone or lidocaine can be used to treat ventricular tachycardia or ventricular fibrillation. For stable supraventricular tachycardia IV adenosine can be used. However, in unstable supraventricular tachycardia, first line therapy is synchronized cardioversion. Premedication with analgesics and/or sedatives are highly recommended for conscious and responsive patients. Unsynchronized cardioversion is indicated for pulseless ventricular tachycardia and for ventricular fibrillation.
Treatment of distributive shock is also dependent on the etiology. The treatment of septic shock offers the best framework for treating distributive shock and will be the focus of this section. More details on sepsis can be found in the chapters on Sepsis and Neonatal Sepsis.
The initial management of septic shock includes giving the patient 10 to 20 mL/kg fluid boluses, and up to a total of 40 to 60 mL/kg in the first hour. Frequent reassessments are made after each bolus with appropriate titration as needed. Fluid resuscitation is discontinued if the patient shows any signs of fluid overload such as crackles or hepatomegaly. Crystalloid is acceptable for fluid resuscitation in septic shock. When the patient is fluid-unresponsive, norepinephrine or epinephrine infusions are used. With ongoing shock refractory to vasoactive infusions, vasopressin may be considered. Vasopressin is a neuropeptide hormone with increased levels as an early compensatory response to hypotension. For septic shock in particular, vasopressin levels may become rapidly depleted leading to the refractory shock-like picture. Another potential complication leading to refractory shock is relative adrenal insufficiency, which would require stress-dose corticosteroids.
In summary, shock is a clinical syndrome of circulatory dysfunction resulting in decreased tissue perfusion. Normal circulatory function depends on three factors: cardiac function (the pump), vascular tone (the pipes), and blood volume (the fluid). A disturbance in one or more results in inadequate delivery of oxygen and nutrients to the tissues, which then leads to shock. Ideally, early recognition and treatment of compensated shock is essential to prevent transition to decompensated shock, which is much more challenging to overcome.
Questions
Getting back to our Case Scenario 2: A 12-year-old girl (40 kg body weight) presents with the chief complaint of respiratory distress and lethargy over the past 18 hours. Parents state that this morning she didn’t feel well. Initial respiratory rate is 40 breaths per minute. Lung exam is notable for tachypnea, slight subcostal retractions and nasal flaring. Aeration is good bilaterally and with faint, fine crackles over the lung bases. No wheezing is appreciated. She is arousable but difficult to maintain attention, poorly following commands, and not particularly bothered by peripheral IV insertion. Cardiac exam is notable for significant tachycardia with a HR of 150, BP 75/35, mean arterial pressure (MAP) 48. Radial pulses are weak, femoral pulses palpable, fair. Hands and feet feel cool to touch. CRT is 5 seconds in the fingers and toes, 4 seconds over the sternum. Abdominal exam is without tenderness or distention. A liver edge is noted to be 5 cm below the right costal margin. Neurologically, she appears to be moving all of her extremities with mild grimacing, weak speech, and localized flexion withdrawal to pinching. Pupils are 4 mm in diameter and are briskly reactive to light. Skin exam unremarkable for any rash.
Initial triage: Initial saturation of peripheral oxygen (SpO2) is 92% on room air. Despite lack of appreciable wheezing, a trial of nebulized albuterol and ipratropium solution is given via nebulizer face mask with the fraction of inspired oxygen (FiO2) of 1.0 with no effect. Oxygen face mask is then changed to a non-rebreather mask at 10 L/min, FiO2 1.0 with SpO2 95%. Upon PIV insertion, samples are obtained for laboratory evaluation while fluid is being prepared for administration.
1. What type of fluid should initially be given?
a. 25% albumin over 30 to 60 min
b. 1-unit PRBC over 60 min
c. 0.45% NaCl solution (1/2 NS), 10 to 20 mL/kg rapid infusion
d. 0.9% NaCl solution (NS), 10 to 20 mL/kg rapid infusion
e. D5 NS, 10 to 20 mL/kg rapid infusion
After a few minutes into the infusion, the patient becomes more tachycardic and hypotensive with worsening dyspnea and lethargy. SpO2 falls to 85% despite the non-rebreather mask. Upon re-examination of the abdomen, the liver edge is noted to be 4 cm below the right costal margin.
2. Your next immediate interventions are...
a. give an additional fluid bolus immediately following the first bolus and increase the oxygen flow rate to 20 L/min
b. slow down the fluid infusion to be given over 60 min and prepare to intubate
c. stop the fluid bolus immediately and begin airway support with manual positive pressure ventilation via bag-valve-mask while preparing to begin a vasoactive infusion
d. begin dopamine infusion immediately and prepare to intubate.
e. start chest compressions and begin airway support with manual rescue breathing via bag-valve-mask
Blood pressure improves to 80/50 after the start of the hemodynamic medication infusion. SpO2 remains at 87% despite manual ventilation on FiO2 of 1.0. Patient is then intubated. Copious amounts of pink, frothy fluid erupts through the larynx upon direct laryngoscopy during intubation. SpO2 is eventually improved to 92% after escalating mechanical ventilatory support and remaining on FiO2 of 1.0. Lung auscultation reveals fair aeration bilaterally with equal breath sounds, moderate diffuse crackles with slight end-expiratory wheeze. BP decreases to 60/40, HR 195. Distal pulses are thready with cool, pale extremities, central pulses are weak. CRT peripherally is >5 seconds, centrally 5 seconds. Heart sounds are appreciated, but HR is too fast to be able to appreciate any abnormal sounds.
3. The next appropriate hemodynamic intervention is...
a. begin an epinephrine continuous infusion
b. begin chest compressions
c. begin a vasopressin continuous infusion
d. give a stress-dose hydrocortisone bolus
e. begin a norepinephrine continuous infusion
Blood pressure improves to 75/55, HR 190. Extremities exam is relatively unchanged. Lactate from the PIV insertion is 10 mmol/L (normal <2). An arterial catheter is emergently placed. The arterial blood gas is pH 7.18, pCO2 35, pO2 65, base excess -14. Lactate from the arterial sample is 9.5 mmol/L. iCa is 0.85 mmol/L (normal 1.20 to 1.32). A CVC is emergently placed.
4. The next medication to try now to improve cardiac output is...
a. Bicarbonate, NaHCO3
b. Hydrocortisone stress dose
c. Cosyntropin stimulation challenge to determine efficacy for stress-dose corticosteroids
d. Calcium, as calcium chloride
e. Calcium, as calcium carbonate
BP improves to 90/65, HR 170 after medication given.
5. The following evaluative interventions are reasonable at this time EXCEPT:
a. Echocardiography
b. eFAST exam
c. Chest radiograph
d. 12-lead electrocardiogram
e. Viral, bacterial and fungal samplings for analysis
6. Other reasonable interventions to consider include which of the following (select all that apply):
a. Calcium continuous infusion
b. Milrinone continuous infusion
c. Bronchoalveolar lavage
d. Continuous renal replacement therapy
References
1. Weiss, Scott L. MD, MSCE, FCCM (Co-Vice Chair)1; Peters, Mark J. MD, PhD (Co-Vice Chair)2; Alhazzani, Waleed MD, MSc, FRCPC (Methodology Chair)3; Agus, Michael S. D. MD, FCCM, FAAP4; Flori, Heidi R. MD, FAAP5; Inwald, David P. MB, BChir, FRCPCH, FFICM, PhD6; Nadel, Simon MBBS, MRCP, FRCP6; Schlapbach, Luregn J. FCICM, FMH-ICU, FMH-Paeds, FMH-Neonatology7; Tasker, Robert C. MB BS, MA, AM, MD, FRCPHC, FRCP4; Argent, Andrew C. MB BCh, MMed, MD (Paediatrics)8; Brierley, Joe MD, MA9; Carcillo, Joseph MD10; Carrol, Enitan D. MB ChB, MD, FRCPCH, DTMH11; Carroll, Christopher L. MD, MS, FCCM, FAAP12; Cheifetz, Ira M. MD, FCCM13; Choong, Karen MB, BCh, FRCP(C) (methodologist)3; Cies, Jeffry J. PharmD, MPH, BCPS-AQ ID, BCPPS, FCCP, FCCM, FPPAG14; Cruz, Andrea T. MD, MPH, FAAP15; De Luca, Daniele MD, PhD16,17; Deep, Akash MB BS, MD, FRCPCH18; Faust, Saul N. MA, MB BS, FRCPCH, PhD, FHEA19; De Oliveira, Claudio Flauzino MD, PhD20; Hall, Mark W. MD, FCCM, FAAP21; Ishimine, Paul MD, FACEP, FAAP22; Javouhey, Etienne MD, PhD23; Joosten, Koen F. M. MD, PhD24; Joshi, Poonam PhD25; Karam, Oliver MD, PhD26; Kneyber, Martin C. J. MD, PhD, FCCM27; Lemson, Joris MD, PhD28; MacLaren, Graeme MD, MSc, FCCM29; Mehta, Nilesh M. MD4; Mřller, Morten Hylander MD, PhD30; Newth, Christopher J. L. MD, ChB, FRCPC, FRACP31; Nguyen, Trung C. MD, FAAP15; Nishisaki, Akira MD, MSCE, FAAP1; Nunnally, Mark E. MD, FCCM (methodologist)32; Parker, Margaret M. MD, MCCM, FAAP33; Paul, Raina M. MD, FAAP34; Randolph, Adrienne G. MD, MS, FCCM, FAAP4; Ranjit, Suchitra MD, FCCM35; Romer, Lewis H. MD36; Scott, Halden F. MD, MSCS, FAAP, FACEP37; Tume, Lyvonne N. BS, MSN, PhD, RN38; Verger, Judy T. RN, PhD, CPNP-AC, FCCM, FAAN1,39; Williams, Eric A. MD, MS, MMM, FCCM, FAAP15; Wolf, Joshua MBBS, PhD, FRACP40; Wong, Hector R. MD41; Zimmerman, Jerry J. MD, PhD, FCCM42; Kissoon, Niranjan MB BS, MCCM, FRCP(C), FAAP, FACPE (Co-Chair)43; Tissieres, Pierre MD, DSc (Co-Chair)16,44 Surviving Sepsis Campaign International Guidelines for the Management of Septic Shock and Sepsis-Associated Organ Dysfunction in Children, Pediatr Crit Care Med. 2020;21(2):e52-e106. doi: 10.1097/PCC.0000000000002198
2. Hoffman RJ, Wang VJ, Scarfone R, Godambe S, Nagler J. Fleisher and Ludwig’s 5-Minute Pediatric Emergency Medicine Consult, 2019. Wolters Kluwer, Philadelphia PA. pp:3154-3176.
3. Karafin MS, Hillyer CD, Shaz BH. Transfusion of Plasma and Plasma Derivatives: Plasma, Cryoprecipitate, Albumin, and Immunoglobulins. In: Hoffman R, Benz EJ, Silberstein LE, Heslop HE, et al (eds). Hematology, Basic Principles and Practice, 7th edition, 2018. Elsevier, Philadelphia, PA. pp:1744-1758.
4. Westfall TC, Macarthur H, Westfall DP. Adrenergic Agonists and Antagonists. In: Brunton LL, Hilal-Dandan R, Knollmann BC (eds). Goodman & Gilman’s: The Pharmacological Basis of Therapeutics, 13th edition, 2017. McGraw Hill, New York..
5. Sibley DR, Hazelwood LA, Amara SG. 5-Hydroxytryptamine (Serotonin) and Dopamine. In: Brunton LL, Hilal-Dandan R, Knollmann BC (eds). Goodman & Gilman’s: The Pharmacological Basis of Therapeutics, 13th edition, 2017. McGraw Hill, New York.
6. Eschenhagen T. Therapy of Heart Failure. In: Brunton LL, Hilal-Dandan R, Knollmann BC (eds). Goodman & Gilman’s: The Pharmacological Basis of Therapeutics, 13th edition, 2017. McGraw Hill, New York.
7. Jackson EK. Drugs Affecting Renal Excretory Function. In: Brunton LL, Hilal-Dandan R, Knollmann BC (eds). Goodman & Gilman’s: The Pharmacological Basis of Therapeutics, 13th edition, 2017. McGraw Hill, New York.
8. American Academy of Pediatrics, American Heart Association. Pediatric Advanced Life Support: Provider Manual. American Heart Association; 2021.
Answers to questions
This is a case of cardiogenic shock secondary to myocarditis likely from a post-infectious viral infection. Later upon further inquiry, the patient’s parents recall that she was sick with runny nose, coughing, headache and low-grade fevers two weeks ago after multiple family members had the same illness before her.
1. The correct answer is d: 0.9% NaCl (NS), 10 to 20 mL/kg rapid infusion. NS or LR is the solution of choice for fluid resuscitation, for almost any disease entity. Since the initial presentation and history had no indication for a myocarditis, it is reasonable to give a full fluid challenge of 10 to 20 ml/kg of isotonic solution and rapidly, not prolonged over one hour, for example. Hypotonic solutions would be inappropriate and would likely result in severe hyponatremia further complicating matters. Dextrose-containing solutions would also be inappropriate especially if serum glucose is unknown. If the patient was found to be significantly hypoglycemic, 10 ml/kg of D5 would increase serum glucose by approximately 100 mg/dL acutely when given as a rapid infusion. However, if the serum glucose were significantly greater than 100 mg/dL, e.g., as a physiologic stress response, then raising the glucose by an additional 100 mg/dL may result in a serum glucose much greater than 200 mg/dL and likely exceed the renal threshold for developing glucosuria and subsequent osmotic diuresis, there by exacerbating intravascular depletion. PRBC transfusion is not indicated in this scenario where acute bleeding shouldn’t be expected at this time. However, in cases of agglutination-induced severe or extreme anemia, e.g., from Mycoplasma pneumoniae infection, emergent PRBC transfusion may be indicated for this differential diagnosis.
2. The correct answer is c: Stop the fluid bolus immediately and begin airway support with manual rescue breathing via bag-valve-mask because she is hypoxic, while preparing to begin a vasoactive infusion. Hemodynamic and pulmonary changes are occurring because the patient is actually in congestive heart failure (CHF) with cardiogenic shock. For this reason, it is important for frequent and constant reassessment upon each intervention, and if the patient’s status worsens, the intervention must immediately be terminated. If CHF were known, it may be reasonable to administer an NS bolus of 5 mL/kg infused over one hour but still with frequent follow-up assessment for tolerance. In this situation, not only did the fluid bolus worsen heart failure and exacerbate cardiogenic shock, but it also induced worse cardiogenic pulmonary edema resulting in hypoxia and acute respiratory failure. Intubation may be required, but airway support with positive pressure manual ventilation should be initiated first to stabilize the pulmonary status as best as possible. In fact, the procedures required for intubation typically worsen cardiogenic shock with the subsequent risk of cardiac arrest, and it would be prudent to be prepared for that worst case scenario before intubation is initiated. A vasoactive agent may be necessary, but dopamine is no longer part of the algorithm for shock management. There is no indication for chest compressions at this time.
3. The correct answer is a: Begin an epinephrine continuous infusion. Given the high index of suspicion for cardiogenic shock and hypotensive shock, it is reasonable to target the beta-1 adrenergic receptor to augment inotropy. Epinephrine will also have beta-2 activation and potentially decrease SVR and afterload. However, bear in mind that escalating EPI infusion to much higher rates will induce significant alpha-receptor activation, and its vasoconstrictive effects will exceed its vasodilatory effects resulting in a net SVR elevation. This and worsening tachycardia may have a detrimental effect on cardiogenic shock. However, if the inotropic effect far exceeds the chronotropic effect, an improvement in tachycardia may actually be observed (CO = HR x SV). Dobutamine may be considered as an option. It has both inotropic and afterload reduction effects, but often it results in worsening hypotensive shock due to excessive chronotropic and afterload reduction effects. There is no indication for chest compressions at this time. There is no indication for vasopressin at this time and is not typically required for cardiogenic shock as opposed to septic shock. Vasopressin would also increase afterload, which would impede left ventricular (LV) ejection and exacerbate cardiogenic shock. There is no indication for systemic corticosteroids at this time. Norepinephrine has an overwhelmingly predominant alpha-receptor activation leading to vasoconstriction and elevation of SVR, which would impede LV ejection and exacerbate cardiogenic shock.
4. The correct answer is d: Calcium as calcium chloride. The ionized (unbound, biological active calcium) calcium level is clearly below normal. Calcium is the substrate for muscle fiber contraction and in this case the myocardium. One suggested target is to maintain iCa at 1.20 mmol/L or higher. Calcium carbonate (Tums), is not be appropriate in this scenario. Bicarbonate may or may not be indicated, but the patient’s acid-base status has not been established yet, and empiric administration would not be indicated. Some practices suggest that severe acidemia contributes to poor contractility, but this has yet to be proven definitively. Systemic corticosteroids are not indicated at this point, and a cosyntropin stimulation challenge would be a distraction and a waste of time and effort when more pressing matters are required.
5. There is no definite correct answer here. It could possibly be b. eFAST exam. An eFAST is used in trauma evaluation to quickly assess for free fluid in the chest and abdomen. It may be beneficial in detecting or confirming a pleural effusion or a pneumothorax. Some physicians have obtained the skills to be very expert at assessing cardiac function via point of care ultrasound so in the hands of some, eFAST can be very helpful. A chest radiograph would be much quicker to assess the cardiac silhouette size and lung perfusion to support the working diagnosis of CHF. Echocardiography would be tremendously helpful in this scenario for confirming the diagnosis and guiding therapy though it might take hours to obtain. A 12-lead electrocardiogram may also be helpful to identify pericarditis or myocarditis in addition to other electrical abnormalities that may contribute to cardiogenic shock such as tachydysrhythmias. For instance, supraventricular tachycardia with instability should be among the differential diagnoses. Viral, bacterial and fungal samplings for analysis would be useful, but they would take several days to render a result.
6. The correct answers are a & b: Calcium continuous infusion and Milrinone continuous infusion. Calcium as stated previously is inherent to muscle contractility. In many circumstances, a therapeutic response to a single or intermittent dosing schedule may not be sustained. Rather than waiting for hypotensive shock to recur due to iCa levels falling, a continuous calcium chloride infusion may be a better interventional strategy while titrating infusion rates against serial iCa levels. Milrinone may also be beneficial and may ultimately be the primary drug of choice for severe myocardial depression given its combined inotropic and afterload reduction effects without inducing tachycardia and without being dependent on receptor activation. This will also have a synergistic effect with calcium given its cytoplasmic calcium modulation in myocardial cells. Bronchoalveolar lavage is not indicated in this scenario and may more likely have detrimental clinical effects. Continuous renal replacement therapy (CRRT) may eventually be indicated if acute kidney injury (AKI) develops. Certainly, in this scenario, the risk for AKI is significantly high, and the patient may then benefit from CRRT. However, there is no indication to initiate this at this time.