Prolonged Cough and Fever
Radiology Cases in Pediatric Emergency Medicine
Volume 7, Case 3
Rachel O. Newton-Weaver, MD
Kapiolani Medical Center For Women And Children
University of Hawaii John A. Burns School of Medicine
This is a 5 year old, male who initially developed
fever (Tmax 40 degrees C) ten days ago along with
coughing, a sore throat and mild back pain. He was
seen at his health center seven days ago and a throat
culture was done at that time (eventually negative).
Over the next five days he continued to have fever and
cough. His mother noted him to have decreased
appetite, increased fatigue and shallow breathing. He
did not have any ill contacts, trauma, aspiration/choking
episodes or foreign travel. His past medical history is
negative. He has not had his 5 year old immunizations,
but he was up to date prior to this.
He presented to his primary care physician earlier
today at which time his vital signs were recorded as: T
37.5, P 120, RR 48, BP 100/56 and oxygen saturation
95-98% in room air. Although he does not appear to be
toxic or in obvious distress, he is making soft grunting
noises and has shallow respirations with diminished
breath sounds bilaterally.
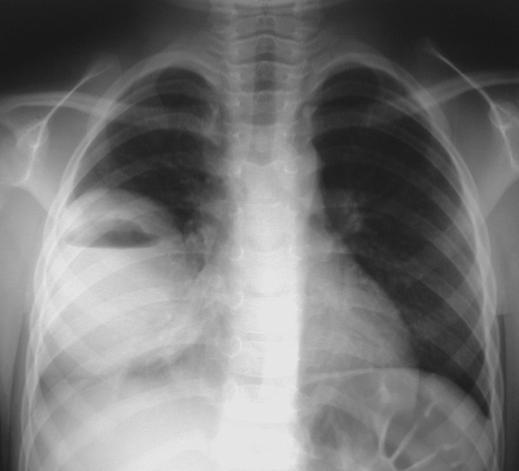
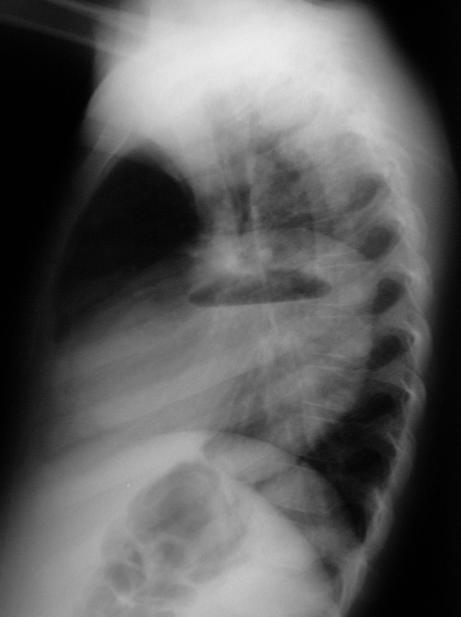
A chest radiograph is ordered.
View chest radiograph.
 Other lab studies done as an outpatient: CBC WBC
23,000, 73% segs, 10% bands, 11% lymphocytes and
6% monocytes, Hgb 10.6, Hct 31.2. ESR 56. His
chemistry panel is normal.
The chest radiograph demonstrates a large well
circumscribed consolidated lesion of the right middle
lobe with an air fluid level.
Arrangements for hospitalization at a children's
hospital are made. Upon admission, he develops
shaking chills with a temperature of 41 degrees C. VS
P 104, RR 52, BP 123/63 and oxygen saturation 96% in
room air. He is alert, cooperative and active with some
tachypnea and shallow respirations noted. He does not
appear to be toxic. Oral mucosa moist, without lesions
and no dental caries. Neck is supple without
lymphadenopathy. Heart regular without murmur.
Lung exam is significant for mild tachypnea, shallow
respirations, decreased breath sounds at both bases
(right > left). No rhonchi, rales, wheeze or retractions
are auscultated. Abdomen with normal bowel sounds,
no hepatosplenomegaly. Skin shows healing insect
bites on his lower legs with no impetiginous lesions
present.
A CT scan of the patient's chest confirms the
presence of a 8 x 6 x 8 cm thick walled mass in the
RML and RLL consistent with an abscess. He is
started empirically on clindamycin and cefotaxime.
Cultures of the abscess fluid isolate non-typable
Hemophilus influenzae (beta lactamase negative)
sensitive to ampicillin, cefotaxime, ciprofloxacin and
trimethoprim/sulfa. He was continued on clindamycin
and ampicillin. He became afebrile within 6 days of
starting intravenous antibiotics and remained so for the
rest of his hospital stay. After two weeks of IV
antibiotics, he was changed to oral amoxicillin to be
continued for another two weeks. His blood culture
remained negative.
Discussion
A lung abscess is defined as an area of necrotic
material within a thick walled cavity. The incidence,
morbidity and mortality of lung abscesses has fallen
due to improved antibiotic therapy and improved early
diagnostic capabilities. Overall, lung abscess remains
a relatively uncommon disease in the pediatric
population.
Pathogenesis
Risk factors for the development of a lung abscess
are aspiration, immunodeficiency and hematogenous
spread. Aspiration is the most important factor
predisposing a child to lung abscess (1). In children, a
lung abscess may also be a complication of a
necrotizing pneumonia. Aspiration occurs in children
with neurologic disorders, altered mental status,
impaired cough mechanisms, swallowing dysfunction or
even foreign body aspiration. Most lung abscesses
related to aspiration are polymicrobial and include
anaerobes. Hematogenous spread occurs with emboli,
right sided endocarditis and bacteremia.
Immunodeficiency in children occurs secondary to
myeloproliferative disorders, chemotherapy, chronic
granulomatous disease, hyper IgE syndrome, etc.
Among pediatric patients, HIV-1 infection has not been
reported as a risk factor (2). Additionally, immotile cilia
disorders and cystic fibrosis can increase the risk for a
lung abscess.
A lung abscess can have a well defined fibrotic wall
that may converge on adjacent structures causing
compression or dissection of the borders. Dissection
into a bronchus results in an air fluid level. Dissection
into the plural space forms a purulent effusion and if an
abscess dissects into the mediastinum, compression of
large vessels and the heart may occur.
Microbiology
The organisms associated with lung abscesses
have evolved as antibiotic therapy and our ability to
isolate organisms have improved. In normal children
with no known underlying disease, the most common
organisms are anaerobic bacteria, Staph aureus, Strep
pneumoniae and Strep pyogenes (group A strep). Gram
negative organisms include non-typable H. influenza,
Klebsiella and Pseudomonas. Anaerobic organisms are
the predominate organism isolated from children with
neurologic disorders (often due to aspiration) and
include Bacteroides and Peptostreptococcus.
Mycobacterium tuberculosis should also be considered.
Isolating organisms remains difficult. Bronchoscopy
is useful only if the abscess has ruptured. Direct
needle aspiration can be used if the abscess is near
the margins of the chest wall and this is aided with CT
and ultrasound guidance. Complications of this
recovery technique include pneumothorax, hemothorax
and empyema. Sputum is not reliable, especially if the
abscess has not ruptured, and it is also very difficult to
obtain in a child.
Signs and Symptoms
The most common clinical finding is fever.
Additional symptoms include cough (productive if the
abscess has ruptured and foul smelling sputum if the
organism is anaerobic), dyspnea, chest pain, shoulder
pain, anorexia and malaise. Acute onset of symptoms
is associated with bacterial organisms while subacute
presentations are typical in patients with tuberculosis
and fungal abscesses (2). The course of a lung
abscess before medical intervention may be
surprisingly indolent and may last several weeks (1).
On physical examination, findings are not always
consistent or specific, especially in children, but include
tachypnea, decreased breath sounds and rales.
Diagnosis
Chest radiographs usually reveal a well
circumscribed radiodense cavity with an air fluid level
that is confirmed with a lateral decubitus views. The
width of the air fluid level is usually of equal length on
both frontal and lateral chest radiographs, and its walls
are thick with an uneven shaggy appearance (3).
Atelectasis may be seen if the abscess compresses
nearby lung parenchyma. Initially the lung abscess
appears as a solid lesion within the parenchyma (5).
Computed tomography is useful in the diagnosis of a
lung abscess especially in cases where there may be
multiple or small abscesses, to differentiate an abscess
from a tumor, and to pinpoint the location of an abscess
in proximity to other structures. Classic findings on CT
include a thick ragged wall, central fluid and
surrounding parenchymal consolidation. Distinctive
features of a lung abscess are well marginated edges,
greater density of the abscess compared to water and
contrast enhancement in adjacent tissue (1).
Ultrasound examination shows a thick irregular wall
with a blurred outer margin and an oval or round shape
that forms an acute angle with the chest wall. However,
with ultrasound, a peripheral lung abscess may contain
low level echoes and thus can mimic a pleural effusion.
Voluntary hyperventilation causes symmetric movement
of the anterior and posterior walls of an abscess cavity,
while a pleural effusion causes asymmetric movement
(3).
The location of a lung abscess may be dependent
on the patient's position especially if aspiration is
involved. Supine position at time of aspiration
commonly results in an abscess located in the upper
lobes and apical aspects of the lower lobes, while the
erect position causes basilar portions of the upper
lobes to be affected. The right lung is usually affected
twice as often as the left because of the anatomic
position of the bronchus (4).
Blood cultures are positive in less than 10% of
cases (2). Leukocytosis and elevated ESR are
nonspecific. A PPD should be placed in all patients
suspected of lung abscess.
Differential Diagnosis
A lung abscess appearance on a chest radiograph
can be confused with a pneumatocele, infected
congenital cyst, loculated empyema, bronchopleural
fistula or pulmonary sequestration. Metastatic disease
from Ewing sarcoma or osteosarcoma can be
associated with pulmonary lesions with central
necrosis.
Treatment
The treatment of choice for lung abscess is
conservative medical management, with the length of
therapy dictated by the patient's clinical course and
documented radiographic improvement (4). In most
cases, the need for surgery is limited to cases of failed
antibiotic therapy or to an abscess complicated by
rupture into adjacent tissue (2).
Recommended antibiotic regimes include coverage
against both penicillinase producing Staph aureus and
anaerobes (5). If aspiration is suspected or the patient
is immunocompromised, there should be coverage for
gram negative organisms. Patients with cystic fibrosis
need coverage for Pseudomonas with an
anti-pseudomonal beta lactam (piperacillin or
ceftazidime) plus an aminoglycoside. Intravenous
antibiotic coverage should continue until the patient is
nontoxic and afebrile for 48-72 hours at which time oral
therapy may be considered (2). Two to three weeks of
antibiotic treatment are recommended.
Surgical intervention includes thoracentesis, guided
percutaneous needle aspiration and chest tube
thoracostomy (if the pleural space requires drainage)
which is recommended if antibiotic therapy fails, a large
abscess is present or for critically ill or deteriorating
patients. In extreme cases, wedge resection or
lobectomy may be needed.
Prognosis
The outcome for pediatric patients is usually very
good when lung abscesses are uncomplicated, and
recovery is more rapid than in adults (2). A study
focusing on follow-up of patients with primary
pulmonary abscess who received only antibiotics,
showed most of them to have normal pulmonary
function tests, normal growth and no other significant
lower respiratory tract disease (6). Chest radiographs
should be followed but complete resolution may take up
to 6 months.
References
1. Miller MA, Ben-Ami T, Daum RS. Bacterial
Pneumonia in Neonates and Older Children. In:
Taussig LM, Landau LI (eds). Pediatric Respiratory
Medicine, Mosby, St. Louis, 1999, pp. 644-647.
2. Wheeler JG, Jacobs RF. Lung Abscess. In:
Feigin RD, Cherry JD (eds). Textbook of Pediatric
Infectious Diseases, fourth edition. W.B. Saunders,
Philadelphia, 1998, pp. 301-307.
3. Sanford AR, Winer-Muram HT, Ellis JV.
Diagnostic imaging of pneumonia and its complications
in the critically ill patient. Clinics in Chest Medicine
1995;16(1):45-59.
4. Tan TQ, Seilheimer DK, Kaplan SL. Pediatric
lung abscess: Clinical management and outcome.
Pediatr Infec Dis J 1995;14(1):51-55.
5. Emanuel B, Shulman S. Lung Abscess in Infants
and Children. Clin Pediatr 1995,34(1):2-6.
6. Asher MI, Spier S, Beland M, Coates AL,
Beaudry PH. Primary lung abscess in childhood: The
long-term outcome of conservative management. Am J
Dis Child 1982;136:491-494.
Other lab studies done as an outpatient: CBC WBC
23,000, 73% segs, 10% bands, 11% lymphocytes and
6% monocytes, Hgb 10.6, Hct 31.2. ESR 56. His
chemistry panel is normal.
The chest radiograph demonstrates a large well
circumscribed consolidated lesion of the right middle
lobe with an air fluid level.
Arrangements for hospitalization at a children's
hospital are made. Upon admission, he develops
shaking chills with a temperature of 41 degrees C. VS
P 104, RR 52, BP 123/63 and oxygen saturation 96% in
room air. He is alert, cooperative and active with some
tachypnea and shallow respirations noted. He does not
appear to be toxic. Oral mucosa moist, without lesions
and no dental caries. Neck is supple without
lymphadenopathy. Heart regular without murmur.
Lung exam is significant for mild tachypnea, shallow
respirations, decreased breath sounds at both bases
(right > left). No rhonchi, rales, wheeze or retractions
are auscultated. Abdomen with normal bowel sounds,
no hepatosplenomegaly. Skin shows healing insect
bites on his lower legs with no impetiginous lesions
present.
A CT scan of the patient's chest confirms the
presence of a 8 x 6 x 8 cm thick walled mass in the
RML and RLL consistent with an abscess. He is
started empirically on clindamycin and cefotaxime.
Cultures of the abscess fluid isolate non-typable
Hemophilus influenzae (beta lactamase negative)
sensitive to ampicillin, cefotaxime, ciprofloxacin and
trimethoprim/sulfa. He was continued on clindamycin
and ampicillin. He became afebrile within 6 days of
starting intravenous antibiotics and remained so for the
rest of his hospital stay. After two weeks of IV
antibiotics, he was changed to oral amoxicillin to be
continued for another two weeks. His blood culture
remained negative.
Discussion
A lung abscess is defined as an area of necrotic
material within a thick walled cavity. The incidence,
morbidity and mortality of lung abscesses has fallen
due to improved antibiotic therapy and improved early
diagnostic capabilities. Overall, lung abscess remains
a relatively uncommon disease in the pediatric
population.
Pathogenesis
Risk factors for the development of a lung abscess
are aspiration, immunodeficiency and hematogenous
spread. Aspiration is the most important factor
predisposing a child to lung abscess (1). In children, a
lung abscess may also be a complication of a
necrotizing pneumonia. Aspiration occurs in children
with neurologic disorders, altered mental status,
impaired cough mechanisms, swallowing dysfunction or
even foreign body aspiration. Most lung abscesses
related to aspiration are polymicrobial and include
anaerobes. Hematogenous spread occurs with emboli,
right sided endocarditis and bacteremia.
Immunodeficiency in children occurs secondary to
myeloproliferative disorders, chemotherapy, chronic
granulomatous disease, hyper IgE syndrome, etc.
Among pediatric patients, HIV-1 infection has not been
reported as a risk factor (2). Additionally, immotile cilia
disorders and cystic fibrosis can increase the risk for a
lung abscess.
A lung abscess can have a well defined fibrotic wall
that may converge on adjacent structures causing
compression or dissection of the borders. Dissection
into a bronchus results in an air fluid level. Dissection
into the plural space forms a purulent effusion and if an
abscess dissects into the mediastinum, compression of
large vessels and the heart may occur.
Microbiology
The organisms associated with lung abscesses
have evolved as antibiotic therapy and our ability to
isolate organisms have improved. In normal children
with no known underlying disease, the most common
organisms are anaerobic bacteria, Staph aureus, Strep
pneumoniae and Strep pyogenes (group A strep). Gram
negative organisms include non-typable H. influenza,
Klebsiella and Pseudomonas. Anaerobic organisms are
the predominate organism isolated from children with
neurologic disorders (often due to aspiration) and
include Bacteroides and Peptostreptococcus.
Mycobacterium tuberculosis should also be considered.
Isolating organisms remains difficult. Bronchoscopy
is useful only if the abscess has ruptured. Direct
needle aspiration can be used if the abscess is near
the margins of the chest wall and this is aided with CT
and ultrasound guidance. Complications of this
recovery technique include pneumothorax, hemothorax
and empyema. Sputum is not reliable, especially if the
abscess has not ruptured, and it is also very difficult to
obtain in a child.
Signs and Symptoms
The most common clinical finding is fever.
Additional symptoms include cough (productive if the
abscess has ruptured and foul smelling sputum if the
organism is anaerobic), dyspnea, chest pain, shoulder
pain, anorexia and malaise. Acute onset of symptoms
is associated with bacterial organisms while subacute
presentations are typical in patients with tuberculosis
and fungal abscesses (2). The course of a lung
abscess before medical intervention may be
surprisingly indolent and may last several weeks (1).
On physical examination, findings are not always
consistent or specific, especially in children, but include
tachypnea, decreased breath sounds and rales.
Diagnosis
Chest radiographs usually reveal a well
circumscribed radiodense cavity with an air fluid level
that is confirmed with a lateral decubitus views. The
width of the air fluid level is usually of equal length on
both frontal and lateral chest radiographs, and its walls
are thick with an uneven shaggy appearance (3).
Atelectasis may be seen if the abscess compresses
nearby lung parenchyma. Initially the lung abscess
appears as a solid lesion within the parenchyma (5).
Computed tomography is useful in the diagnosis of a
lung abscess especially in cases where there may be
multiple or small abscesses, to differentiate an abscess
from a tumor, and to pinpoint the location of an abscess
in proximity to other structures. Classic findings on CT
include a thick ragged wall, central fluid and
surrounding parenchymal consolidation. Distinctive
features of a lung abscess are well marginated edges,
greater density of the abscess compared to water and
contrast enhancement in adjacent tissue (1).
Ultrasound examination shows a thick irregular wall
with a blurred outer margin and an oval or round shape
that forms an acute angle with the chest wall. However,
with ultrasound, a peripheral lung abscess may contain
low level echoes and thus can mimic a pleural effusion.
Voluntary hyperventilation causes symmetric movement
of the anterior and posterior walls of an abscess cavity,
while a pleural effusion causes asymmetric movement
(3).
The location of a lung abscess may be dependent
on the patient's position especially if aspiration is
involved. Supine position at time of aspiration
commonly results in an abscess located in the upper
lobes and apical aspects of the lower lobes, while the
erect position causes basilar portions of the upper
lobes to be affected. The right lung is usually affected
twice as often as the left because of the anatomic
position of the bronchus (4).
Blood cultures are positive in less than 10% of
cases (2). Leukocytosis and elevated ESR are
nonspecific. A PPD should be placed in all patients
suspected of lung abscess.
Differential Diagnosis
A lung abscess appearance on a chest radiograph
can be confused with a pneumatocele, infected
congenital cyst, loculated empyema, bronchopleural
fistula or pulmonary sequestration. Metastatic disease
from Ewing sarcoma or osteosarcoma can be
associated with pulmonary lesions with central
necrosis.
Treatment
The treatment of choice for lung abscess is
conservative medical management, with the length of
therapy dictated by the patient's clinical course and
documented radiographic improvement (4). In most
cases, the need for surgery is limited to cases of failed
antibiotic therapy or to an abscess complicated by
rupture into adjacent tissue (2).
Recommended antibiotic regimes include coverage
against both penicillinase producing Staph aureus and
anaerobes (5). If aspiration is suspected or the patient
is immunocompromised, there should be coverage for
gram negative organisms. Patients with cystic fibrosis
need coverage for Pseudomonas with an
anti-pseudomonal beta lactam (piperacillin or
ceftazidime) plus an aminoglycoside. Intravenous
antibiotic coverage should continue until the patient is
nontoxic and afebrile for 48-72 hours at which time oral
therapy may be considered (2). Two to three weeks of
antibiotic treatment are recommended.
Surgical intervention includes thoracentesis, guided
percutaneous needle aspiration and chest tube
thoracostomy (if the pleural space requires drainage)
which is recommended if antibiotic therapy fails, a large
abscess is present or for critically ill or deteriorating
patients. In extreme cases, wedge resection or
lobectomy may be needed.
Prognosis
The outcome for pediatric patients is usually very
good when lung abscesses are uncomplicated, and
recovery is more rapid than in adults (2). A study
focusing on follow-up of patients with primary
pulmonary abscess who received only antibiotics,
showed most of them to have normal pulmonary
function tests, normal growth and no other significant
lower respiratory tract disease (6). Chest radiographs
should be followed but complete resolution may take up
to 6 months.
References
1. Miller MA, Ben-Ami T, Daum RS. Bacterial
Pneumonia in Neonates and Older Children. In:
Taussig LM, Landau LI (eds). Pediatric Respiratory
Medicine, Mosby, St. Louis, 1999, pp. 644-647.
2. Wheeler JG, Jacobs RF. Lung Abscess. In:
Feigin RD, Cherry JD (eds). Textbook of Pediatric
Infectious Diseases, fourth edition. W.B. Saunders,
Philadelphia, 1998, pp. 301-307.
3. Sanford AR, Winer-Muram HT, Ellis JV.
Diagnostic imaging of pneumonia and its complications
in the critically ill patient. Clinics in Chest Medicine
1995;16(1):45-59.
4. Tan TQ, Seilheimer DK, Kaplan SL. Pediatric
lung abscess: Clinical management and outcome.
Pediatr Infec Dis J 1995;14(1):51-55.
5. Emanuel B, Shulman S. Lung Abscess in Infants
and Children. Clin Pediatr 1995,34(1):2-6.
6. Asher MI, Spier S, Beland M, Coates AL,
Beaudry PH. Primary lung abscess in childhood: The
long-term outcome of conservative management. Am J
Dis Child 1982;136:491-494.
Return to Radiology Cases In Ped Emerg Med Case Selection Page
Return to Univ. Hawaii Dept. Pediatrics Home Page

 Other lab studies done as an outpatient: CBC WBC
23,000, 73% segs, 10% bands, 11% lymphocytes and
6% monocytes, Hgb 10.6, Hct 31.2. ESR 56. His
chemistry panel is normal.
The chest radiograph demonstrates a large well
circumscribed consolidated lesion of the right middle
lobe with an air fluid level.
Arrangements for hospitalization at a children's
hospital are made. Upon admission, he develops
shaking chills with a temperature of 41 degrees C. VS
P 104, RR 52, BP 123/63 and oxygen saturation 96% in
room air. He is alert, cooperative and active with some
tachypnea and shallow respirations noted. He does not
appear to be toxic. Oral mucosa moist, without lesions
and no dental caries. Neck is supple without
lymphadenopathy. Heart regular without murmur.
Lung exam is significant for mild tachypnea, shallow
respirations, decreased breath sounds at both bases
(right > left). No rhonchi, rales, wheeze or retractions
are auscultated. Abdomen with normal bowel sounds,
no hepatosplenomegaly. Skin shows healing insect
bites on his lower legs with no impetiginous lesions
present.
A CT scan of the patient's chest confirms the
presence of a 8 x 6 x 8 cm thick walled mass in the
RML and RLL consistent with an abscess. He is
started empirically on clindamycin and cefotaxime.
Cultures of the abscess fluid isolate non-typable
Hemophilus influenzae (beta lactamase negative)
sensitive to ampicillin, cefotaxime, ciprofloxacin and
trimethoprim/sulfa. He was continued on clindamycin
and ampicillin. He became afebrile within 6 days of
starting intravenous antibiotics and remained so for the
rest of his hospital stay. After two weeks of IV
antibiotics, he was changed to oral amoxicillin to be
continued for another two weeks. His blood culture
remained negative.
Discussion
A lung abscess is defined as an area of necrotic
material within a thick walled cavity. The incidence,
morbidity and mortality of lung abscesses has fallen
due to improved antibiotic therapy and improved early
diagnostic capabilities. Overall, lung abscess remains
a relatively uncommon disease in the pediatric
population.
Pathogenesis
Risk factors for the development of a lung abscess
are aspiration, immunodeficiency and hematogenous
spread. Aspiration is the most important factor
predisposing a child to lung abscess (1). In children, a
lung abscess may also be a complication of a
necrotizing pneumonia. Aspiration occurs in children
with neurologic disorders, altered mental status,
impaired cough mechanisms, swallowing dysfunction or
even foreign body aspiration. Most lung abscesses
related to aspiration are polymicrobial and include
anaerobes. Hematogenous spread occurs with emboli,
right sided endocarditis and bacteremia.
Immunodeficiency in children occurs secondary to
myeloproliferative disorders, chemotherapy, chronic
granulomatous disease, hyper IgE syndrome, etc.
Among pediatric patients, HIV-1 infection has not been
reported as a risk factor (2). Additionally, immotile cilia
disorders and cystic fibrosis can increase the risk for a
lung abscess.
A lung abscess can have a well defined fibrotic wall
that may converge on adjacent structures causing
compression or dissection of the borders. Dissection
into a bronchus results in an air fluid level. Dissection
into the plural space forms a purulent effusion and if an
abscess dissects into the mediastinum, compression of
large vessels and the heart may occur.
Microbiology
The organisms associated with lung abscesses
have evolved as antibiotic therapy and our ability to
isolate organisms have improved. In normal children
with no known underlying disease, the most common
organisms are anaerobic bacteria, Staph aureus, Strep
pneumoniae and Strep pyogenes (group A strep). Gram
negative organisms include non-typable H. influenza,
Klebsiella and Pseudomonas. Anaerobic organisms are
the predominate organism isolated from children with
neurologic disorders (often due to aspiration) and
include Bacteroides and Peptostreptococcus.
Mycobacterium tuberculosis should also be considered.
Isolating organisms remains difficult. Bronchoscopy
is useful only if the abscess has ruptured. Direct
needle aspiration can be used if the abscess is near
the margins of the chest wall and this is aided with CT
and ultrasound guidance. Complications of this
recovery technique include pneumothorax, hemothorax
and empyema. Sputum is not reliable, especially if the
abscess has not ruptured, and it is also very difficult to
obtain in a child.
Signs and Symptoms
The most common clinical finding is fever.
Additional symptoms include cough (productive if the
abscess has ruptured and foul smelling sputum if the
organism is anaerobic), dyspnea, chest pain, shoulder
pain, anorexia and malaise. Acute onset of symptoms
is associated with bacterial organisms while subacute
presentations are typical in patients with tuberculosis
and fungal abscesses (2). The course of a lung
abscess before medical intervention may be
surprisingly indolent and may last several weeks (1).
On physical examination, findings are not always
consistent or specific, especially in children, but include
tachypnea, decreased breath sounds and rales.
Diagnosis
Chest radiographs usually reveal a well
circumscribed radiodense cavity with an air fluid level
that is confirmed with a lateral decubitus views. The
width of the air fluid level is usually of equal length on
both frontal and lateral chest radiographs, and its walls
are thick with an uneven shaggy appearance (3).
Atelectasis may be seen if the abscess compresses
nearby lung parenchyma. Initially the lung abscess
appears as a solid lesion within the parenchyma (5).
Computed tomography is useful in the diagnosis of a
lung abscess especially in cases where there may be
multiple or small abscesses, to differentiate an abscess
from a tumor, and to pinpoint the location of an abscess
in proximity to other structures. Classic findings on CT
include a thick ragged wall, central fluid and
surrounding parenchymal consolidation. Distinctive
features of a lung abscess are well marginated edges,
greater density of the abscess compared to water and
contrast enhancement in adjacent tissue (1).
Ultrasound examination shows a thick irregular wall
with a blurred outer margin and an oval or round shape
that forms an acute angle with the chest wall. However,
with ultrasound, a peripheral lung abscess may contain
low level echoes and thus can mimic a pleural effusion.
Voluntary hyperventilation causes symmetric movement
of the anterior and posterior walls of an abscess cavity,
while a pleural effusion causes asymmetric movement
(3).
The location of a lung abscess may be dependent
on the patient's position especially if aspiration is
involved. Supine position at time of aspiration
commonly results in an abscess located in the upper
lobes and apical aspects of the lower lobes, while the
erect position causes basilar portions of the upper
lobes to be affected. The right lung is usually affected
twice as often as the left because of the anatomic
position of the bronchus (4).
Blood cultures are positive in less than 10% of
cases (2). Leukocytosis and elevated ESR are
nonspecific. A PPD should be placed in all patients
suspected of lung abscess.
Differential Diagnosis
A lung abscess appearance on a chest radiograph
can be confused with a pneumatocele, infected
congenital cyst, loculated empyema, bronchopleural
fistula or pulmonary sequestration. Metastatic disease
from Ewing sarcoma or osteosarcoma can be
associated with pulmonary lesions with central
necrosis.
Treatment
The treatment of choice for lung abscess is
conservative medical management, with the length of
therapy dictated by the patient's clinical course and
documented radiographic improvement (4). In most
cases, the need for surgery is limited to cases of failed
antibiotic therapy or to an abscess complicated by
rupture into adjacent tissue (2).
Recommended antibiotic regimes include coverage
against both penicillinase producing Staph aureus and
anaerobes (5). If aspiration is suspected or the patient
is immunocompromised, there should be coverage for
gram negative organisms. Patients with cystic fibrosis
need coverage for Pseudomonas with an
anti-pseudomonal beta lactam (piperacillin or
ceftazidime) plus an aminoglycoside. Intravenous
antibiotic coverage should continue until the patient is
nontoxic and afebrile for 48-72 hours at which time oral
therapy may be considered (2). Two to three weeks of
antibiotic treatment are recommended.
Surgical intervention includes thoracentesis, guided
percutaneous needle aspiration and chest tube
thoracostomy (if the pleural space requires drainage)
which is recommended if antibiotic therapy fails, a large
abscess is present or for critically ill or deteriorating
patients. In extreme cases, wedge resection or
lobectomy may be needed.
Prognosis
The outcome for pediatric patients is usually very
good when lung abscesses are uncomplicated, and
recovery is more rapid than in adults (2). A study
focusing on follow-up of patients with primary
pulmonary abscess who received only antibiotics,
showed most of them to have normal pulmonary
function tests, normal growth and no other significant
lower respiratory tract disease (6). Chest radiographs
should be followed but complete resolution may take up
to 6 months.
References
1. Miller MA, Ben-Ami T, Daum RS. Bacterial
Pneumonia in Neonates and Older Children. In:
Taussig LM, Landau LI (eds). Pediatric Respiratory
Medicine, Mosby, St. Louis, 1999, pp. 644-647.
2. Wheeler JG, Jacobs RF. Lung Abscess. In:
Feigin RD, Cherry JD (eds). Textbook of Pediatric
Infectious Diseases, fourth edition. W.B. Saunders,
Philadelphia, 1998, pp. 301-307.
3. Sanford AR, Winer-Muram HT, Ellis JV.
Diagnostic imaging of pneumonia and its complications
in the critically ill patient. Clinics in Chest Medicine
1995;16(1):45-59.
4. Tan TQ, Seilheimer DK, Kaplan SL. Pediatric
lung abscess: Clinical management and outcome.
Pediatr Infec Dis J 1995;14(1):51-55.
5. Emanuel B, Shulman S. Lung Abscess in Infants
and Children. Clin Pediatr 1995,34(1):2-6.
6. Asher MI, Spier S, Beland M, Coates AL,
Beaudry PH. Primary lung abscess in childhood: The
long-term outcome of conservative management. Am J
Dis Child 1982;136:491-494.
Other lab studies done as an outpatient: CBC WBC
23,000, 73% segs, 10% bands, 11% lymphocytes and
6% monocytes, Hgb 10.6, Hct 31.2. ESR 56. His
chemistry panel is normal.
The chest radiograph demonstrates a large well
circumscribed consolidated lesion of the right middle
lobe with an air fluid level.
Arrangements for hospitalization at a children's
hospital are made. Upon admission, he develops
shaking chills with a temperature of 41 degrees C. VS
P 104, RR 52, BP 123/63 and oxygen saturation 96% in
room air. He is alert, cooperative and active with some
tachypnea and shallow respirations noted. He does not
appear to be toxic. Oral mucosa moist, without lesions
and no dental caries. Neck is supple without
lymphadenopathy. Heart regular without murmur.
Lung exam is significant for mild tachypnea, shallow
respirations, decreased breath sounds at both bases
(right > left). No rhonchi, rales, wheeze or retractions
are auscultated. Abdomen with normal bowel sounds,
no hepatosplenomegaly. Skin shows healing insect
bites on his lower legs with no impetiginous lesions
present.
A CT scan of the patient's chest confirms the
presence of a 8 x 6 x 8 cm thick walled mass in the
RML and RLL consistent with an abscess. He is
started empirically on clindamycin and cefotaxime.
Cultures of the abscess fluid isolate non-typable
Hemophilus influenzae (beta lactamase negative)
sensitive to ampicillin, cefotaxime, ciprofloxacin and
trimethoprim/sulfa. He was continued on clindamycin
and ampicillin. He became afebrile within 6 days of
starting intravenous antibiotics and remained so for the
rest of his hospital stay. After two weeks of IV
antibiotics, he was changed to oral amoxicillin to be
continued for another two weeks. His blood culture
remained negative.
Discussion
A lung abscess is defined as an area of necrotic
material within a thick walled cavity. The incidence,
morbidity and mortality of lung abscesses has fallen
due to improved antibiotic therapy and improved early
diagnostic capabilities. Overall, lung abscess remains
a relatively uncommon disease in the pediatric
population.
Pathogenesis
Risk factors for the development of a lung abscess
are aspiration, immunodeficiency and hematogenous
spread. Aspiration is the most important factor
predisposing a child to lung abscess (1). In children, a
lung abscess may also be a complication of a
necrotizing pneumonia. Aspiration occurs in children
with neurologic disorders, altered mental status,
impaired cough mechanisms, swallowing dysfunction or
even foreign body aspiration. Most lung abscesses
related to aspiration are polymicrobial and include
anaerobes. Hematogenous spread occurs with emboli,
right sided endocarditis and bacteremia.
Immunodeficiency in children occurs secondary to
myeloproliferative disorders, chemotherapy, chronic
granulomatous disease, hyper IgE syndrome, etc.
Among pediatric patients, HIV-1 infection has not been
reported as a risk factor (2). Additionally, immotile cilia
disorders and cystic fibrosis can increase the risk for a
lung abscess.
A lung abscess can have a well defined fibrotic wall
that may converge on adjacent structures causing
compression or dissection of the borders. Dissection
into a bronchus results in an air fluid level. Dissection
into the plural space forms a purulent effusion and if an
abscess dissects into the mediastinum, compression of
large vessels and the heart may occur.
Microbiology
The organisms associated with lung abscesses
have evolved as antibiotic therapy and our ability to
isolate organisms have improved. In normal children
with no known underlying disease, the most common
organisms are anaerobic bacteria, Staph aureus, Strep
pneumoniae and Strep pyogenes (group A strep). Gram
negative organisms include non-typable H. influenza,
Klebsiella and Pseudomonas. Anaerobic organisms are
the predominate organism isolated from children with
neurologic disorders (often due to aspiration) and
include Bacteroides and Peptostreptococcus.
Mycobacterium tuberculosis should also be considered.
Isolating organisms remains difficult. Bronchoscopy
is useful only if the abscess has ruptured. Direct
needle aspiration can be used if the abscess is near
the margins of the chest wall and this is aided with CT
and ultrasound guidance. Complications of this
recovery technique include pneumothorax, hemothorax
and empyema. Sputum is not reliable, especially if the
abscess has not ruptured, and it is also very difficult to
obtain in a child.
Signs and Symptoms
The most common clinical finding is fever.
Additional symptoms include cough (productive if the
abscess has ruptured and foul smelling sputum if the
organism is anaerobic), dyspnea, chest pain, shoulder
pain, anorexia and malaise. Acute onset of symptoms
is associated with bacterial organisms while subacute
presentations are typical in patients with tuberculosis
and fungal abscesses (2). The course of a lung
abscess before medical intervention may be
surprisingly indolent and may last several weeks (1).
On physical examination, findings are not always
consistent or specific, especially in children, but include
tachypnea, decreased breath sounds and rales.
Diagnosis
Chest radiographs usually reveal a well
circumscribed radiodense cavity with an air fluid level
that is confirmed with a lateral decubitus views. The
width of the air fluid level is usually of equal length on
both frontal and lateral chest radiographs, and its walls
are thick with an uneven shaggy appearance (3).
Atelectasis may be seen if the abscess compresses
nearby lung parenchyma. Initially the lung abscess
appears as a solid lesion within the parenchyma (5).
Computed tomography is useful in the diagnosis of a
lung abscess especially in cases where there may be
multiple or small abscesses, to differentiate an abscess
from a tumor, and to pinpoint the location of an abscess
in proximity to other structures. Classic findings on CT
include a thick ragged wall, central fluid and
surrounding parenchymal consolidation. Distinctive
features of a lung abscess are well marginated edges,
greater density of the abscess compared to water and
contrast enhancement in adjacent tissue (1).
Ultrasound examination shows a thick irregular wall
with a blurred outer margin and an oval or round shape
that forms an acute angle with the chest wall. However,
with ultrasound, a peripheral lung abscess may contain
low level echoes and thus can mimic a pleural effusion.
Voluntary hyperventilation causes symmetric movement
of the anterior and posterior walls of an abscess cavity,
while a pleural effusion causes asymmetric movement
(3).
The location of a lung abscess may be dependent
on the patient's position especially if aspiration is
involved. Supine position at time of aspiration
commonly results in an abscess located in the upper
lobes and apical aspects of the lower lobes, while the
erect position causes basilar portions of the upper
lobes to be affected. The right lung is usually affected
twice as often as the left because of the anatomic
position of the bronchus (4).
Blood cultures are positive in less than 10% of
cases (2). Leukocytosis and elevated ESR are
nonspecific. A PPD should be placed in all patients
suspected of lung abscess.
Differential Diagnosis
A lung abscess appearance on a chest radiograph
can be confused with a pneumatocele, infected
congenital cyst, loculated empyema, bronchopleural
fistula or pulmonary sequestration. Metastatic disease
from Ewing sarcoma or osteosarcoma can be
associated with pulmonary lesions with central
necrosis.
Treatment
The treatment of choice for lung abscess is
conservative medical management, with the length of
therapy dictated by the patient's clinical course and
documented radiographic improvement (4). In most
cases, the need for surgery is limited to cases of failed
antibiotic therapy or to an abscess complicated by
rupture into adjacent tissue (2).
Recommended antibiotic regimes include coverage
against both penicillinase producing Staph aureus and
anaerobes (5). If aspiration is suspected or the patient
is immunocompromised, there should be coverage for
gram negative organisms. Patients with cystic fibrosis
need coverage for Pseudomonas with an
anti-pseudomonal beta lactam (piperacillin or
ceftazidime) plus an aminoglycoside. Intravenous
antibiotic coverage should continue until the patient is
nontoxic and afebrile for 48-72 hours at which time oral
therapy may be considered (2). Two to three weeks of
antibiotic treatment are recommended.
Surgical intervention includes thoracentesis, guided
percutaneous needle aspiration and chest tube
thoracostomy (if the pleural space requires drainage)
which is recommended if antibiotic therapy fails, a large
abscess is present or for critically ill or deteriorating
patients. In extreme cases, wedge resection or
lobectomy may be needed.
Prognosis
The outcome for pediatric patients is usually very
good when lung abscesses are uncomplicated, and
recovery is more rapid than in adults (2). A study
focusing on follow-up of patients with primary
pulmonary abscess who received only antibiotics,
showed most of them to have normal pulmonary
function tests, normal growth and no other significant
lower respiratory tract disease (6). Chest radiographs
should be followed but complete resolution may take up
to 6 months.
References
1. Miller MA, Ben-Ami T, Daum RS. Bacterial
Pneumonia in Neonates and Older Children. In:
Taussig LM, Landau LI (eds). Pediatric Respiratory
Medicine, Mosby, St. Louis, 1999, pp. 644-647.
2. Wheeler JG, Jacobs RF. Lung Abscess. In:
Feigin RD, Cherry JD (eds). Textbook of Pediatric
Infectious Diseases, fourth edition. W.B. Saunders,
Philadelphia, 1998, pp. 301-307.
3. Sanford AR, Winer-Muram HT, Ellis JV.
Diagnostic imaging of pneumonia and its complications
in the critically ill patient. Clinics in Chest Medicine
1995;16(1):45-59.
4. Tan TQ, Seilheimer DK, Kaplan SL. Pediatric
lung abscess: Clinical management and outcome.
Pediatr Infec Dis J 1995;14(1):51-55.
5. Emanuel B, Shulman S. Lung Abscess in Infants
and Children. Clin Pediatr 1995,34(1):2-6.
6. Asher MI, Spier S, Beland M, Coates AL,
Beaudry PH. Primary lung abscess in childhood: The
long-term outcome of conservative management. Am J
Dis Child 1982;136:491-494.