An innovative technique to treat up to four COVID-19 patients with a single ventilator has the potential to save lives in Hawaiʻi and around the world.
The team working on the new method includes: University of Hawaiʻi at Mānoa Mechanical Engineering Associate Professors A Zachary Trimble and Scott Miller, Brennan Yamamoto, a 2019 UH Mānoa mechanical engineering PhD graduate and researcher for the University of Hawaiʻi Applied Research Laboratory, Russell Woo, MD, Kapiʻolani Medical Center for Women and Children pediatric surgeon and John A. Burns School of Medicine (JABSOM) associate professor of surgery, and the project’s founder, Donald Gaucher, MD, an anesthesiologist at Straub Medical Center.
“The quad-split ventilator system allows four patients to be ventilated off one ventilator, each with their own different minute ventilation,” Gaucher said.
Need for ventilators
Hawaiʻi Lt. Gov. Josh Green, who is also a medical doctor, said there are about 535 ventilators in the state and about 15 percent are currently in use. This new technique would be implemented only in an emergency if all ventilation capacity has been used. If needed, it would enable four times the number of patients to be treated.
“That’s a huge difference. Often, intensive care units are clustered so that you can get beds near one another. We have our Army Corp of Engineers also looking at some additional facilities, and those facilities will be designed with this kind of technology in mind so that if we did have to couple people onto a ventilator or bring people into close contact, this of course in a crisis circumstance, we could do it,” Green said.
“Currently with the coronavirus, we predict there will not be enough ventilators available in the United States,” Gaucher said.
How it works
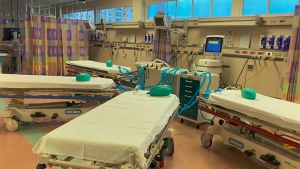
Researchers said doctors worldwide are already working on ways to treat more than one patient with a single ventilator. However, this advancement allows patients to receive more individualized care than simply just sharing the ventilator.
“This system works by using a series of flow and one-way valves, as well as some 3D-printed materials to individually regulate the flow and thereby the volume and pressures to each of the patients sharing the ventilator,” Woo said. “It allows for individualizing multiple elements of the respiratory care, which we feel will make this more safe and more feasible.”
One of the challenges researchers needed to overcome was to institute safety measures to prevent cross-contamination between patients.
“There are medical grade biofilters (a filter designed to remove 99.97 percent of airborne particles, including biomaterials like bacteria and viruses, measuring 0.3 micrometers or greater in diameter passing through it) in every patient limb in both the inspiration and expiration sides, and there are anti-backflow valves in both inspiration and expiration sides which limit the flow between patients. Thus, what limited flow that may be shared between patients is filtered,” Trimble said.
The team added that its technique allows doctors worldwide to make modifications because the shared ventilator system is sourced by parts they can find at local hardware stores.
Next steps
The team said it is conducting additional testing to improve the system before the need becomes critical in Hawaiʻi.
“This is not an approved use of the ventilator in an ideal situation. I will spend more time studying this system. However, time is of the essence,” Gaucher said.
“This solution, as any sharing solution, is only in an absolute emergency situation when all ventilation capacity has been used up, there’s no more ventilation capacity. So, if we need the ability to ventilate people, this would be an emergency solution,” Trimble said.
“I have a strong feeling that this department is in line for the department of the year award because of COVID-19 and it’s a pretty great thing to see. I’m really pleased,” Green said. “I like to see the partnership that will ensue from the perspective of engineering to JABSOM to, of course, the Healthcare Association of Hawaii. All these people, we’re able to bring them together.”
—By Marc Arakaki