Near Drowning
Radiology Cases in Pediatric Emergency Medicine
Volume 5, Case 15
Meri-Mika Morisada, MD
Kapiolani Medical Center For Women And Children
University of Hawaii John A. Burns School of Medicine
This is an 11-month old female who experienced a
near-drowning episode in a bathtub. She had been
placed in a bathtub approximately one-fourth full of
water by her mother. Her mother then left the child
unattended and went to the restroom herself. The child
was behind the shower curtain. The mother was gone
approximately five minutes, and upon returning she
found the child floating in the water face up without any
respiratory effort. She immediately grabbed the infant
out of the bathtub, took her to the closest bed and
attempted mouth-to-mouth resuscitation and some
chest compressions. She called 911 at that time.
Immediately prior to the arrival of the ambulance, the
mother noted spontaneous respirations. Paramedics
initiated positive pressure ventilation with a bag and
mask apparatus. Five minutes later, they arrived at the
E.D. at which time the infant was noted to be crying.
Exam: VS T 36.5, P 120, R 45, BP 130/50, oxygen
saturation while on supplemental oxygen (exact FiO2
not known) and continuous positive airway pressure
was 98%. She was crying and active. Head without
signs of trauma. Eyes normal. Pupils equal and
reactive. Neck supple. Heart regular. Lungs
spontaneous respirations with bilateral wheezing and
rales. Good air exchange. Abdomen benign.
Extremities with good pulses and perfusion. No
evidence of trauma. Neuro: active, crying, recognizes
mother, interactive with mother. Muscle tone good.
Cardiac and pulse oximetry monitors were placed.
A Foley catheter and nasogastric tube were placed.
200cc of fluid was evacuated from the stomach. Initial
ABG: pH 7.11, pCO2 27, pO2 140, bicarb 9.
Electrolytes Na 125, K 4.0, Cl 92, bicarb 11. Glucose
245. WBC 29,500 with 5% segs, 1% bands, 92%
lymphs. Hgb 12.3, Hct 35.8, platelets 394,000. A chest
radiograph was obtained.
View chest radiograph.
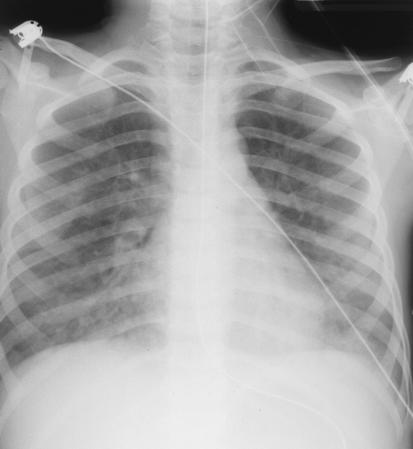 She was treated with sodium bicarbonate for
metabolic acidosis, aerosolized albuterol for wheezing
and furosemide for pulmonary edema. The CXR shows
small patchy basilar pulmonary infiltrates.
She improves clinically and her chest radiograph is
repeated two days later.
View follow-up chest radiograph.
She was treated with sodium bicarbonate for
metabolic acidosis, aerosolized albuterol for wheezing
and furosemide for pulmonary edema. The CXR shows
small patchy basilar pulmonary infiltrates.
She improves clinically and her chest radiograph is
repeated two days later.
View follow-up chest radiograph.
 Her chest radiograph is now normal.
Discussion
Drowning is defined as death within 24 hours as a
result of submersion. "Near drowning" refers to survival
beyond 24 hours of the submersion episode. The
majority of accidents occur in swimming pools, ponds,
lakes and bathtubs, with a peak incidence in children at
less than 4 years of age and a second peak during the
risk-taking age group of 15-24 years. Among boys
15-19 years, 38% of drownings are alcohol related.
Pathophysiologically, the problems commonly seen in a
submersion accident are:
1. Hypoxia
2. Hypothermia (EXCEPT when submersion occurs
in water greater than body temperature)
3. Aspiration (which can impair lung function and
aggravate existing hypoxia after breathing is restored)
Hypoxia is the primary problem. The clinical
manifestations of hypoxia are related to both the
severity of hypoxia and the differing abilities of
individual organs to tolerate hypoxia. The brain cortex
is the first to sustain irreversible damage. The lower
brain is next. The lungs and heart can tolerate up to
20-30 minutes of hypoxia and survive with appropriate
post-rescue support.
Hypothermia: This phenomenon explains the good
outcome of victims who are submerged in icy waters for
up to 45 minutes (and occasionally longer). When
submerged in icy cold water, the body temperature
drops rapidly to a point where body activity and
metabolism come to a virtual standstill. If this standstill
develops before available oxygen is completely used,
the hypothermia confers a protective effect. The
remaining oxygen is used slowly and the body can
survive submersion for a longer period of time before
irreversible anoxic tissue damage develops. In most
other instances, (non-icy water drowning), the victim's
temperature will drop too slowly to confer any protective
effect.
Aspiration: Experience indicates that saltwater and
freshwater aspiration do not produce significantly
different respiratory injury patterns. If large amounts
are swallowed, hypo or hypernatremia may result from
fresh or salt water submersions, respectively.
Respiratory infection is possible, but antibiotics should
be reserved for proven infection or when grossly
contaminated water is aspirated.
Clinical Manifestations
In the first moments after rescue, the appearance of
the child who has nearly drowned may range from
apparently normal to apparently dead. Body
temperature is frequently low, even in temperate,
warm-water environments. Respiratory efforts may be
absent, irregular, or labored, with pallor or cyanosis,
retractions, grunting, and cough productive of pink,
frothy material. The lungs may be clear, or there may
be rales, rhonchi and wheezing. Infection may develop
as a consequence of aspirated mouth flora or
organisms in stagnant water, but this is not usually
important in the first 24 hours.
Respiratory function may improve spontaneously or
deteriorate rapidly as pulmonary edema and small
airway dysfunction worsens.
Neurologic assessment may show an alert, normal
child or any level of CNS compromise. A child may
display agitation and combative behavior, seizures,
blunted responsiveness to the environment, or profound
coma with stereotypic posturing or flaccid extremities.
Superficial evidence of head trauma may be noted in a
few children whose submersion episode is a secondary
event.
Conn and Baker devised a classification of
submersion victims based on neurologic function since
the CNS is the system most susceptible to damage
from hypoxia. The classification is useful for 3 reasons:
1) it allows one to estimate the magnitude of the
hypoxic insult; 2) it guides one in the selection of
appropriate therapy; 3) it is highly predictive of patient
outcome.
They suggest the classification be made on patient
findings within the first hour of retrieval from water.
Patient classification by Conn and Baker divides the
patient into categories A,B,C1-4.
Category:
A: Awake = Alert, fully conscious, minimal injury
B: Blunted = Obtunded to stuporous, normal central
respiratory drive and other brain stem functions.
C: Comatose = Unarousable, abnormal brain stem
function, abnormal central respiratory pattern, abnormal
motor responses to painful stimuli. May have seizures.
Respiratory failure present. Category C patients may
be further subdivided:
C1: Decorticate. Flexor posturing. Cheyne-Stokes
respirations
C2: Decerebrate. Extensor posturing. Central
hyperventilation
C3: Flaccid. Apneustic or cluster breathing
C4: Deceased? Flaccid, apneic, no detectable
circulation
Prediction of submersion victim outcome can be
reduced to the following observation: If the victim has
not sustained a cardiac arrest, the potential for intact
survival is good when appropriate resuscitation and
prehospital care are provided.
Patients in categories A and B almost uniformly do
well with medical supportive therapy alone; intact
survival is the rule. A few category B patients develop
respiratory failure severe enough to require mechanical
ventilation, usually from aspiration.
Patients in category C are in respiratory failure and
require intensive therapy and monitoring. Patient
outcomes vary. A very high percentage of category C1
and C2 have normal outcomes. A significant portion of
C3 patients survive, but there is a substantial increase
in their incidence of death or survival with
anoxic-ischemic encephalopathy. C4 patients do
poorly. The majority die or survive with profound
anoxic-ischemic encephalopathy.
Note that all submersion victims may be apneic
when retrieved from the water since apnea is a
common reflex when the face is immersed in cold water
even if they have not sustained a cardiac arrest. Since
submersion victims with excellent prognosis may
initially be found apneic, vigorous initial resuscitation
measures should be attempted in all submersion
victims. Our patient was a Category A patient and did
quite well as predicted. The hypoxia was mild, and
neurologic functioning was good. Although she was felt
to have aspirated, antibiotics are reserved for proven
infection or when grossly contaminated water is
aspirated. For these reasons, this patient did not
receive antibiotics. She was observed for 24 hours, as
there may be a pulmonary inflammatory response
24-48 hours after the insult.
Immediate evaluation:
1. Consider: ABG, CBC, electrolytes, CXR.
2. Look for associated problems: head, neck, other
injuries; ingestion; possibility of a seizure (primary or
resulting from trauma, hypoxia, hyponatremia). Further
tests after stabilization to be considered are CT scan of
head, radiographs of the cervical spine, drug screen
(eg., alcohol).
Management - Category A:
1. Supplemental oxygen.
2. Aerosolized beta-adrenergic agents for wheezing
(albuterol).
3. Consider diuretic (furosemide) for pulmonary
edema seen on CXR.
4. Sodium bicarbonate. Give 1 meq/kg for pH 7.1
or less. As oxygenation improves, the acidosis will also
resolve.
5. Drying and warming measures.
6. Consider NG tube placement to prevent
aspiration and decompress the stomach. Excessive
stomach contents could elevate the diaphragm and
restrict thoracic volume.
Management - Category B:
1. The above measures plus:
2. Intubation usually is not needed.
3. Electrolyte disturbances: Hyponatremia may
occur if large amounts of fresh water are swallowed.
Hypernatremia may occur if salt water has been
swallowed.
4. Start an IV at maintenance or slightly less than
maintenance to prevent further pulmonary compromise.
5. Consider antibiotics for aspiration of
contaminated contents. Note that leukocytosis is a
common stress response and is not indicative of
infection.
Management - Category C:
1. Apply the above measures plus:
2. Intubate and ventilate, as all C patients are
comatose and have respiratory failure. High distending
pressures are usually required.
3. Monitor EKG for dysrhythmias. Hypotension
may also occur.
4. In addition to sodium abnormalities, hyperkalemia
from metabolic acidosis may occur.
5. Treat seizures (primary or from electrolyte
abnormalities, hypoxia, trauma).
6. Hyperglycemia is a stress response. There is
usually no need to treat this.
7. Leukocytosis, as mentioned, is an expected
stress response. Leukopenia can occur in profound
hypoxia. Consider antibiotics for aspiration of dirty
water.
Prevention
1. Educate caretakers to potential submersion risks
of bathtubs, water pails, pools, lakes, streams and the
ocean. Stress the need for close supervision by a
responsible adult.
2. Neighborhood and private swimming pools
should ideally be surrounded by a double barrier (eg.,
two sets of fences). If a single barrier is used to
surround the pool, the house should NOT be used as
part of the barrier.
3. Encourage swimming lessons for all patients.
However, water safety is not solely dependent on one's
ability to swim. An overall understanding of water
safety to avoid risk-taking behavior is necessary to
minimize risk. For example, a 9-year old who can swim
in a pool will easily drown in ocean surf or a rapidly
flowing stream.
4. Encourage caretakers to learn CPR
References
Aoki B. Evaluation, stabilization, and transportation
of the critically ill child. Mosby Yearbook, 1992,
pp.237-251.
Her chest radiograph is now normal.
Discussion
Drowning is defined as death within 24 hours as a
result of submersion. "Near drowning" refers to survival
beyond 24 hours of the submersion episode. The
majority of accidents occur in swimming pools, ponds,
lakes and bathtubs, with a peak incidence in children at
less than 4 years of age and a second peak during the
risk-taking age group of 15-24 years. Among boys
15-19 years, 38% of drownings are alcohol related.
Pathophysiologically, the problems commonly seen in a
submersion accident are:
1. Hypoxia
2. Hypothermia (EXCEPT when submersion occurs
in water greater than body temperature)
3. Aspiration (which can impair lung function and
aggravate existing hypoxia after breathing is restored)
Hypoxia is the primary problem. The clinical
manifestations of hypoxia are related to both the
severity of hypoxia and the differing abilities of
individual organs to tolerate hypoxia. The brain cortex
is the first to sustain irreversible damage. The lower
brain is next. The lungs and heart can tolerate up to
20-30 minutes of hypoxia and survive with appropriate
post-rescue support.
Hypothermia: This phenomenon explains the good
outcome of victims who are submerged in icy waters for
up to 45 minutes (and occasionally longer). When
submerged in icy cold water, the body temperature
drops rapidly to a point where body activity and
metabolism come to a virtual standstill. If this standstill
develops before available oxygen is completely used,
the hypothermia confers a protective effect. The
remaining oxygen is used slowly and the body can
survive submersion for a longer period of time before
irreversible anoxic tissue damage develops. In most
other instances, (non-icy water drowning), the victim's
temperature will drop too slowly to confer any protective
effect.
Aspiration: Experience indicates that saltwater and
freshwater aspiration do not produce significantly
different respiratory injury patterns. If large amounts
are swallowed, hypo or hypernatremia may result from
fresh or salt water submersions, respectively.
Respiratory infection is possible, but antibiotics should
be reserved for proven infection or when grossly
contaminated water is aspirated.
Clinical Manifestations
In the first moments after rescue, the appearance of
the child who has nearly drowned may range from
apparently normal to apparently dead. Body
temperature is frequently low, even in temperate,
warm-water environments. Respiratory efforts may be
absent, irregular, or labored, with pallor or cyanosis,
retractions, grunting, and cough productive of pink,
frothy material. The lungs may be clear, or there may
be rales, rhonchi and wheezing. Infection may develop
as a consequence of aspirated mouth flora or
organisms in stagnant water, but this is not usually
important in the first 24 hours.
Respiratory function may improve spontaneously or
deteriorate rapidly as pulmonary edema and small
airway dysfunction worsens.
Neurologic assessment may show an alert, normal
child or any level of CNS compromise. A child may
display agitation and combative behavior, seizures,
blunted responsiveness to the environment, or profound
coma with stereotypic posturing or flaccid extremities.
Superficial evidence of head trauma may be noted in a
few children whose submersion episode is a secondary
event.
Conn and Baker devised a classification of
submersion victims based on neurologic function since
the CNS is the system most susceptible to damage
from hypoxia. The classification is useful for 3 reasons:
1) it allows one to estimate the magnitude of the
hypoxic insult; 2) it guides one in the selection of
appropriate therapy; 3) it is highly predictive of patient
outcome.
They suggest the classification be made on patient
findings within the first hour of retrieval from water.
Patient classification by Conn and Baker divides the
patient into categories A,B,C1-4.
Category:
A: Awake = Alert, fully conscious, minimal injury
B: Blunted = Obtunded to stuporous, normal central
respiratory drive and other brain stem functions.
C: Comatose = Unarousable, abnormal brain stem
function, abnormal central respiratory pattern, abnormal
motor responses to painful stimuli. May have seizures.
Respiratory failure present. Category C patients may
be further subdivided:
C1: Decorticate. Flexor posturing. Cheyne-Stokes
respirations
C2: Decerebrate. Extensor posturing. Central
hyperventilation
C3: Flaccid. Apneustic or cluster breathing
C4: Deceased? Flaccid, apneic, no detectable
circulation
Prediction of submersion victim outcome can be
reduced to the following observation: If the victim has
not sustained a cardiac arrest, the potential for intact
survival is good when appropriate resuscitation and
prehospital care are provided.
Patients in categories A and B almost uniformly do
well with medical supportive therapy alone; intact
survival is the rule. A few category B patients develop
respiratory failure severe enough to require mechanical
ventilation, usually from aspiration.
Patients in category C are in respiratory failure and
require intensive therapy and monitoring. Patient
outcomes vary. A very high percentage of category C1
and C2 have normal outcomes. A significant portion of
C3 patients survive, but there is a substantial increase
in their incidence of death or survival with
anoxic-ischemic encephalopathy. C4 patients do
poorly. The majority die or survive with profound
anoxic-ischemic encephalopathy.
Note that all submersion victims may be apneic
when retrieved from the water since apnea is a
common reflex when the face is immersed in cold water
even if they have not sustained a cardiac arrest. Since
submersion victims with excellent prognosis may
initially be found apneic, vigorous initial resuscitation
measures should be attempted in all submersion
victims. Our patient was a Category A patient and did
quite well as predicted. The hypoxia was mild, and
neurologic functioning was good. Although she was felt
to have aspirated, antibiotics are reserved for proven
infection or when grossly contaminated water is
aspirated. For these reasons, this patient did not
receive antibiotics. She was observed for 24 hours, as
there may be a pulmonary inflammatory response
24-48 hours after the insult.
Immediate evaluation:
1. Consider: ABG, CBC, electrolytes, CXR.
2. Look for associated problems: head, neck, other
injuries; ingestion; possibility of a seizure (primary or
resulting from trauma, hypoxia, hyponatremia). Further
tests after stabilization to be considered are CT scan of
head, radiographs of the cervical spine, drug screen
(eg., alcohol).
Management - Category A:
1. Supplemental oxygen.
2. Aerosolized beta-adrenergic agents for wheezing
(albuterol).
3. Consider diuretic (furosemide) for pulmonary
edema seen on CXR.
4. Sodium bicarbonate. Give 1 meq/kg for pH 7.1
or less. As oxygenation improves, the acidosis will also
resolve.
5. Drying and warming measures.
6. Consider NG tube placement to prevent
aspiration and decompress the stomach. Excessive
stomach contents could elevate the diaphragm and
restrict thoracic volume.
Management - Category B:
1. The above measures plus:
2. Intubation usually is not needed.
3. Electrolyte disturbances: Hyponatremia may
occur if large amounts of fresh water are swallowed.
Hypernatremia may occur if salt water has been
swallowed.
4. Start an IV at maintenance or slightly less than
maintenance to prevent further pulmonary compromise.
5. Consider antibiotics for aspiration of
contaminated contents. Note that leukocytosis is a
common stress response and is not indicative of
infection.
Management - Category C:
1. Apply the above measures plus:
2. Intubate and ventilate, as all C patients are
comatose and have respiratory failure. High distending
pressures are usually required.
3. Monitor EKG for dysrhythmias. Hypotension
may also occur.
4. In addition to sodium abnormalities, hyperkalemia
from metabolic acidosis may occur.
5. Treat seizures (primary or from electrolyte
abnormalities, hypoxia, trauma).
6. Hyperglycemia is a stress response. There is
usually no need to treat this.
7. Leukocytosis, as mentioned, is an expected
stress response. Leukopenia can occur in profound
hypoxia. Consider antibiotics for aspiration of dirty
water.
Prevention
1. Educate caretakers to potential submersion risks
of bathtubs, water pails, pools, lakes, streams and the
ocean. Stress the need for close supervision by a
responsible adult.
2. Neighborhood and private swimming pools
should ideally be surrounded by a double barrier (eg.,
two sets of fences). If a single barrier is used to
surround the pool, the house should NOT be used as
part of the barrier.
3. Encourage swimming lessons for all patients.
However, water safety is not solely dependent on one's
ability to swim. An overall understanding of water
safety to avoid risk-taking behavior is necessary to
minimize risk. For example, a 9-year old who can swim
in a pool will easily drown in ocean surf or a rapidly
flowing stream.
4. Encourage caretakers to learn CPR
References
Aoki B. Evaluation, stabilization, and transportation
of the critically ill child. Mosby Yearbook, 1992,
pp.237-251.
Return to Radiology Cases In Ped Emerg Med Case Selection Page
Return to Univ. Hawaii Dept. Pediatrics Home Page
 She was treated with sodium bicarbonate for
metabolic acidosis, aerosolized albuterol for wheezing
and furosemide for pulmonary edema. The CXR shows
small patchy basilar pulmonary infiltrates.
She improves clinically and her chest radiograph is
repeated two days later.
View follow-up chest radiograph.
She was treated with sodium bicarbonate for
metabolic acidosis, aerosolized albuterol for wheezing
and furosemide for pulmonary edema. The CXR shows
small patchy basilar pulmonary infiltrates.
She improves clinically and her chest radiograph is
repeated two days later.
View follow-up chest radiograph.
 Her chest radiograph is now normal.
Discussion
Drowning is defined as death within 24 hours as a
result of submersion. "Near drowning" refers to survival
beyond 24 hours of the submersion episode. The
majority of accidents occur in swimming pools, ponds,
lakes and bathtubs, with a peak incidence in children at
less than 4 years of age and a second peak during the
risk-taking age group of 15-24 years. Among boys
15-19 years, 38% of drownings are alcohol related.
Pathophysiologically, the problems commonly seen in a
submersion accident are:
1. Hypoxia
2. Hypothermia (EXCEPT when submersion occurs
in water greater than body temperature)
3. Aspiration (which can impair lung function and
aggravate existing hypoxia after breathing is restored)
Hypoxia is the primary problem. The clinical
manifestations of hypoxia are related to both the
severity of hypoxia and the differing abilities of
individual organs to tolerate hypoxia. The brain cortex
is the first to sustain irreversible damage. The lower
brain is next. The lungs and heart can tolerate up to
20-30 minutes of hypoxia and survive with appropriate
post-rescue support.
Hypothermia: This phenomenon explains the good
outcome of victims who are submerged in icy waters for
up to 45 minutes (and occasionally longer). When
submerged in icy cold water, the body temperature
drops rapidly to a point where body activity and
metabolism come to a virtual standstill. If this standstill
develops before available oxygen is completely used,
the hypothermia confers a protective effect. The
remaining oxygen is used slowly and the body can
survive submersion for a longer period of time before
irreversible anoxic tissue damage develops. In most
other instances, (non-icy water drowning), the victim's
temperature will drop too slowly to confer any protective
effect.
Aspiration: Experience indicates that saltwater and
freshwater aspiration do not produce significantly
different respiratory injury patterns. If large amounts
are swallowed, hypo or hypernatremia may result from
fresh or salt water submersions, respectively.
Respiratory infection is possible, but antibiotics should
be reserved for proven infection or when grossly
contaminated water is aspirated.
Clinical Manifestations
In the first moments after rescue, the appearance of
the child who has nearly drowned may range from
apparently normal to apparently dead. Body
temperature is frequently low, even in temperate,
warm-water environments. Respiratory efforts may be
absent, irregular, or labored, with pallor or cyanosis,
retractions, grunting, and cough productive of pink,
frothy material. The lungs may be clear, or there may
be rales, rhonchi and wheezing. Infection may develop
as a consequence of aspirated mouth flora or
organisms in stagnant water, but this is not usually
important in the first 24 hours.
Respiratory function may improve spontaneously or
deteriorate rapidly as pulmonary edema and small
airway dysfunction worsens.
Neurologic assessment may show an alert, normal
child or any level of CNS compromise. A child may
display agitation and combative behavior, seizures,
blunted responsiveness to the environment, or profound
coma with stereotypic posturing or flaccid extremities.
Superficial evidence of head trauma may be noted in a
few children whose submersion episode is a secondary
event.
Conn and Baker devised a classification of
submersion victims based on neurologic function since
the CNS is the system most susceptible to damage
from hypoxia. The classification is useful for 3 reasons:
1) it allows one to estimate the magnitude of the
hypoxic insult; 2) it guides one in the selection of
appropriate therapy; 3) it is highly predictive of patient
outcome.
They suggest the classification be made on patient
findings within the first hour of retrieval from water.
Patient classification by Conn and Baker divides the
patient into categories A,B,C1-4.
Category:
A: Awake = Alert, fully conscious, minimal injury
B: Blunted = Obtunded to stuporous, normal central
respiratory drive and other brain stem functions.
C: Comatose = Unarousable, abnormal brain stem
function, abnormal central respiratory pattern, abnormal
motor responses to painful stimuli. May have seizures.
Respiratory failure present. Category C patients may
be further subdivided:
C1: Decorticate. Flexor posturing. Cheyne-Stokes
respirations
C2: Decerebrate. Extensor posturing. Central
hyperventilation
C3: Flaccid. Apneustic or cluster breathing
C4: Deceased? Flaccid, apneic, no detectable
circulation
Prediction of submersion victim outcome can be
reduced to the following observation: If the victim has
not sustained a cardiac arrest, the potential for intact
survival is good when appropriate resuscitation and
prehospital care are provided.
Patients in categories A and B almost uniformly do
well with medical supportive therapy alone; intact
survival is the rule. A few category B patients develop
respiratory failure severe enough to require mechanical
ventilation, usually from aspiration.
Patients in category C are in respiratory failure and
require intensive therapy and monitoring. Patient
outcomes vary. A very high percentage of category C1
and C2 have normal outcomes. A significant portion of
C3 patients survive, but there is a substantial increase
in their incidence of death or survival with
anoxic-ischemic encephalopathy. C4 patients do
poorly. The majority die or survive with profound
anoxic-ischemic encephalopathy.
Note that all submersion victims may be apneic
when retrieved from the water since apnea is a
common reflex when the face is immersed in cold water
even if they have not sustained a cardiac arrest. Since
submersion victims with excellent prognosis may
initially be found apneic, vigorous initial resuscitation
measures should be attempted in all submersion
victims. Our patient was a Category A patient and did
quite well as predicted. The hypoxia was mild, and
neurologic functioning was good. Although she was felt
to have aspirated, antibiotics are reserved for proven
infection or when grossly contaminated water is
aspirated. For these reasons, this patient did not
receive antibiotics. She was observed for 24 hours, as
there may be a pulmonary inflammatory response
24-48 hours after the insult.
Immediate evaluation:
1. Consider: ABG, CBC, electrolytes, CXR.
2. Look for associated problems: head, neck, other
injuries; ingestion; possibility of a seizure (primary or
resulting from trauma, hypoxia, hyponatremia). Further
tests after stabilization to be considered are CT scan of
head, radiographs of the cervical spine, drug screen
(eg., alcohol).
Management - Category A:
1. Supplemental oxygen.
2. Aerosolized beta-adrenergic agents for wheezing
(albuterol).
3. Consider diuretic (furosemide) for pulmonary
edema seen on CXR.
4. Sodium bicarbonate. Give 1 meq/kg for pH 7.1
or less. As oxygenation improves, the acidosis will also
resolve.
5. Drying and warming measures.
6. Consider NG tube placement to prevent
aspiration and decompress the stomach. Excessive
stomach contents could elevate the diaphragm and
restrict thoracic volume.
Management - Category B:
1. The above measures plus:
2. Intubation usually is not needed.
3. Electrolyte disturbances: Hyponatremia may
occur if large amounts of fresh water are swallowed.
Hypernatremia may occur if salt water has been
swallowed.
4. Start an IV at maintenance or slightly less than
maintenance to prevent further pulmonary compromise.
5. Consider antibiotics for aspiration of
contaminated contents. Note that leukocytosis is a
common stress response and is not indicative of
infection.
Management - Category C:
1. Apply the above measures plus:
2. Intubate and ventilate, as all C patients are
comatose and have respiratory failure. High distending
pressures are usually required.
3. Monitor EKG for dysrhythmias. Hypotension
may also occur.
4. In addition to sodium abnormalities, hyperkalemia
from metabolic acidosis may occur.
5. Treat seizures (primary or from electrolyte
abnormalities, hypoxia, trauma).
6. Hyperglycemia is a stress response. There is
usually no need to treat this.
7. Leukocytosis, as mentioned, is an expected
stress response. Leukopenia can occur in profound
hypoxia. Consider antibiotics for aspiration of dirty
water.
Prevention
1. Educate caretakers to potential submersion risks
of bathtubs, water pails, pools, lakes, streams and the
ocean. Stress the need for close supervision by a
responsible adult.
2. Neighborhood and private swimming pools
should ideally be surrounded by a double barrier (eg.,
two sets of fences). If a single barrier is used to
surround the pool, the house should NOT be used as
part of the barrier.
3. Encourage swimming lessons for all patients.
However, water safety is not solely dependent on one's
ability to swim. An overall understanding of water
safety to avoid risk-taking behavior is necessary to
minimize risk. For example, a 9-year old who can swim
in a pool will easily drown in ocean surf or a rapidly
flowing stream.
4. Encourage caretakers to learn CPR
References
Aoki B. Evaluation, stabilization, and transportation
of the critically ill child. Mosby Yearbook, 1992,
pp.237-251.
Her chest radiograph is now normal.
Discussion
Drowning is defined as death within 24 hours as a
result of submersion. "Near drowning" refers to survival
beyond 24 hours of the submersion episode. The
majority of accidents occur in swimming pools, ponds,
lakes and bathtubs, with a peak incidence in children at
less than 4 years of age and a second peak during the
risk-taking age group of 15-24 years. Among boys
15-19 years, 38% of drownings are alcohol related.
Pathophysiologically, the problems commonly seen in a
submersion accident are:
1. Hypoxia
2. Hypothermia (EXCEPT when submersion occurs
in water greater than body temperature)
3. Aspiration (which can impair lung function and
aggravate existing hypoxia after breathing is restored)
Hypoxia is the primary problem. The clinical
manifestations of hypoxia are related to both the
severity of hypoxia and the differing abilities of
individual organs to tolerate hypoxia. The brain cortex
is the first to sustain irreversible damage. The lower
brain is next. The lungs and heart can tolerate up to
20-30 minutes of hypoxia and survive with appropriate
post-rescue support.
Hypothermia: This phenomenon explains the good
outcome of victims who are submerged in icy waters for
up to 45 minutes (and occasionally longer). When
submerged in icy cold water, the body temperature
drops rapidly to a point where body activity and
metabolism come to a virtual standstill. If this standstill
develops before available oxygen is completely used,
the hypothermia confers a protective effect. The
remaining oxygen is used slowly and the body can
survive submersion for a longer period of time before
irreversible anoxic tissue damage develops. In most
other instances, (non-icy water drowning), the victim's
temperature will drop too slowly to confer any protective
effect.
Aspiration: Experience indicates that saltwater and
freshwater aspiration do not produce significantly
different respiratory injury patterns. If large amounts
are swallowed, hypo or hypernatremia may result from
fresh or salt water submersions, respectively.
Respiratory infection is possible, but antibiotics should
be reserved for proven infection or when grossly
contaminated water is aspirated.
Clinical Manifestations
In the first moments after rescue, the appearance of
the child who has nearly drowned may range from
apparently normal to apparently dead. Body
temperature is frequently low, even in temperate,
warm-water environments. Respiratory efforts may be
absent, irregular, or labored, with pallor or cyanosis,
retractions, grunting, and cough productive of pink,
frothy material. The lungs may be clear, or there may
be rales, rhonchi and wheezing. Infection may develop
as a consequence of aspirated mouth flora or
organisms in stagnant water, but this is not usually
important in the first 24 hours.
Respiratory function may improve spontaneously or
deteriorate rapidly as pulmonary edema and small
airway dysfunction worsens.
Neurologic assessment may show an alert, normal
child or any level of CNS compromise. A child may
display agitation and combative behavior, seizures,
blunted responsiveness to the environment, or profound
coma with stereotypic posturing or flaccid extremities.
Superficial evidence of head trauma may be noted in a
few children whose submersion episode is a secondary
event.
Conn and Baker devised a classification of
submersion victims based on neurologic function since
the CNS is the system most susceptible to damage
from hypoxia. The classification is useful for 3 reasons:
1) it allows one to estimate the magnitude of the
hypoxic insult; 2) it guides one in the selection of
appropriate therapy; 3) it is highly predictive of patient
outcome.
They suggest the classification be made on patient
findings within the first hour of retrieval from water.
Patient classification by Conn and Baker divides the
patient into categories A,B,C1-4.
Category:
A: Awake = Alert, fully conscious, minimal injury
B: Blunted = Obtunded to stuporous, normal central
respiratory drive and other brain stem functions.
C: Comatose = Unarousable, abnormal brain stem
function, abnormal central respiratory pattern, abnormal
motor responses to painful stimuli. May have seizures.
Respiratory failure present. Category C patients may
be further subdivided:
C1: Decorticate. Flexor posturing. Cheyne-Stokes
respirations
C2: Decerebrate. Extensor posturing. Central
hyperventilation
C3: Flaccid. Apneustic or cluster breathing
C4: Deceased? Flaccid, apneic, no detectable
circulation
Prediction of submersion victim outcome can be
reduced to the following observation: If the victim has
not sustained a cardiac arrest, the potential for intact
survival is good when appropriate resuscitation and
prehospital care are provided.
Patients in categories A and B almost uniformly do
well with medical supportive therapy alone; intact
survival is the rule. A few category B patients develop
respiratory failure severe enough to require mechanical
ventilation, usually from aspiration.
Patients in category C are in respiratory failure and
require intensive therapy and monitoring. Patient
outcomes vary. A very high percentage of category C1
and C2 have normal outcomes. A significant portion of
C3 patients survive, but there is a substantial increase
in their incidence of death or survival with
anoxic-ischemic encephalopathy. C4 patients do
poorly. The majority die or survive with profound
anoxic-ischemic encephalopathy.
Note that all submersion victims may be apneic
when retrieved from the water since apnea is a
common reflex when the face is immersed in cold water
even if they have not sustained a cardiac arrest. Since
submersion victims with excellent prognosis may
initially be found apneic, vigorous initial resuscitation
measures should be attempted in all submersion
victims. Our patient was a Category A patient and did
quite well as predicted. The hypoxia was mild, and
neurologic functioning was good. Although she was felt
to have aspirated, antibiotics are reserved for proven
infection or when grossly contaminated water is
aspirated. For these reasons, this patient did not
receive antibiotics. She was observed for 24 hours, as
there may be a pulmonary inflammatory response
24-48 hours after the insult.
Immediate evaluation:
1. Consider: ABG, CBC, electrolytes, CXR.
2. Look for associated problems: head, neck, other
injuries; ingestion; possibility of a seizure (primary or
resulting from trauma, hypoxia, hyponatremia). Further
tests after stabilization to be considered are CT scan of
head, radiographs of the cervical spine, drug screen
(eg., alcohol).
Management - Category A:
1. Supplemental oxygen.
2. Aerosolized beta-adrenergic agents for wheezing
(albuterol).
3. Consider diuretic (furosemide) for pulmonary
edema seen on CXR.
4. Sodium bicarbonate. Give 1 meq/kg for pH 7.1
or less. As oxygenation improves, the acidosis will also
resolve.
5. Drying and warming measures.
6. Consider NG tube placement to prevent
aspiration and decompress the stomach. Excessive
stomach contents could elevate the diaphragm and
restrict thoracic volume.
Management - Category B:
1. The above measures plus:
2. Intubation usually is not needed.
3. Electrolyte disturbances: Hyponatremia may
occur if large amounts of fresh water are swallowed.
Hypernatremia may occur if salt water has been
swallowed.
4. Start an IV at maintenance or slightly less than
maintenance to prevent further pulmonary compromise.
5. Consider antibiotics for aspiration of
contaminated contents. Note that leukocytosis is a
common stress response and is not indicative of
infection.
Management - Category C:
1. Apply the above measures plus:
2. Intubate and ventilate, as all C patients are
comatose and have respiratory failure. High distending
pressures are usually required.
3. Monitor EKG for dysrhythmias. Hypotension
may also occur.
4. In addition to sodium abnormalities, hyperkalemia
from metabolic acidosis may occur.
5. Treat seizures (primary or from electrolyte
abnormalities, hypoxia, trauma).
6. Hyperglycemia is a stress response. There is
usually no need to treat this.
7. Leukocytosis, as mentioned, is an expected
stress response. Leukopenia can occur in profound
hypoxia. Consider antibiotics for aspiration of dirty
water.
Prevention
1. Educate caretakers to potential submersion risks
of bathtubs, water pails, pools, lakes, streams and the
ocean. Stress the need for close supervision by a
responsible adult.
2. Neighborhood and private swimming pools
should ideally be surrounded by a double barrier (eg.,
two sets of fences). If a single barrier is used to
surround the pool, the house should NOT be used as
part of the barrier.
3. Encourage swimming lessons for all patients.
However, water safety is not solely dependent on one's
ability to swim. An overall understanding of water
safety to avoid risk-taking behavior is necessary to
minimize risk. For example, a 9-year old who can swim
in a pool will easily drown in ocean surf or a rapidly
flowing stream.
4. Encourage caretakers to learn CPR
References
Aoki B. Evaluation, stabilization, and transportation
of the critically ill child. Mosby Yearbook, 1992,
pp.237-251.