Swollen Elbow with a Normal X-Ray
Radiology Cases in Pediatric Emergency Medicine
Volume 1, Case 19
Loren G. Yamamoto, MD, MPH
Kapiolani Medical Center For Women And Children
University of Hawaii John A. Burns School of Medicine
An 8 year old male presents to the ED complaining
of pain in his left elbow after falling off a 2 meter high
wall onto his hand and arm.
Exam: The left elbow is obviously swollen. He is
reluctant to move it due to pain. He points to the lateral
region of his elbow as the area of greatest pain.
Tenderness to the medial elbow is mild. Palpation of
the mid and upper humerus is non-tender. Palpation of
the mid and distal forearm is non-tender. His clavicle is
non-tender. His wrist is non-tender including the radial
and ulnar epiphyses. The carpal bones are non-tender
and his hand function is good. AP and lateral
radiographs of the elbow are obtained.
View elbow radiographs.
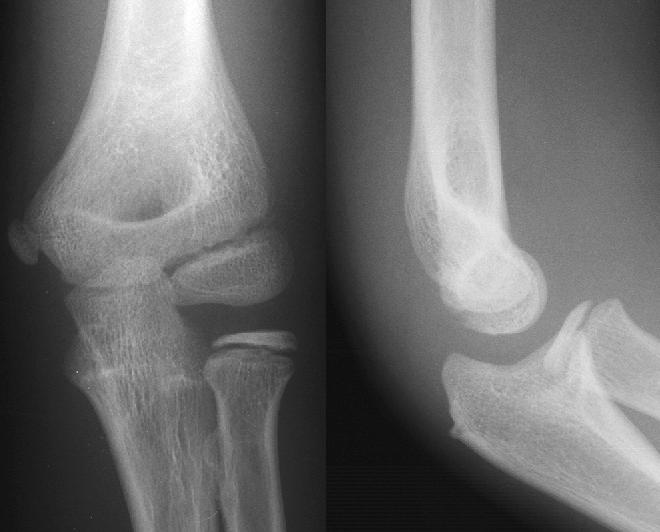 Although these radiographs appear to be normal,
the patient obviously has something wrong with his
elbow. Diagnosing a sprain of the elbow is a pitfall that
should be avoided. When the patient has obvious
clinical findings around the elbow, examine the
radiographs carefully for a posterior fat pad sign, a
supracondylar fracture, a radial head fracture, and
misplaced ossification centers that may represent
fractures.
In this case, none of these are visible on the
radiographs, which should lead one to be suspicious of
an occult fracture not radiographically visible. In this
case, two oblique views of the elbow were obtained.
View oblique films.
Although these radiographs appear to be normal,
the patient obviously has something wrong with his
elbow. Diagnosing a sprain of the elbow is a pitfall that
should be avoided. When the patient has obvious
clinical findings around the elbow, examine the
radiographs carefully for a posterior fat pad sign, a
supracondylar fracture, a radial head fracture, and
misplaced ossification centers that may represent
fractures.
In this case, none of these are visible on the
radiographs, which should lead one to be suspicious of
an occult fracture not radiographically visible. In this
case, two oblique views of the elbow were obtained.
View oblique films.
 The first oblique view does not reveal much, but the
other oblique view shows an obvious fracture of the
lateral (external) condyle. This diagnosis makes sense
based on the patient's physical exam. This fracture
typically produces a larger than expected degree of
swelling.
One might consider that this fragment over the
lateral condyle is the ossification center of the external
epicondyle (lateral condyle); however, this ossification
center does not have this appearance. In addition, this
ossification center is the last to appear in the elbow.
The ossification center of the olecranon appears before
this. Since the olecranon's ossification center is not
visible (see lateral view), the external epicondyle will not
be ossified yet. The mnemonic CRITOE is useful to
remember the sequence of appearance of the elbow
ossification centers (Capitellum, Radial Head, Internal
epicondyle, Trochlea, Olecranon, and External
epicondyle). See Case 11 (Elbow Ossification Centers
in a Child) for more details.
In retrospect, this fracture is visible on the AP
view. Go back and examine the lateral condyle region
of the AP view. Magnify the view to examine it closely.
View AP and lateral view above:
Discussion & Teaching Points:
1) A swollen elbow usually contains a fracture
injury. In some instances, a joint effusion (posterior fat
pad sign or enlarged anterior fat pad sign) can be seen
in the absence of a visible fracture. Occult fractures
may still be present in such cases. It is prudent to treat
such an injury as a non-displaced fracture, with a splint,
sling, and follow-up with a primary care physician or
orthopedic surgeon.
2) When uncertainty exists, careful examination of
the patient will often help guide your review of the
radiographs and the need to request special views.
3) Occult fractures in the elbow may be difficult to
identify. Areas that are commonly fractured include the
supracondylar region, the radial head, and the lateral
condyle.
4) Even with special views, not all fractures are
radiographically visible. Other imaging modalities such
as bone scanning, CT scanning, and MRI scanning
have all identified fractures in patients with normal
radiographs. Normal radiographs are not able to totally
rule out fractures. It is often beneficial to advise
patients of the limitation of radiographs. In any
musculoskeletal injury, persistent pain should prompt
the patient to seek medical care even if their initial set
of radiographs was normal. Orthopedic referral, a
repeat set of radiographs, or an advanced imaging
modality should be considered in injuries resulting in
persistent pain.
5) It is useful to include a standardized instruction
sheet to patients whenever radiographs are obtained in
the emergency department. This instruction sheet
should explain the possibility of interpretation errors,
differences of opinion in the radiographic interpretation,
the limitation of radiographs, and instructions for
follow-up. Such an instruction sheet can substantially
reduce the number of patient complaints regarding
misinterpreted radiographs and reduce the ED's liability
potential. An example of such an instruction sheet
follows:
1. The emergency physician has read your X-ray
as: Normal elbow (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (949-8899) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.
The first oblique view does not reveal much, but the
other oblique view shows an obvious fracture of the
lateral (external) condyle. This diagnosis makes sense
based on the patient's physical exam. This fracture
typically produces a larger than expected degree of
swelling.
One might consider that this fragment over the
lateral condyle is the ossification center of the external
epicondyle (lateral condyle); however, this ossification
center does not have this appearance. In addition, this
ossification center is the last to appear in the elbow.
The ossification center of the olecranon appears before
this. Since the olecranon's ossification center is not
visible (see lateral view), the external epicondyle will not
be ossified yet. The mnemonic CRITOE is useful to
remember the sequence of appearance of the elbow
ossification centers (Capitellum, Radial Head, Internal
epicondyle, Trochlea, Olecranon, and External
epicondyle). See Case 11 (Elbow Ossification Centers
in a Child) for more details.
In retrospect, this fracture is visible on the AP
view. Go back and examine the lateral condyle region
of the AP view. Magnify the view to examine it closely.
View AP and lateral view above:
Discussion & Teaching Points:
1) A swollen elbow usually contains a fracture
injury. In some instances, a joint effusion (posterior fat
pad sign or enlarged anterior fat pad sign) can be seen
in the absence of a visible fracture. Occult fractures
may still be present in such cases. It is prudent to treat
such an injury as a non-displaced fracture, with a splint,
sling, and follow-up with a primary care physician or
orthopedic surgeon.
2) When uncertainty exists, careful examination of
the patient will often help guide your review of the
radiographs and the need to request special views.
3) Occult fractures in the elbow may be difficult to
identify. Areas that are commonly fractured include the
supracondylar region, the radial head, and the lateral
condyle.
4) Even with special views, not all fractures are
radiographically visible. Other imaging modalities such
as bone scanning, CT scanning, and MRI scanning
have all identified fractures in patients with normal
radiographs. Normal radiographs are not able to totally
rule out fractures. It is often beneficial to advise
patients of the limitation of radiographs. In any
musculoskeletal injury, persistent pain should prompt
the patient to seek medical care even if their initial set
of radiographs was normal. Orthopedic referral, a
repeat set of radiographs, or an advanced imaging
modality should be considered in injuries resulting in
persistent pain.
5) It is useful to include a standardized instruction
sheet to patients whenever radiographs are obtained in
the emergency department. This instruction sheet
should explain the possibility of interpretation errors,
differences of opinion in the radiographic interpretation,
the limitation of radiographs, and instructions for
follow-up. Such an instruction sheet can substantially
reduce the number of patient complaints regarding
misinterpreted radiographs and reduce the ED's liability
potential. An example of such an instruction sheet
follows:
1. The emergency physician has read your X-ray
as: Normal elbow (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (949-8899) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.
Return to Radiology Cases In Ped Emerg Med Case Selection Page
Return to Univ. Hawaii Dept. Pediatrics Home Page
 Although these radiographs appear to be normal,
the patient obviously has something wrong with his
elbow. Diagnosing a sprain of the elbow is a pitfall that
should be avoided. When the patient has obvious
clinical findings around the elbow, examine the
radiographs carefully for a posterior fat pad sign, a
supracondylar fracture, a radial head fracture, and
misplaced ossification centers that may represent
fractures.
In this case, none of these are visible on the
radiographs, which should lead one to be suspicious of
an occult fracture not radiographically visible. In this
case, two oblique views of the elbow were obtained.
View oblique films.
Although these radiographs appear to be normal,
the patient obviously has something wrong with his
elbow. Diagnosing a sprain of the elbow is a pitfall that
should be avoided. When the patient has obvious
clinical findings around the elbow, examine the
radiographs carefully for a posterior fat pad sign, a
supracondylar fracture, a radial head fracture, and
misplaced ossification centers that may represent
fractures.
In this case, none of these are visible on the
radiographs, which should lead one to be suspicious of
an occult fracture not radiographically visible. In this
case, two oblique views of the elbow were obtained.
View oblique films.
 The first oblique view does not reveal much, but the
other oblique view shows an obvious fracture of the
lateral (external) condyle. This diagnosis makes sense
based on the patient's physical exam. This fracture
typically produces a larger than expected degree of
swelling.
One might consider that this fragment over the
lateral condyle is the ossification center of the external
epicondyle (lateral condyle); however, this ossification
center does not have this appearance. In addition, this
ossification center is the last to appear in the elbow.
The ossification center of the olecranon appears before
this. Since the olecranon's ossification center is not
visible (see lateral view), the external epicondyle will not
be ossified yet. The mnemonic CRITOE is useful to
remember the sequence of appearance of the elbow
ossification centers (Capitellum, Radial Head, Internal
epicondyle, Trochlea, Olecranon, and External
epicondyle). See Case 11 (Elbow Ossification Centers
in a Child) for more details.
In retrospect, this fracture is visible on the AP
view. Go back and examine the lateral condyle region
of the AP view. Magnify the view to examine it closely.
View AP and lateral view above:
Discussion & Teaching Points:
1) A swollen elbow usually contains a fracture
injury. In some instances, a joint effusion (posterior fat
pad sign or enlarged anterior fat pad sign) can be seen
in the absence of a visible fracture. Occult fractures
may still be present in such cases. It is prudent to treat
such an injury as a non-displaced fracture, with a splint,
sling, and follow-up with a primary care physician or
orthopedic surgeon.
2) When uncertainty exists, careful examination of
the patient will often help guide your review of the
radiographs and the need to request special views.
3) Occult fractures in the elbow may be difficult to
identify. Areas that are commonly fractured include the
supracondylar region, the radial head, and the lateral
condyle.
4) Even with special views, not all fractures are
radiographically visible. Other imaging modalities such
as bone scanning, CT scanning, and MRI scanning
have all identified fractures in patients with normal
radiographs. Normal radiographs are not able to totally
rule out fractures. It is often beneficial to advise
patients of the limitation of radiographs. In any
musculoskeletal injury, persistent pain should prompt
the patient to seek medical care even if their initial set
of radiographs was normal. Orthopedic referral, a
repeat set of radiographs, or an advanced imaging
modality should be considered in injuries resulting in
persistent pain.
5) It is useful to include a standardized instruction
sheet to patients whenever radiographs are obtained in
the emergency department. This instruction sheet
should explain the possibility of interpretation errors,
differences of opinion in the radiographic interpretation,
the limitation of radiographs, and instructions for
follow-up. Such an instruction sheet can substantially
reduce the number of patient complaints regarding
misinterpreted radiographs and reduce the ED's liability
potential. An example of such an instruction sheet
follows:
1. The emergency physician has read your X-ray
as: Normal elbow (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (949-8899) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.
The first oblique view does not reveal much, but the
other oblique view shows an obvious fracture of the
lateral (external) condyle. This diagnosis makes sense
based on the patient's physical exam. This fracture
typically produces a larger than expected degree of
swelling.
One might consider that this fragment over the
lateral condyle is the ossification center of the external
epicondyle (lateral condyle); however, this ossification
center does not have this appearance. In addition, this
ossification center is the last to appear in the elbow.
The ossification center of the olecranon appears before
this. Since the olecranon's ossification center is not
visible (see lateral view), the external epicondyle will not
be ossified yet. The mnemonic CRITOE is useful to
remember the sequence of appearance of the elbow
ossification centers (Capitellum, Radial Head, Internal
epicondyle, Trochlea, Olecranon, and External
epicondyle). See Case 11 (Elbow Ossification Centers
in a Child) for more details.
In retrospect, this fracture is visible on the AP
view. Go back and examine the lateral condyle region
of the AP view. Magnify the view to examine it closely.
View AP and lateral view above:
Discussion & Teaching Points:
1) A swollen elbow usually contains a fracture
injury. In some instances, a joint effusion (posterior fat
pad sign or enlarged anterior fat pad sign) can be seen
in the absence of a visible fracture. Occult fractures
may still be present in such cases. It is prudent to treat
such an injury as a non-displaced fracture, with a splint,
sling, and follow-up with a primary care physician or
orthopedic surgeon.
2) When uncertainty exists, careful examination of
the patient will often help guide your review of the
radiographs and the need to request special views.
3) Occult fractures in the elbow may be difficult to
identify. Areas that are commonly fractured include the
supracondylar region, the radial head, and the lateral
condyle.
4) Even with special views, not all fractures are
radiographically visible. Other imaging modalities such
as bone scanning, CT scanning, and MRI scanning
have all identified fractures in patients with normal
radiographs. Normal radiographs are not able to totally
rule out fractures. It is often beneficial to advise
patients of the limitation of radiographs. In any
musculoskeletal injury, persistent pain should prompt
the patient to seek medical care even if their initial set
of radiographs was normal. Orthopedic referral, a
repeat set of radiographs, or an advanced imaging
modality should be considered in injuries resulting in
persistent pain.
5) It is useful to include a standardized instruction
sheet to patients whenever radiographs are obtained in
the emergency department. This instruction sheet
should explain the possibility of interpretation errors,
differences of opinion in the radiographic interpretation,
the limitation of radiographs, and instructions for
follow-up. Such an instruction sheet can substantially
reduce the number of patient complaints regarding
misinterpreted radiographs and reduce the ED's liability
potential. An example of such an instruction sheet
follows:
1. The emergency physician has read your X-ray
as: Normal elbow (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (949-8899) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.