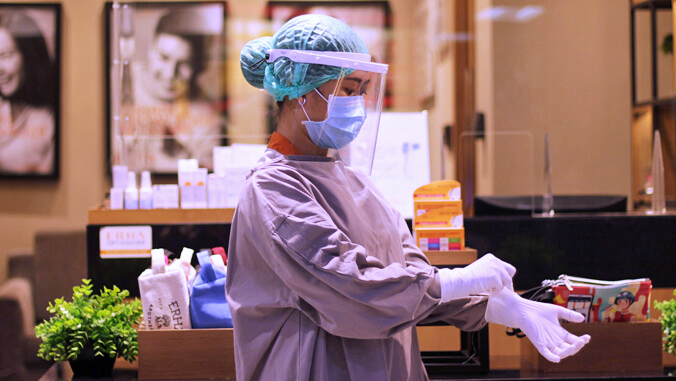
Hawaiʻi healthcare workers surveyed in 2020 were primarily concerned about contracting COVID-19 at work and transmitting it to their families, according to a recently published University of Hawaiʻi at Mānoa public health study. The survey was conducted between July and October 2020 by Anna D. Davide and Amelia R. Arechy, who earned their bachelor’s of arts degrees in public health in December 2020 and May 2021, respectively.
“As essential workers on the front lines of a pandemic, healthcare workers are unable to shelter-in-place, and to treat patients, often cannot obey physical distancing guidelines, making them highly exposed and vulnerable to infection,” said Davide.
According to national statistics, 93% of health care workers were experiencing stress in 2020, and 76% of healthcare workers with children reported that they were worried about exposing their families to COVID-19.
Davide added, “Despite this, we did not know about the impact of COVID-19 on the physical and emotional health of Hawaiʻi healthcare workers, or how healthcare workers in Hawaiʻi may have experienced the COVID-19 pandemic differently than those in less isolated geographic regions—this study worked to change that.”
The study also highlighted several findings of how the pandemic has affected the local healthcare community:
- Solo practitioners in outpatient clinics reported increased financial challenges and greater difficulty obtaining personal protective equipment than those employed by hospitals or group practices.
- Nearly all participants noted an increased use of telehealth options for healthcare access.
- Inequities in access to telehealth services among kūpuna (elders) and underserved populations, including those with poor internet connectivity and low technological literacy.
- Participants expressed worry that the new “forgiving” workplace attitudes that emerged from the pandemic would be diminished after the spread of COVID-19 subsides.
- Additional mental health support and resources from employers are needed.
Study methods
Data for the study was collected through qualitative interviews and demographic surveys. Davide and Arechy recruited two cohorts for the interview portion, which consisted of 15 participants in Cohort 1 (July–August) and 16 participants in Cohort 2 (September–October), all between the ages of 18–60+ years old. Seven themes were identified among the participants utilizing thematic analysis: 1) Emotional effects 2) Physical effects, 3) Workplace effects, 4) Telehealth and patient care, 5) Private practice challenges, 6) Mental health resources and 7) Regional attitude.
The demographic surveys were self-reported and included 28 physicians and three registered nurses. Participants were asked about their degree of worry about the COVID-19 pandemic, their overall wellbeing at the beginning of the pandemic, and their degree of worry at the time of the survey.
“I thought the most interesting finding was the increase in telehealth use among physicians and the perceived impact it would have in the future. It appears that the COVID-19 pandemic may have helped create a shift in medicine in Hawaiʻi by encouraging hospitals and clinics to provide virtual care and increase accessibility for patients,” said Arechy.
“I was proud of Ms. Arechy and Ms. Davide’s decision to use their undergraduate capstone project to contribute to our understanding of the pandemic’s impact on the health care community. Their work is an outstanding example of our students’ passion for public health,” said Opal V. Buchthal, assistant professor of public health.
Overall, available personal protective equipment, good communication and leadership from employers, and new information regarding best practices against COVID-19 contributed to health care workers’ sense of safety. The study’s findings help bring a better understanding on the effect of the pandemic on health care workers. Further research into the effects of COVID-19, specifically on nurses in Hawaiʻi, is recommended by the researchers.
Davide and Arechy’s co-authors on the paper also included Buchthal, and Professor Joseph Keaweʻaimoku Kaholokula and Assistant Professor Andrea H. Hermosura from the Department of Native Hawaiian Health at the John A. Burns School of Medicine.