Fractured Radius From a Fall, Rule-Out Foot Fracture
Radiology Cases in Pediatric Emergency Medicine
Volume 4, Case 14
Loren G. Yamamoto, MD, MPH
Kapiolani Medical Center For Women And Children
University of Hawaii John A. Burns School of Medicine
This is a 10-year old male who fell down three stairs
yesterday afternoon. He now presents to the
emergency department (20 hours later) complaining of
persistent pain in his right wrist and left foot. He denies
head trauma or symptoms of head injury.
Exam VS T37.2 (tympanic), P80, R20, BP 125/65.
There is point tenderness over the distal radius. There
is slight swelling in this area but no deformity. There is
no scaphoid tenderness. Neurovascular testing distally
is intact. There is diffuse tenderness over the dorsal
lateral portion of his left foot. There is no swelling
evident. He bears weight well on both feet.
Radiographs of his right wrist and left foot are
obtained. The wrist films demonstrate a non-displaced
distal radius torus fracture. A volar splint is placed.
Orthopedic follow-up is arranged.
View left foot radiographs.
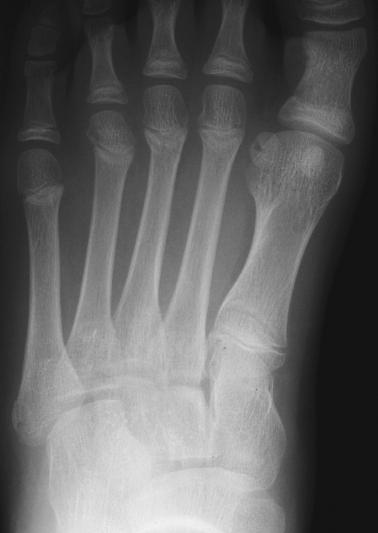

 Examine these radiographs for any abnormalities.
What type of imaging study would you order at this
point? 1) Nuclear bone scan, 2) CT scan, 3) Clinical
follow-up without further imaging studies.
The paragraph above is merely a distraction. It
attempts to lull you into believing that these radiographs
are normal. However, these radiographs would not be
displayed here if they are normal. You are fortunate
since you now know that these radiographs are
somehow abnormal. Unfortunately in the emergency
department, we are not afforded this luxury. While we
try to examine all radiographs carefully, the degree of
scrutiny that we apply to a radiograph is proportional to
our degree of clinical suspicion of an abnormality. In
this case, the suspicion of a foot fracture is low since
his tenderness is not focal, there is no swelling, he
presents on the day after the injury, and he can bear
weight well on the foot. All of these clinical factors
suggest that the likelihood of fracture is low.
Unfortunately, it is these low risk cases that tend to
have small fractures that are the most difficult to
identify. They demand maximal scrutiny in order to find
them. Cases in which we expect to find a fracture, are
usually more obvious radiographically. Thus, the cases
with the most difficult fractures to identify on
radiographs, are usually the radiographs which we
examine with the least scrutiny.
Fortunately, most orthopedic abnormalities missed
on the initial interpretation of radiographs are small
(that's why they are missed) and not of major clinical
consequence. These small injuries can usually be
treated at follow-up. When fractures are not identified
during the initial emergency department visit, patients
are usually dissatisfied with their emergency care since
the patient expected to find a fracture (that's why they
came to the E.D. in the first place), and the physician
failed to find it. These missed fractures often result in
complaints. Such complaints can usually be prevented
if you inform the patient during the initial E.D. visit that a
radiologist, reading the radiographs later, may have a
different interpretation of the radiographs. If an occult
fracture is suspected despite negative radiographs, it
may be prudent to splint the injury pending clinical
follow-up and a second opinion from a radiologist.
You have one more chance to scrutinize our
patient's foot radiographs to identify any abnormalities.
Examine these radiographs for any abnormalities.
What type of imaging study would you order at this
point? 1) Nuclear bone scan, 2) CT scan, 3) Clinical
follow-up without further imaging studies.
The paragraph above is merely a distraction. It
attempts to lull you into believing that these radiographs
are normal. However, these radiographs would not be
displayed here if they are normal. You are fortunate
since you now know that these radiographs are
somehow abnormal. Unfortunately in the emergency
department, we are not afforded this luxury. While we
try to examine all radiographs carefully, the degree of
scrutiny that we apply to a radiograph is proportional to
our degree of clinical suspicion of an abnormality. In
this case, the suspicion of a foot fracture is low since
his tenderness is not focal, there is no swelling, he
presents on the day after the injury, and he can bear
weight well on the foot. All of these clinical factors
suggest that the likelihood of fracture is low.
Unfortunately, it is these low risk cases that tend to
have small fractures that are the most difficult to
identify. They demand maximal scrutiny in order to find
them. Cases in which we expect to find a fracture, are
usually more obvious radiographically. Thus, the cases
with the most difficult fractures to identify on
radiographs, are usually the radiographs which we
examine with the least scrutiny.
Fortunately, most orthopedic abnormalities missed
on the initial interpretation of radiographs are small
(that's why they are missed) and not of major clinical
consequence. These small injuries can usually be
treated at follow-up. When fractures are not identified
during the initial emergency department visit, patients
are usually dissatisfied with their emergency care since
the patient expected to find a fracture (that's why they
came to the E.D. in the first place), and the physician
failed to find it. These missed fractures often result in
complaints. Such complaints can usually be prevented
if you inform the patient during the initial E.D. visit that a
radiologist, reading the radiographs later, may have a
different interpretation of the radiographs. If an occult
fracture is suspected despite negative radiographs, it
may be prudent to splint the injury pending clinical
follow-up and a second opinion from a radiologist.
You have one more chance to scrutinize our
patient's foot radiographs to identify any abnormalities.


 These radiographs show non-displaced fractures of
the distal second, third, and fourth metatarsals. The
second and third metatarsals fractures involve the
metaphysis. The third metatarsal fracture is a
Salter-Harris type II fracture involving the metaphysis
extending into the physis (growth plate). The fourth
metatarsal fracture involves the epiphysis. Note that it
extends from the epiphysis into the physis and possibly
into the metaphysis. This is a Salter-Harris type III or
type IV fracture. Point tenderness was not appreciated
on examination since more than one fracture is present
in the foot. Refer to Case 18 of Volume 1,
Salter-Harris, for more discussion on the Salter-Harris
classification of fractures involving the growth plate.
View a focused view of these areas.
These radiographs show non-displaced fractures of
the distal second, third, and fourth metatarsals. The
second and third metatarsals fractures involve the
metaphysis. The third metatarsal fracture is a
Salter-Harris type II fracture involving the metaphysis
extending into the physis (growth plate). The fourth
metatarsal fracture involves the epiphysis. Note that it
extends from the epiphysis into the physis and possibly
into the metaphysis. This is a Salter-Harris type III or
type IV fracture. Point tenderness was not appreciated
on examination since more than one fracture is present
in the foot. Refer to Case 18 of Volume 1,
Salter-Harris, for more discussion on the Salter-Harris
classification of fractures involving the growth plate.
View a focused view of these areas.
 The upper image is taken from the AP view and the
lower image is taken from the oblique view.
The fractures are pointed out below.
The upper image is taken from the AP view and the
lower image is taken from the oblique view.
The fractures are pointed out below.
 The black arrows point out the metaphyseal
fractures of the second and third metatarsals. The third
metatarsal fracture is evident. The second metatarsal
fracture is not obvious, but the angle of the metaphysis
where the arrow is pointing, is sharper than it should be.
The white outlined arrow points out the lateral
epiphyseal fracture of the fourth metatarsal. The
lucency on the medial side of the fourth metatarsal
epiphysis is also a fracture (no arrow).
If you failed to identify all the fractures in his foot,
your patient may be less than satisfied even though
splinting the foot would be an appropriate initial
management for the fractures. One suggestion as
pointed out in Case 19 of Volume 1 is to routinely
discharge all patients with a form such as that below if
radiographs are ordered:
1. The emergency physician has read your X-ray
as: Normal foot (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (999-9999) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days, could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.
The black arrows point out the metaphyseal
fractures of the second and third metatarsals. The third
metatarsal fracture is evident. The second metatarsal
fracture is not obvious, but the angle of the metaphysis
where the arrow is pointing, is sharper than it should be.
The white outlined arrow points out the lateral
epiphyseal fracture of the fourth metatarsal. The
lucency on the medial side of the fourth metatarsal
epiphysis is also a fracture (no arrow).
If you failed to identify all the fractures in his foot,
your patient may be less than satisfied even though
splinting the foot would be an appropriate initial
management for the fractures. One suggestion as
pointed out in Case 19 of Volume 1 is to routinely
discharge all patients with a form such as that below if
radiographs are ordered:
1. The emergency physician has read your X-ray
as: Normal foot (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (999-9999) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days, could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.
Return to Radiology Cases In Ped Emerg Med Case Selection Page
Return to Univ. Hawaii Dept. Pediatrics Home Page


 Examine these radiographs for any abnormalities.
What type of imaging study would you order at this
point? 1) Nuclear bone scan, 2) CT scan, 3) Clinical
follow-up without further imaging studies.
The paragraph above is merely a distraction. It
attempts to lull you into believing that these radiographs
are normal. However, these radiographs would not be
displayed here if they are normal. You are fortunate
since you now know that these radiographs are
somehow abnormal. Unfortunately in the emergency
department, we are not afforded this luxury. While we
try to examine all radiographs carefully, the degree of
scrutiny that we apply to a radiograph is proportional to
our degree of clinical suspicion of an abnormality. In
this case, the suspicion of a foot fracture is low since
his tenderness is not focal, there is no swelling, he
presents on the day after the injury, and he can bear
weight well on the foot. All of these clinical factors
suggest that the likelihood of fracture is low.
Unfortunately, it is these low risk cases that tend to
have small fractures that are the most difficult to
identify. They demand maximal scrutiny in order to find
them. Cases in which we expect to find a fracture, are
usually more obvious radiographically. Thus, the cases
with the most difficult fractures to identify on
radiographs, are usually the radiographs which we
examine with the least scrutiny.
Fortunately, most orthopedic abnormalities missed
on the initial interpretation of radiographs are small
(that's why they are missed) and not of major clinical
consequence. These small injuries can usually be
treated at follow-up. When fractures are not identified
during the initial emergency department visit, patients
are usually dissatisfied with their emergency care since
the patient expected to find a fracture (that's why they
came to the E.D. in the first place), and the physician
failed to find it. These missed fractures often result in
complaints. Such complaints can usually be prevented
if you inform the patient during the initial E.D. visit that a
radiologist, reading the radiographs later, may have a
different interpretation of the radiographs. If an occult
fracture is suspected despite negative radiographs, it
may be prudent to splint the injury pending clinical
follow-up and a second opinion from a radiologist.
You have one more chance to scrutinize our
patient's foot radiographs to identify any abnormalities.
Examine these radiographs for any abnormalities.
What type of imaging study would you order at this
point? 1) Nuclear bone scan, 2) CT scan, 3) Clinical
follow-up without further imaging studies.
The paragraph above is merely a distraction. It
attempts to lull you into believing that these radiographs
are normal. However, these radiographs would not be
displayed here if they are normal. You are fortunate
since you now know that these radiographs are
somehow abnormal. Unfortunately in the emergency
department, we are not afforded this luxury. While we
try to examine all radiographs carefully, the degree of
scrutiny that we apply to a radiograph is proportional to
our degree of clinical suspicion of an abnormality. In
this case, the suspicion of a foot fracture is low since
his tenderness is not focal, there is no swelling, he
presents on the day after the injury, and he can bear
weight well on the foot. All of these clinical factors
suggest that the likelihood of fracture is low.
Unfortunately, it is these low risk cases that tend to
have small fractures that are the most difficult to
identify. They demand maximal scrutiny in order to find
them. Cases in which we expect to find a fracture, are
usually more obvious radiographically. Thus, the cases
with the most difficult fractures to identify on
radiographs, are usually the radiographs which we
examine with the least scrutiny.
Fortunately, most orthopedic abnormalities missed
on the initial interpretation of radiographs are small
(that's why they are missed) and not of major clinical
consequence. These small injuries can usually be
treated at follow-up. When fractures are not identified
during the initial emergency department visit, patients
are usually dissatisfied with their emergency care since
the patient expected to find a fracture (that's why they
came to the E.D. in the first place), and the physician
failed to find it. These missed fractures often result in
complaints. Such complaints can usually be prevented
if you inform the patient during the initial E.D. visit that a
radiologist, reading the radiographs later, may have a
different interpretation of the radiographs. If an occult
fracture is suspected despite negative radiographs, it
may be prudent to splint the injury pending clinical
follow-up and a second opinion from a radiologist.
You have one more chance to scrutinize our
patient's foot radiographs to identify any abnormalities.


 These radiographs show non-displaced fractures of
the distal second, third, and fourth metatarsals. The
second and third metatarsals fractures involve the
metaphysis. The third metatarsal fracture is a
Salter-Harris type II fracture involving the metaphysis
extending into the physis (growth plate). The fourth
metatarsal fracture involves the epiphysis. Note that it
extends from the epiphysis into the physis and possibly
into the metaphysis. This is a Salter-Harris type III or
type IV fracture. Point tenderness was not appreciated
on examination since more than one fracture is present
in the foot. Refer to Case 18 of Volume 1,
Salter-Harris, for more discussion on the Salter-Harris
classification of fractures involving the growth plate.
View a focused view of these areas.
These radiographs show non-displaced fractures of
the distal second, third, and fourth metatarsals. The
second and third metatarsals fractures involve the
metaphysis. The third metatarsal fracture is a
Salter-Harris type II fracture involving the metaphysis
extending into the physis (growth plate). The fourth
metatarsal fracture involves the epiphysis. Note that it
extends from the epiphysis into the physis and possibly
into the metaphysis. This is a Salter-Harris type III or
type IV fracture. Point tenderness was not appreciated
on examination since more than one fracture is present
in the foot. Refer to Case 18 of Volume 1,
Salter-Harris, for more discussion on the Salter-Harris
classification of fractures involving the growth plate.
View a focused view of these areas.
 The upper image is taken from the AP view and the
lower image is taken from the oblique view.
The fractures are pointed out below.
The upper image is taken from the AP view and the
lower image is taken from the oblique view.
The fractures are pointed out below.
 The black arrows point out the metaphyseal
fractures of the second and third metatarsals. The third
metatarsal fracture is evident. The second metatarsal
fracture is not obvious, but the angle of the metaphysis
where the arrow is pointing, is sharper than it should be.
The white outlined arrow points out the lateral
epiphyseal fracture of the fourth metatarsal. The
lucency on the medial side of the fourth metatarsal
epiphysis is also a fracture (no arrow).
If you failed to identify all the fractures in his foot,
your patient may be less than satisfied even though
splinting the foot would be an appropriate initial
management for the fractures. One suggestion as
pointed out in Case 19 of Volume 1 is to routinely
discharge all patients with a form such as that below if
radiographs are ordered:
1. The emergency physician has read your X-ray
as: Normal foot (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (999-9999) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days, could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.
The black arrows point out the metaphyseal
fractures of the second and third metatarsals. The third
metatarsal fracture is evident. The second metatarsal
fracture is not obvious, but the angle of the metaphysis
where the arrow is pointing, is sharper than it should be.
The white outlined arrow points out the lateral
epiphyseal fracture of the fourth metatarsal. The
lucency on the medial side of the fourth metatarsal
epiphysis is also a fracture (no arrow).
If you failed to identify all the fractures in his foot,
your patient may be less than satisfied even though
splinting the foot would be an appropriate initial
management for the fractures. One suggestion as
pointed out in Case 19 of Volume 1 is to routinely
discharge all patients with a form such as that below if
radiographs are ordered:
1. The emergency physician has read your X-ray
as: Normal foot (example)
2. Large abnormalities requiring urgent care are
generally obvious and, therefore, this is unlikely at this
point. An emergency physician can find most of the
problems on an X-ray, but the emergency physician is
not a specialist in radiology.
3. To be sure, we will have the hospital radiologist
(X-ray specialist) read your X-ray on the morning of the
next working day (Monday through Saturday). If there
is an important difference in the X-ray reading, we will
try to call you or your doctor, but this doesn't always
happen. To double check us, please call your physician
or the hospital clinic (999-9999) to find out how your
X-ray is being read by the radiologist. If you call the
hospital X-ray department directly, they will not give you
the reading over the phone since the medical reading is
not understood by most people. It must be done
through your doctor.
4. When you call your doctor or your doctor's office
nurse, tell him/her that you came to the Emergency
Department where some X-rays were taken, and you
were told to call your doctor to double-check the X-ray
reading with the hospital radiologist. The most
common things that are missed on X-ray readings are
tiny fractures (cracks, chips, or hairlines) and small
areas of infection (bronchitis, pneumonia, bone
infection, etc.).
5. To be sure that these problems are not there, it is
important that you contact your physician so that you
will receive the proper care for this condition.
6. For injuries, pain that lasts for more than a week
or pain that doesn't get better after two days, could
mean that you have a hidden broken bone, even if your
X-rays are normal (X-rays cannot find all broken
bones). See your doctor for an examination of the
area. Another set of X-rays may be needed.